Opening requested calculation...
Loading a bajillion calculations...
☠
0 people died of preventable disease while you waited
Abstract
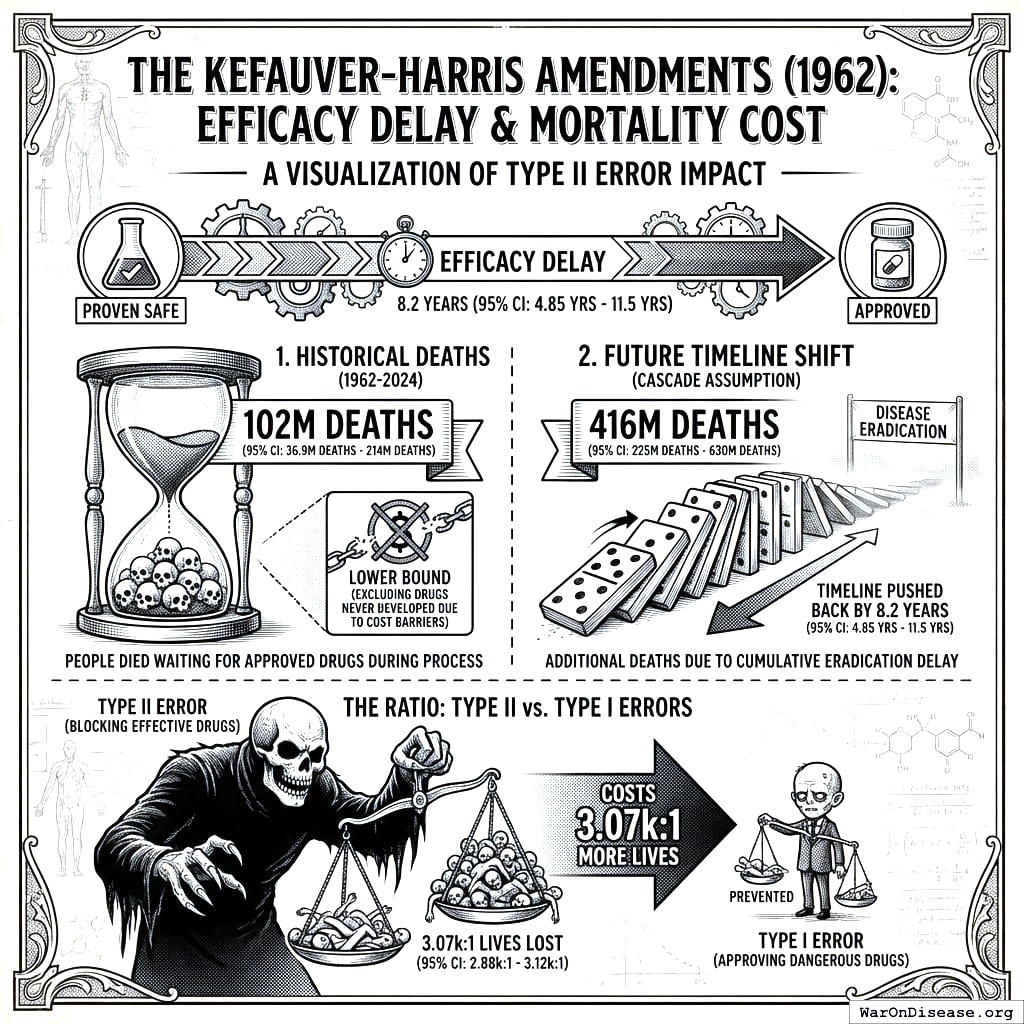
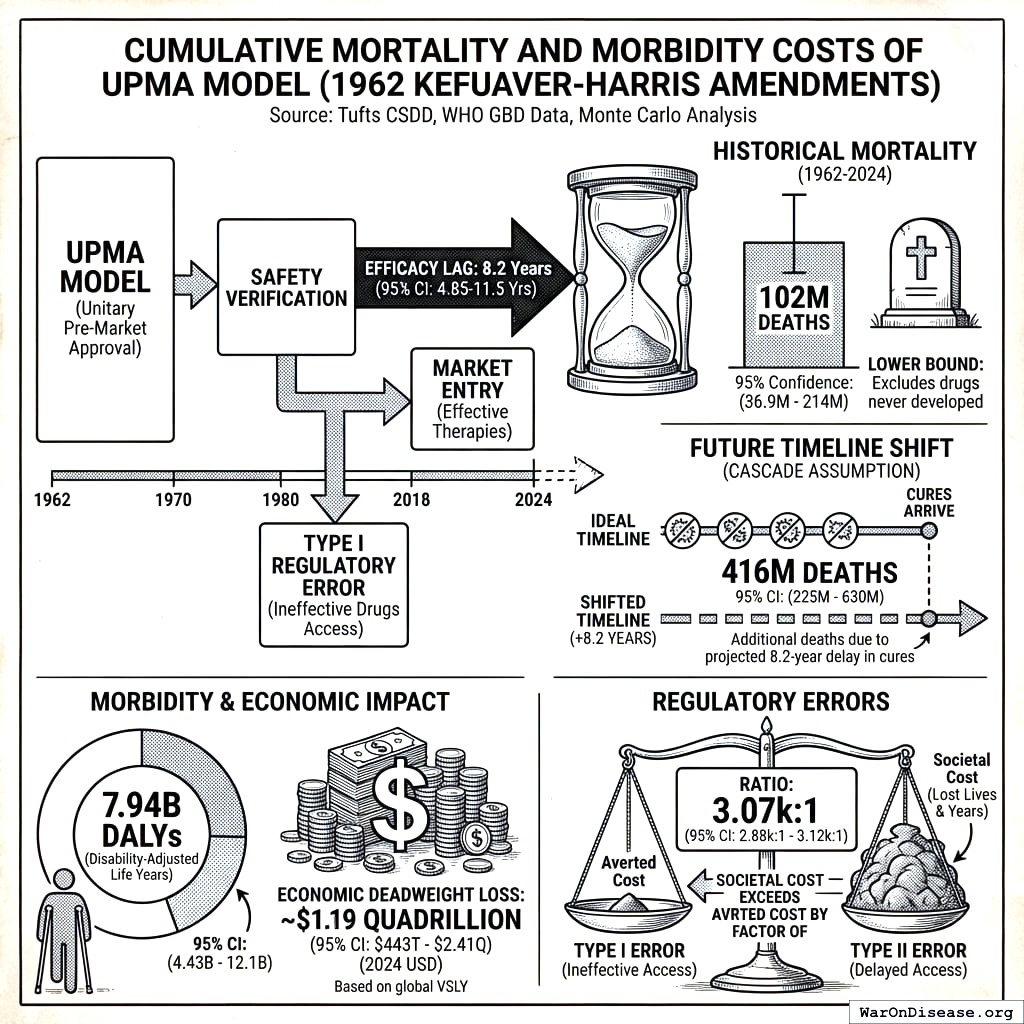
This study quantifies the cumulative mortality and morbidity costs associated with the Unitary Pre-Market Approval (UPMA) model mandated by the 1962 Kefauver-Harris Amendments. By enforcing efficacy testing prior to market entry, the current regulatory framework imposes an average “Efficacy Lag” of 8.2 years (95% CI: 4.85 years-11.5 years) post-safety verification.
Using data from the Tufts Center for the Study of Drug Development (CSDD) and the WHO Global Burden of Disease (GBD) database, we estimate two distinct mortality costs:
Historical mortality (1962-2024): Approximately 102 million people died waiting for approved drugs during their 8.2 years (95% CI: 4.85 years-11.5 years) approval delays. This is a lower bound - it excludes drugs never developed due to cost barriers.
Future timeline shift (under cascade assumption): An additional 416 million deaths (95% CI: 225 million deaths-630 million deaths) will eventually die because the entire disease eradication timeline has been pushed back by 8.2 years (95% CI: 4.85 years-11.5 years). When cures finally arrive, they arrive 8.2 years (95% CI: 4.85 years-11.5 years) later than they would have without efficacy requirements. During that delay, people die.
Historical Deaths Calculation:
\[
\begin{gathered}
Deaths_{lag,total} \\
= Lives_{saved,annual} \times T_{lag} \\
= 12.4M \times 8.2 \\
= 102M
\end{gathered}
\]
where:
\[
\begin{gathered}
Lives_{saved,annual} \\
= \frac{LY_{saved,annual}}{T_{ext}} \\
= \frac{149M}{12} \\
= 12.4M
\end{gathered}
\]
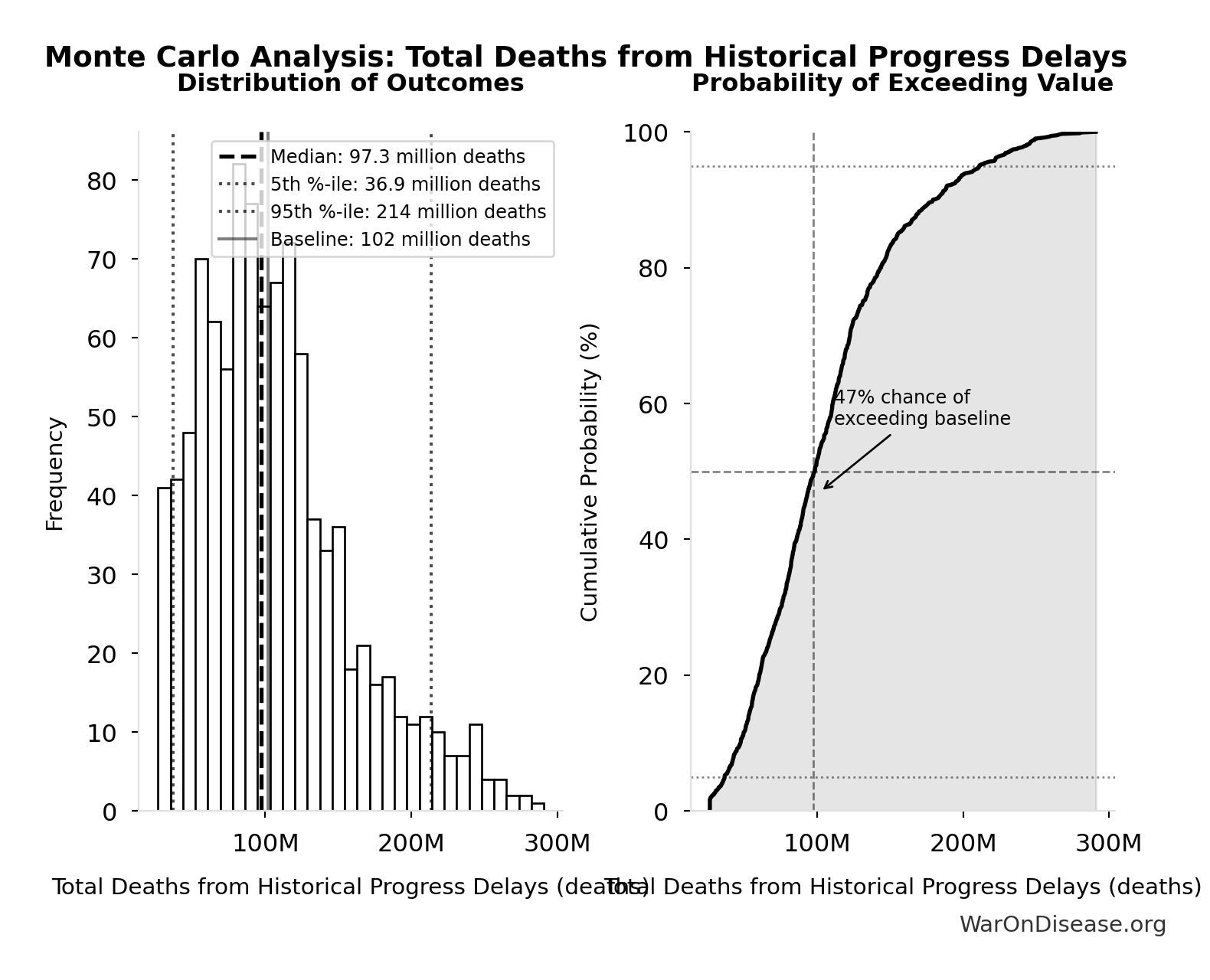
Simulation Results Summary: Total Deaths from Historical Progress Delays
| Baseline (deterministic) |
102 million |
| Mean (expected value) |
107 million |
| Median (50th percentile) |
97.3 million |
| Standard Deviation |
53 million |
| 90% Range (5th-95th percentile) |
[36.9 million, 214 million] |
The histogram shows the distribution of Total Deaths from Historical Progress Delays across 10,000 Monte Carlo simulations. The CDF (right) shows the probability of the outcome exceeding any given value, which is useful for risk assessment.
Combined, these represent 7.94 billion Disability-Adjusted Life Years (DALYs) when adjusted for morbidity. All estimates include Monte Carlo confidence intervals.
Valuing these lost years at a conservative global Value of a Statistical Life Year (VSLY) of $150,000 (95% CI: $100,000-$199,282)/DALY (the standard normative valuation used in WHO and health economics cost-effectiveness analyses), we find a cumulative economic deadweight loss of approximately $1.19 quadrillion (95% CI: $443 trillion-$2.41 quadrillion) (2024 USD). The study concludes that the societal cost of Type II Regulatory Errors (delayed access to effective therapies) exceeds the averted cost of Type I Regulatory Errors (market access for ineffective therapies) by a factor of 3,068 (95% CI: 2,878-3,125).
Scale
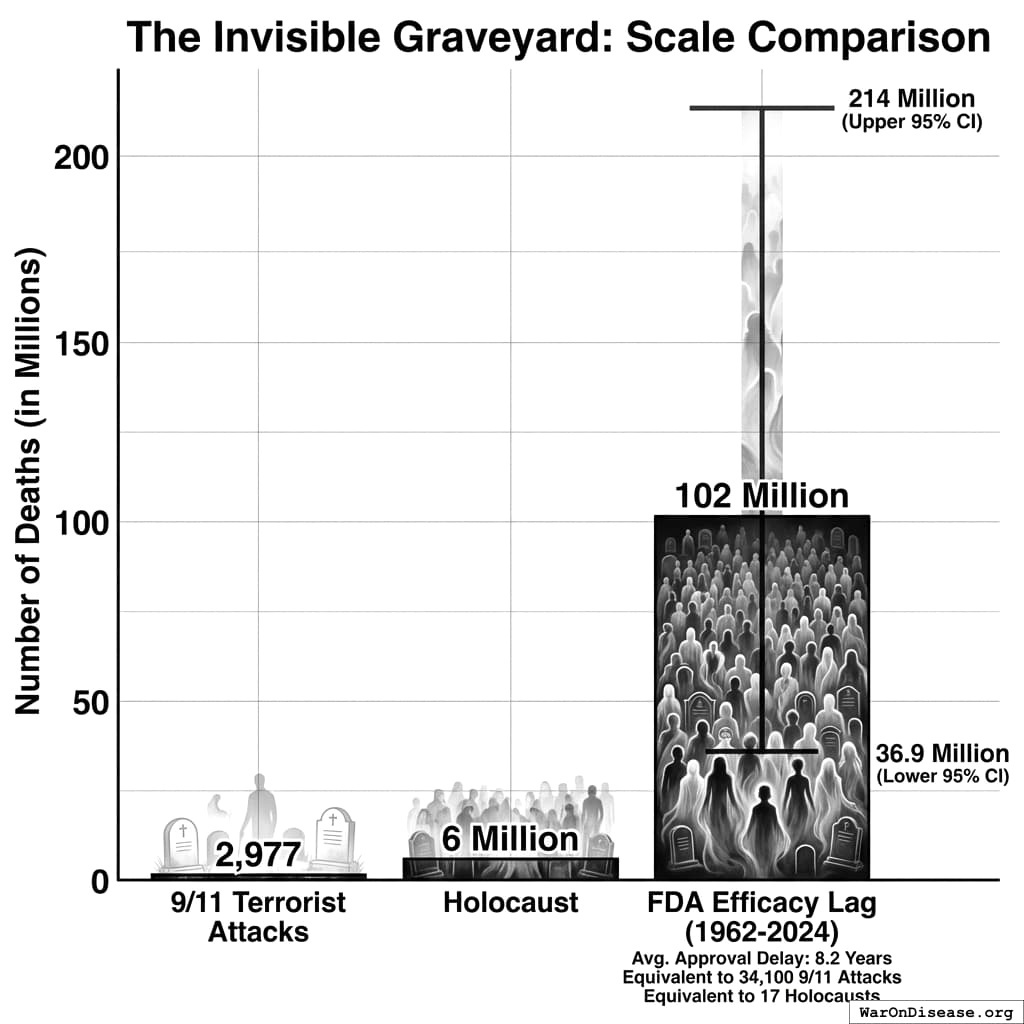
9/11: 2,977 people dead. We spent $8 trillion in response.
Holocaust: 6 million dead.
Efficacy lag: 102 million dead. That’s 34,132 9/11s (95% CI: 12,387 9/11s-71,845 9/11s), or 17 Holocausts.
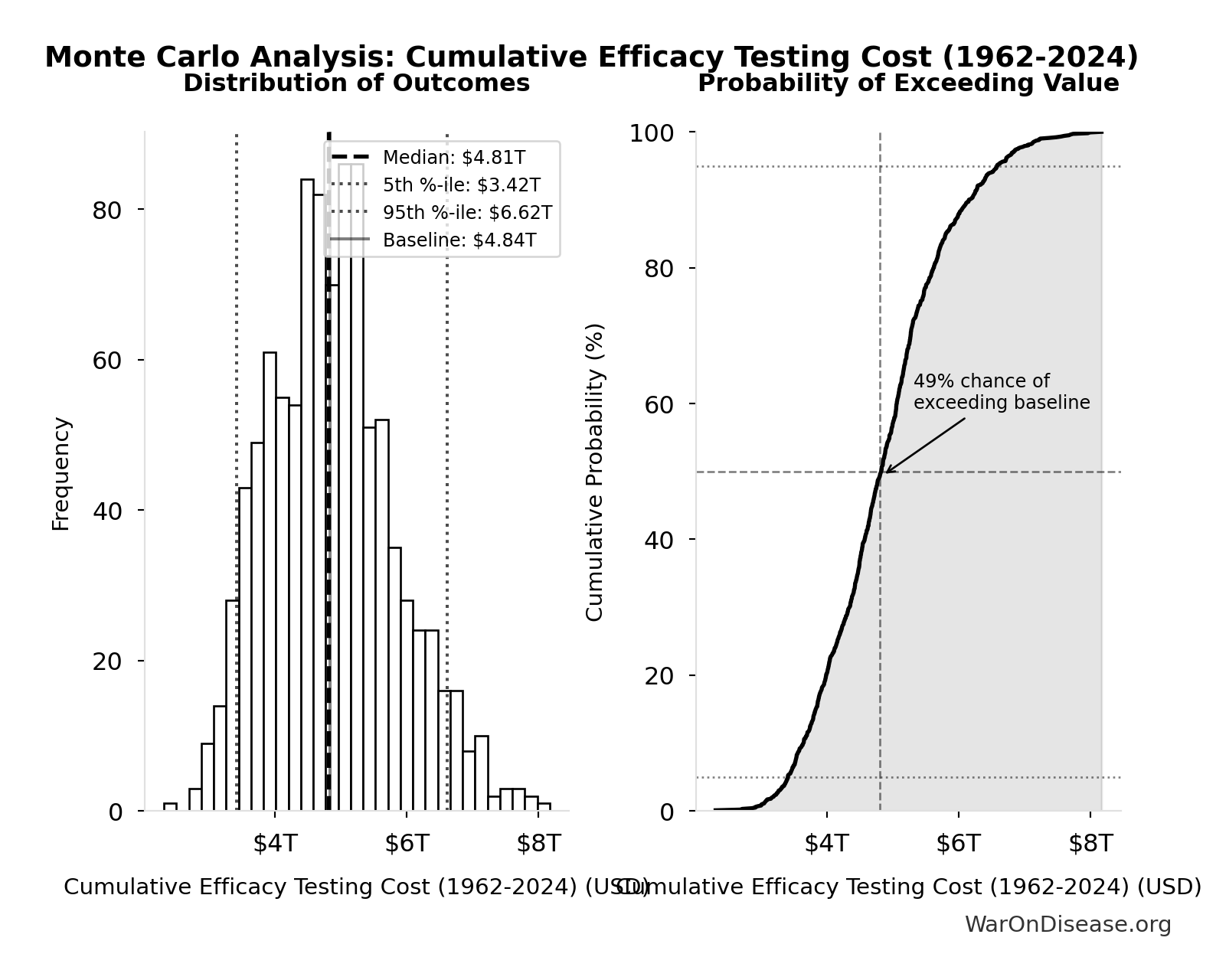
We paid $4.84 trillion (95% CI: $3.42 trillion-$6.62 trillion) (lower bound - Phase 2/3 costs only) to cause 34,132 9/11s (95% CI: 12,387 9/11s-71,845 9/11s).
Simulation Results Summary: Cumulative Efficacy Testing Cost (1962-2024)
| Baseline (deterministic) |
$4.84 trillion |
| Mean (expected value) |
$4.88 trillion |
| Median (50th percentile) |
$4.81 trillion |
| Standard Deviation |
$977 billion |
| 90% Range (5th-95th percentile) |
[$3.42 trillion, $6.62 trillion] |
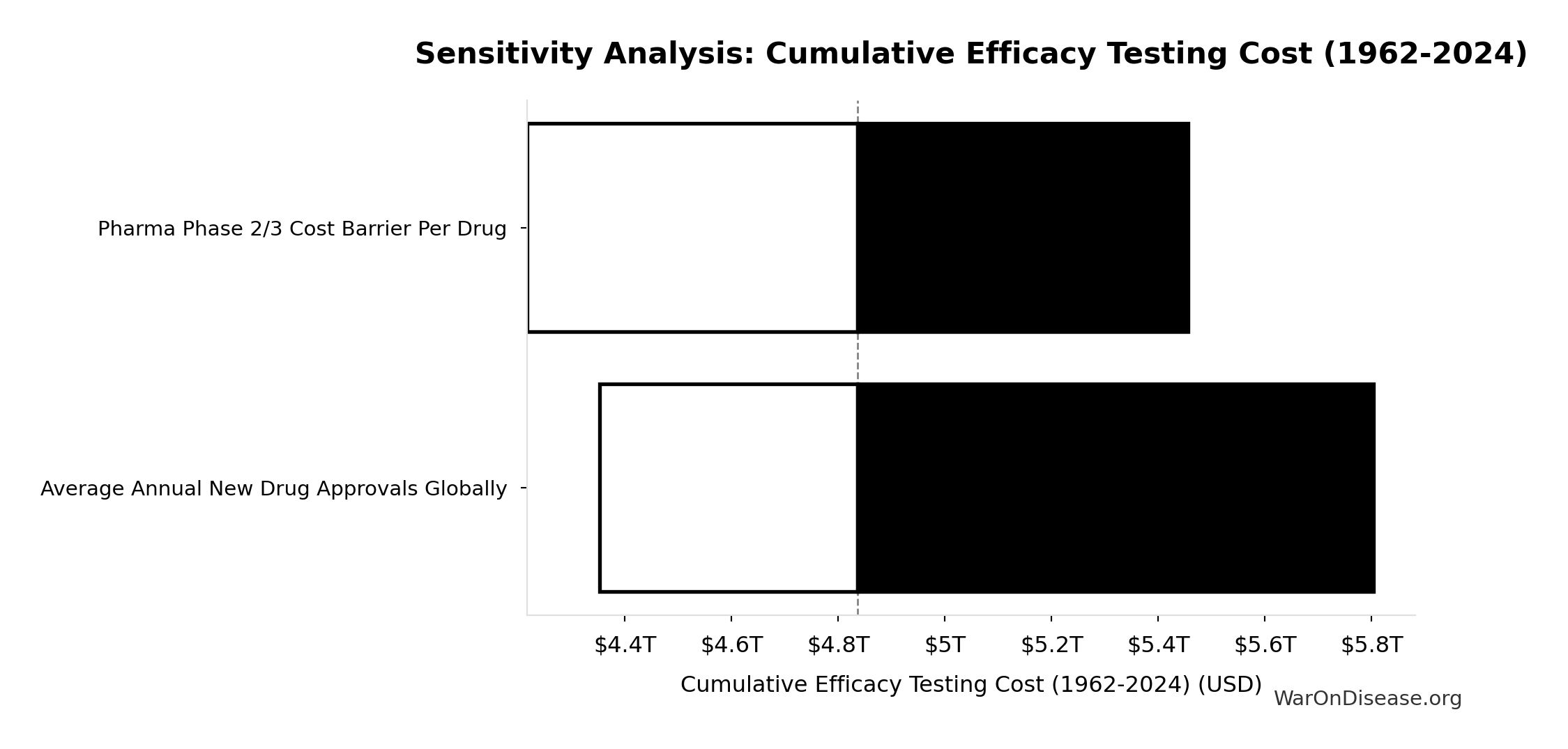
The histogram shows the distribution of Cumulative Efficacy Testing Cost (1962-2024) across 10,000 Monte Carlo simulations. The CDF (right) shows the probability of the outcome exceeding any given value, which is useful for risk assessment.
That’s $1.56 billion (95% CI: $1.23 billion-$1.89 billion) per drug for Phase 2/3 efficacy trials, paid by patients through higher drug prices. Before 1962, the AMA’s 144 thousand physicians tracked patient outcomes and JAMA published the results. We replaced that with tiny trials on handpicked patients.
Without mandatory pre-market trials, the market wouldn’t be blind. Knowing whether drugs work is one of the highest consumer demands imaginable. Organizations like Consumer Reports, JAMA, and independent research institutes would compete to provide rigorous, large-scale efficacy data - with no pharma conflicts of interest, across real-world populations, with ongoing monitoring instead of a pre-approval snapshot.
These are underestimates. They only count delays to drugs that got developed. The $2.6 billion (95% CI: $1.5 billion-$4 billion) approval cost killed other drugs before they started. We can’t count deaths prevented by cures that don’t exist.
\[
\begin{gathered}
N_{9/11,equiv} \\
= \frac{Deaths_{lag,total}}{N_{9/11}} \\
= \frac{102M}{2{,}980} \\
= 34{,}100
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag,total} \\
= Lives_{saved,annual} \times T_{lag} \\
= 12.4M \times 8.2 \\
= 102M
\end{gathered}
\]
where:
\[
\begin{gathered}
Lives_{saved,annual} \\
= \frac{LY_{saved,annual}}{T_{ext}} \\
= \frac{149M}{12} \\
= 12.4M
\end{gathered}
\]
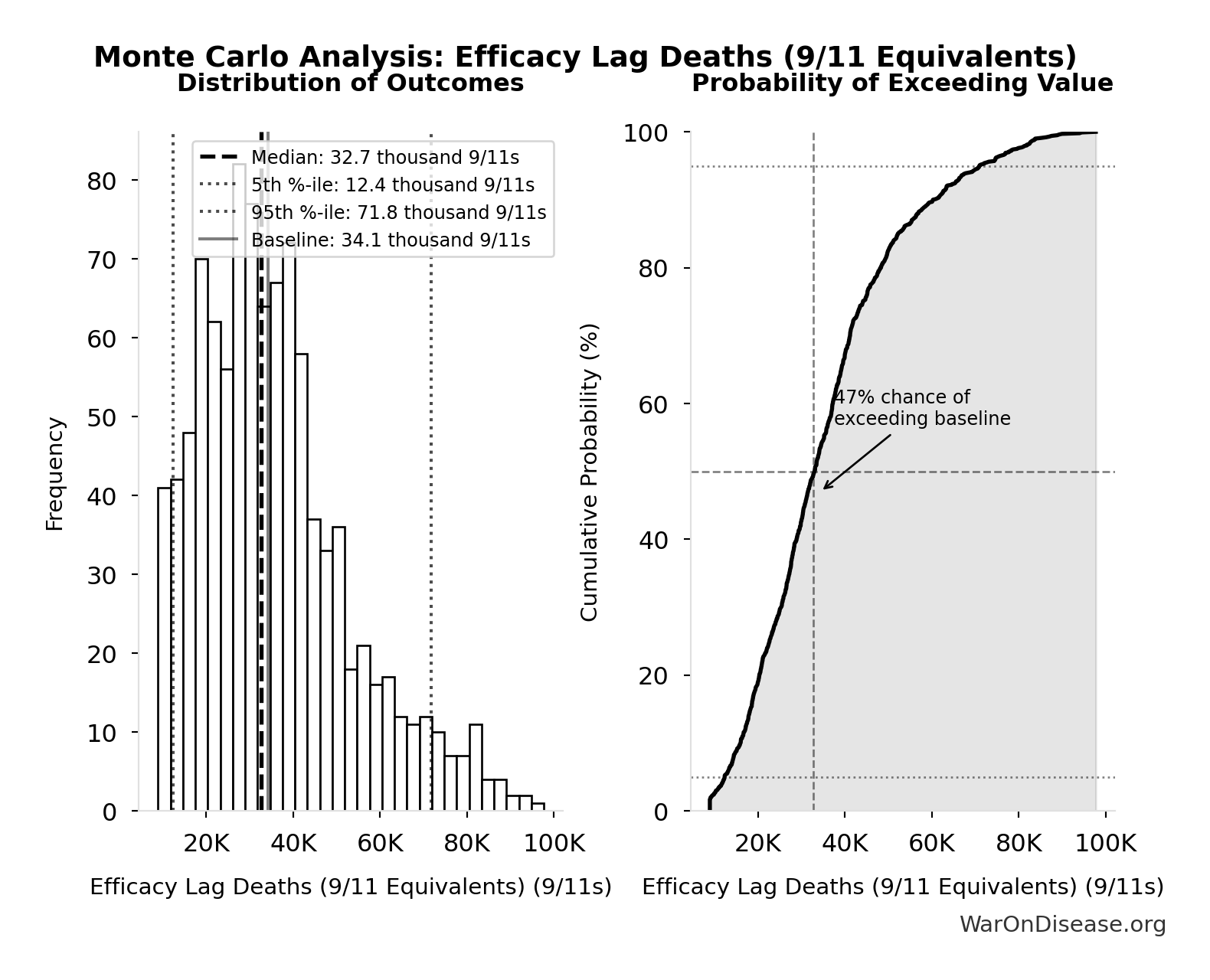
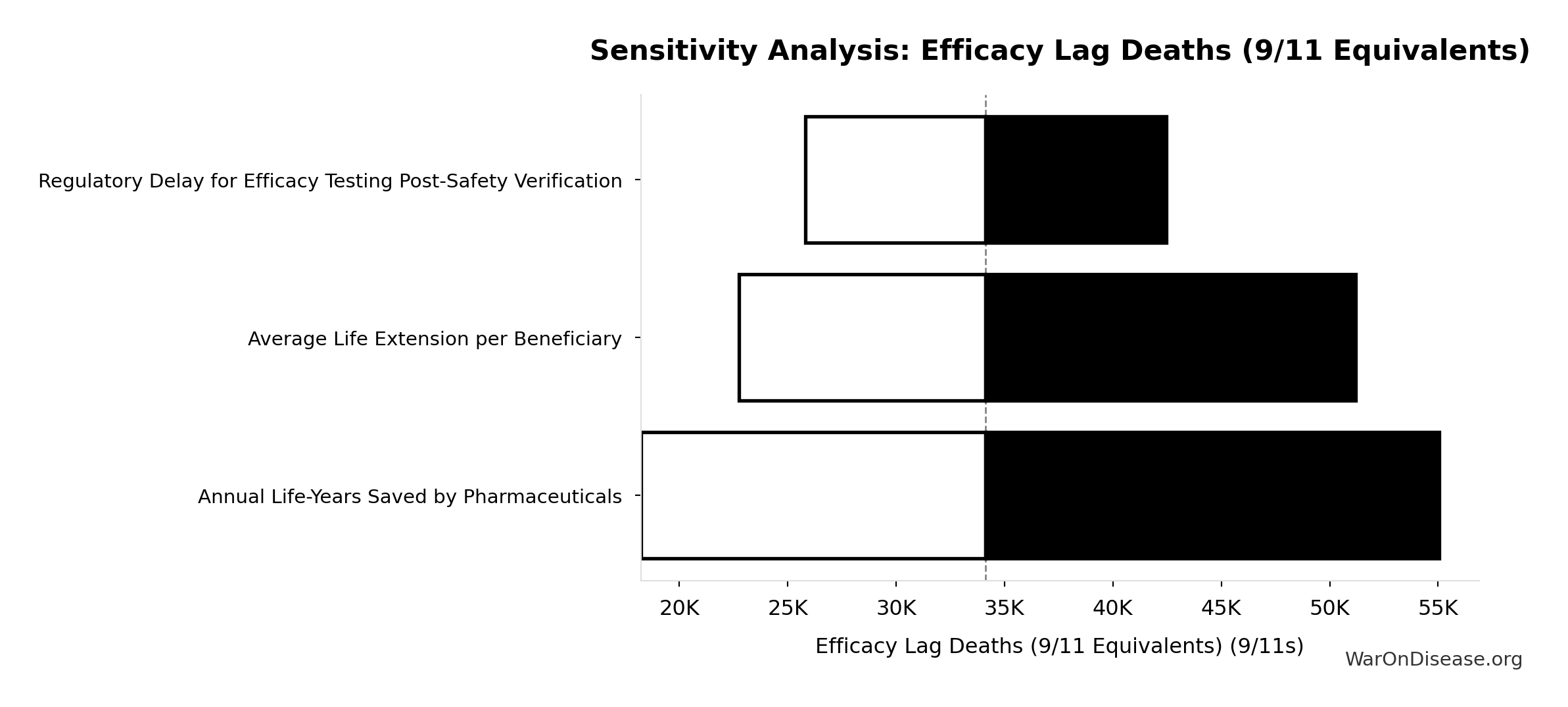
Simulation Results Summary: Efficacy Lag Deaths (9/11 Equivalents)
| Baseline (deterministic) |
34,132 |
| Mean (expected value) |
35,973 |
| Median (50th percentile) |
32,687 |
| Standard Deviation |
17,792 |
| 90% Range (5th-95th percentile) |
[12,387, 71,845] |
The histogram shows the distribution of Efficacy Lag Deaths (9/11 Equivalents) across 10,000 Monte Carlo simulations. The CDF (right) shows the probability of the outcome exceeding any given value, which is useful for risk assessment.
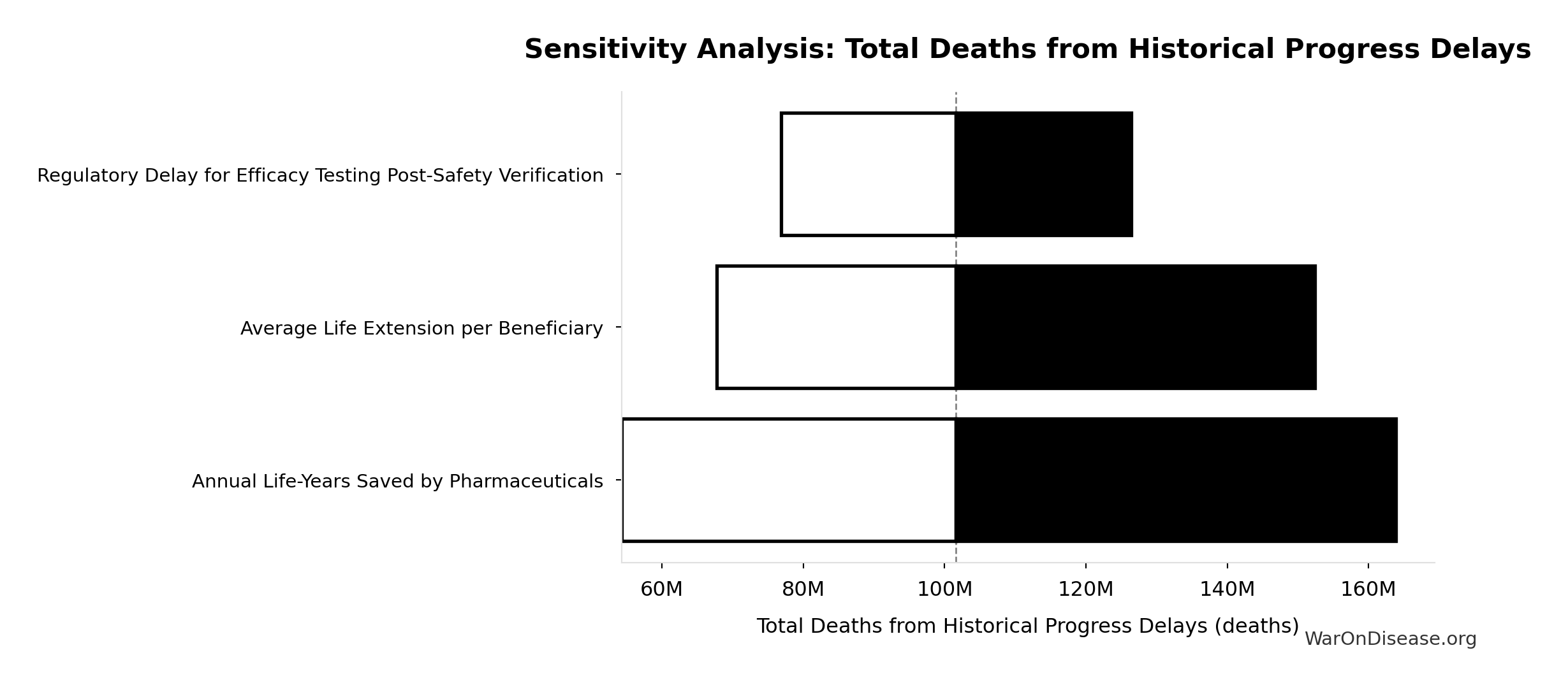
Sensitivity Indices for Efficacy Lag Deaths (9/11 Equivalents)
Regression-based sensitivity showing which inputs explain the most variance in the output.
| Total Deaths from Historical Progress Delays (deaths) |
1.0000 |
Strong driver |
Interpretation: Standardized coefficients show the change in output (in SD units) per 1 SD change in input. Values near ±1 indicate strong influence; values exceeding ±1 may occur with correlated inputs.
Introduction
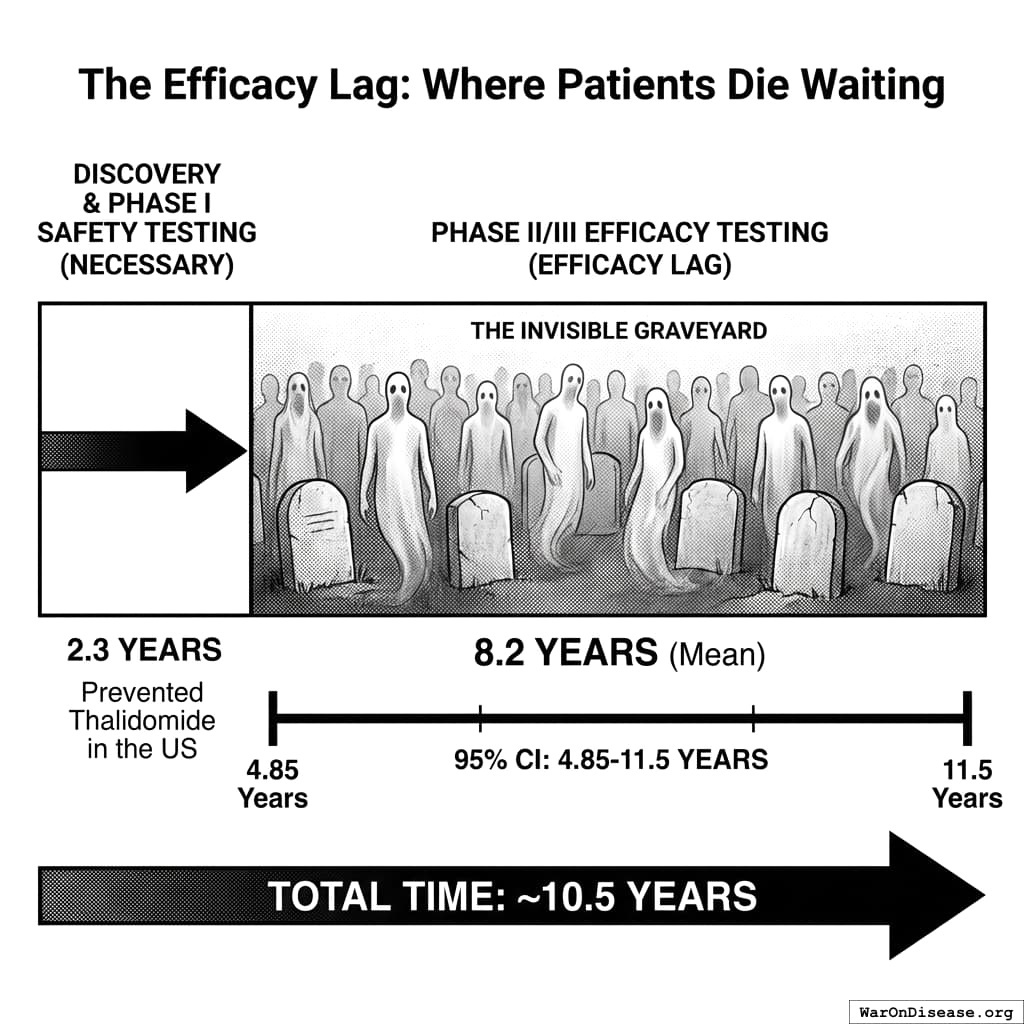
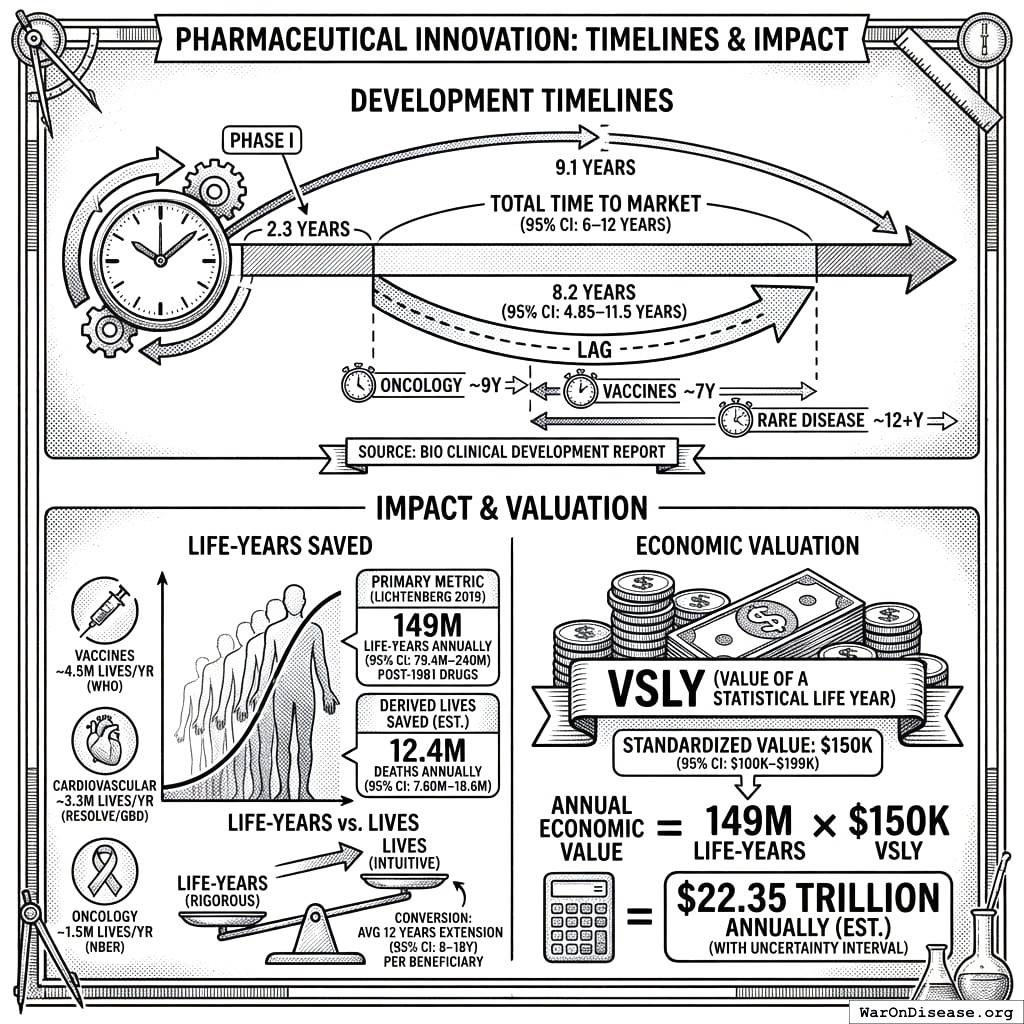
The modern pharmaceutical regulatory paradigm relies on a binary licensure model: a drug is either “safe and effective” (approved) or “unsafe/ineffective” (prohibited). While Phase I trials typically establish safety within 2.3 years, the requirement to prove statistical efficacy (Phase II/III) extends the pre-market timeline by an additional 8.2 years (95% CI: 4.85 years-11.5 years) on average.
This study evaluates the Bifurcated Regulatory Model (BRM), defined as “Safety-First / Efficacy-Later”, to measure the “Invisible Graveyard”: the population that dies during the regulatory latency period between safety verification and final approval.
Literature Review: The Drug Lag Debate
Foundational Economic Analysis
The regulatory cost of FDA efficacy requirements was first rigorously quantified by Peltzman148, who estimated that the 1962 Kefauver-Harris Amendments reduced the flow of new drugs by 50-60%. His analysis concluded that the costs of reduced pharmaceutical innovation substantially exceeded any benefits from keeping ineffective drugs off the market, resulting in net welfare losses to society.
Wardell149 documented the emerging “drug lag” between US and UK drug approvals, finding that the UK had access to significantly more new therapeutic agents. His estimate that beta-blockers alone could save 10,000 American lives annually if approved became a landmark finding in regulatory economics.
Gieringer150 synthesized these estimates, calculating 21,000-120,000 lives lost per decade from FDA delay. His work documented specific drug delays: propranolol (approved in the US 3 years after Europe for cardiac use, 10 years later for hypertension), interleukin-2 (7-year gap), and numerous other therapeutics.
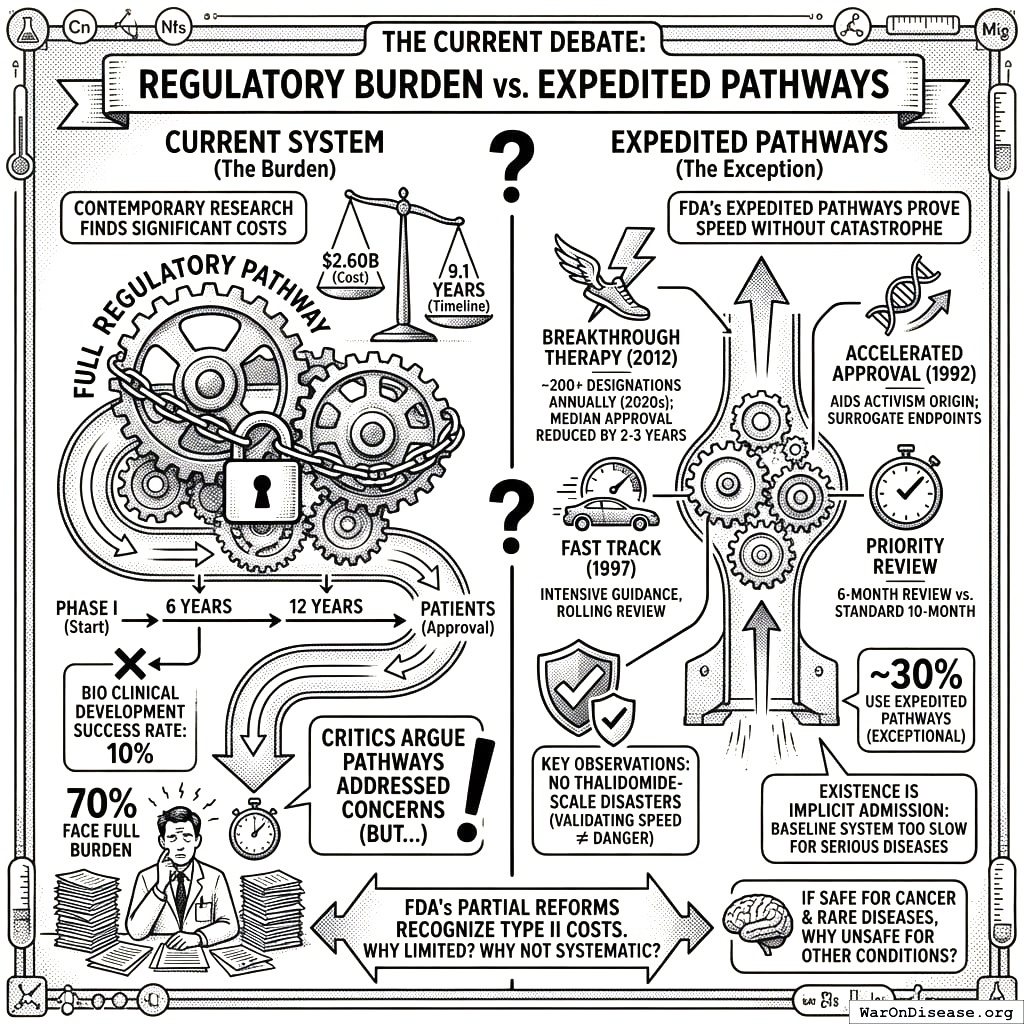
The Current Debate
Contemporary research continues to find significant regulatory costs. The Tufts Center for the Study of Drug Development documents development timelines of 10.5 years (95% CI: 6 years-12 years) and costs of $2.6 billion (95% CI: $1.5 billion-$4 billion) per approved drug. BIO’s clinical development success rates show only 10% of drugs entering Phase I ultimately reach patients.
Critics argue that faster approval pathways (breakthrough therapy designation, accelerated approval) have addressed these concerns. However, these pathways actually support our argument:
FDA’s Expedited Pathways Prove Speed is Possible Without Catastrophe:
- Breakthrough Therapy Designation (2012): ~200+ designations annually by 2020s, median approval time reduced by 2-3 years for qualifying drugs
- Accelerated Approval (1992): Born from AIDS activism; allows approval based on surrogate endpoints
- Fast Track (1997): Intensive FDA guidance and rolling review
- Priority Review: 6-month review vs. standard 10-month
Key observations:
- These pathways have NOT produced Thalidomide-scale disasters, validating that speed ≠ danger
- They remain exceptional rather than default: ~30% of approvals use expedited pathways; 70% face full regulatory burden
- Their existence is an implicit admission that the baseline system is too slow for serious diseases
- If expedited pathways are safe for cancer and rare diseases, why are they unsafe for other conditions?
The FDA’s partial reforms prove the system recognizes Type II costs exist. The question is why the recognition is limited to a subset of diseases rather than systematically applied.
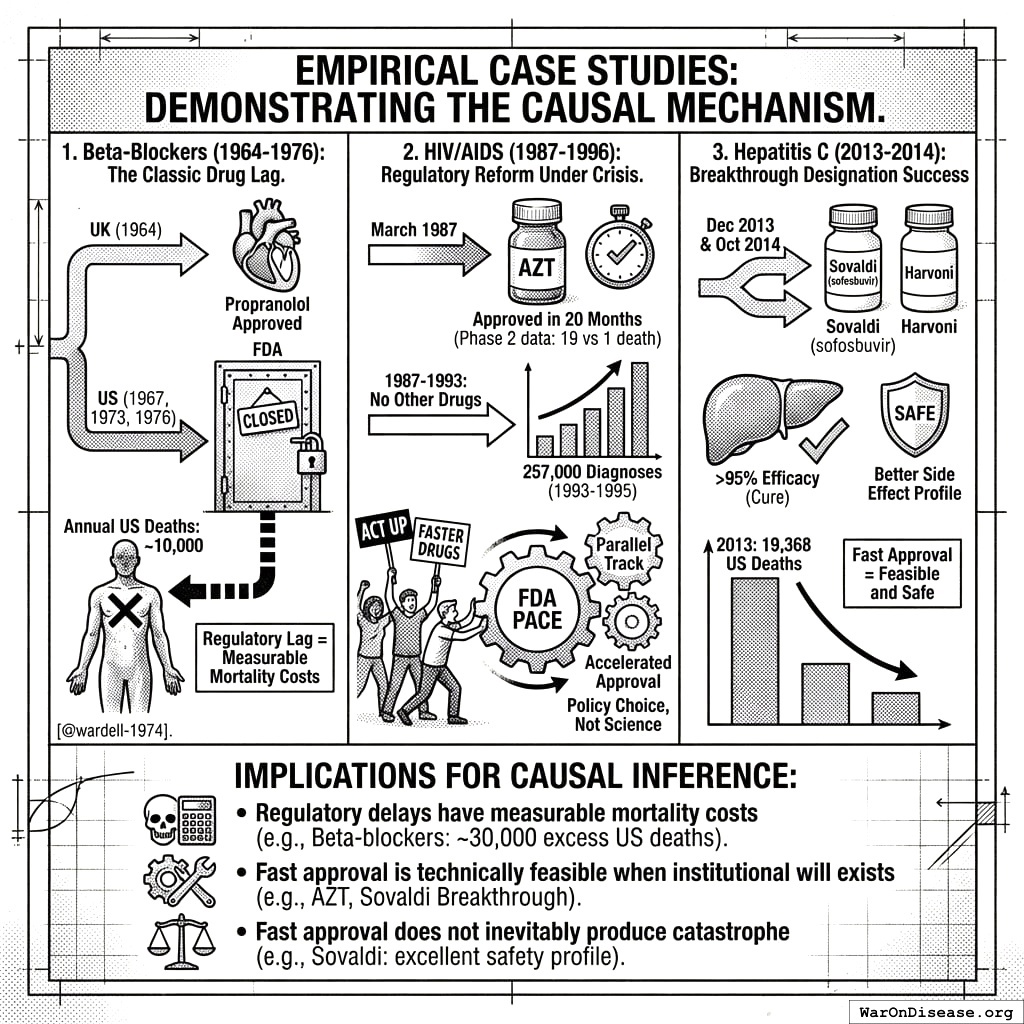
Empirical Case Studies: Demonstrating the Causal Mechanism
The theoretical claim that regulatory delay causes mortality requires empirical grounding. Three case studies demonstrate the mechanism operates in practice:
1. Beta-Blockers (1964-1976): The Classic Drug Lag
Propranolol, the first beta-blocker for treating angina and hypertension, was approved in the UK in 1964. US approval came in 1967 for minor uses, but not until 1973 (angina) and 1976 (hypertension) for cardiovascular indications. Wardell estimated approximately 10,000 Americans died annually during this delay, as the FDA’s doors were “essentially closed to cardiovascular drugs for an entire decade”149. This single drug’s regulatory lag may have caused more American deaths than all other drug-related deaths in that century.
2. HIV/AIDS (1987-1996): Regulatory Reform Under Crisis
The AIDS epidemic demonstrated that regulatory speed is a policy choice. AZT was approved in March 1987 in a record 20 months, without a Phase 3 trial, after Phase 2 showed 19 placebo deaths vs. 1 treatment death151. This proves expedited approval is technically feasible. However, from 1987-1993, no other AIDS drugs were approved, despite 257,000 diagnoses in 1993-1995 alone. ACT UP activism forced regulatory reforms (Parallel Track, Accelerated Approval), proving that the FDA’s pace reflects institutional priorities, not immutable scientific requirements.
3. Hepatitis C (2013-2014): Breakthrough Designation Success
Sovaldi (sofosbuvir) received FDA Breakthrough Therapy designation and was approved December 2013, with Harvoni following in October 2014. These drugs cure HCV in 12 weeks with >95% efficacy. In 2013, HCV caused 19,368 US deaths. Critically, despite rapid approval, no Thalidomide-scale disaster occurred. The drugs’ side effect profile was actually better than prior interferon-based treatments. This demonstrates that fast approval of transformative drugs is both possible and safe.
Implications for Causal Inference:
These cases establish that:
- Regulatory delays have measurable mortality costs (beta-blockers: if Wardell’s 10,000/year estimate holds, the 3-year US delay implies ~30,000 excess deaths)
- Fast approval is technically feasible when institutional will exists (AZT: 20 months; Sovaldi: Breakthrough pathway)
- Fast approval does not inevitably produce catastrophe (Sovaldi: excellent safety profile)
The counterfactual is not purely speculative: we observe the mechanism operating in discrete cases where data is available.
Methodology & Data
We define the Total Mortality Cost (\(D_{total}\)) as the sum of two distinct variables:
\[
D_{total} = D_{lag} + D_{void}
\]
Variable Definitions
- \(D_{lag}\) (Delay Mortality): Deaths occurring while existing, working drugs are in Phase II/III trials.
- \(D_{void}\) (Innovation Loss): Deaths occurring because high regulatory costs prevented the development of potential cures (The “Innovation Tax”).
Theoretical Upper Bound: What’s Eventually Preventable?
Before calculating regulatory delay costs, we must establish what percentage of deaths are theoretically preventable with sufficient biomedical advancement. This sets the upper bound for any intervention.
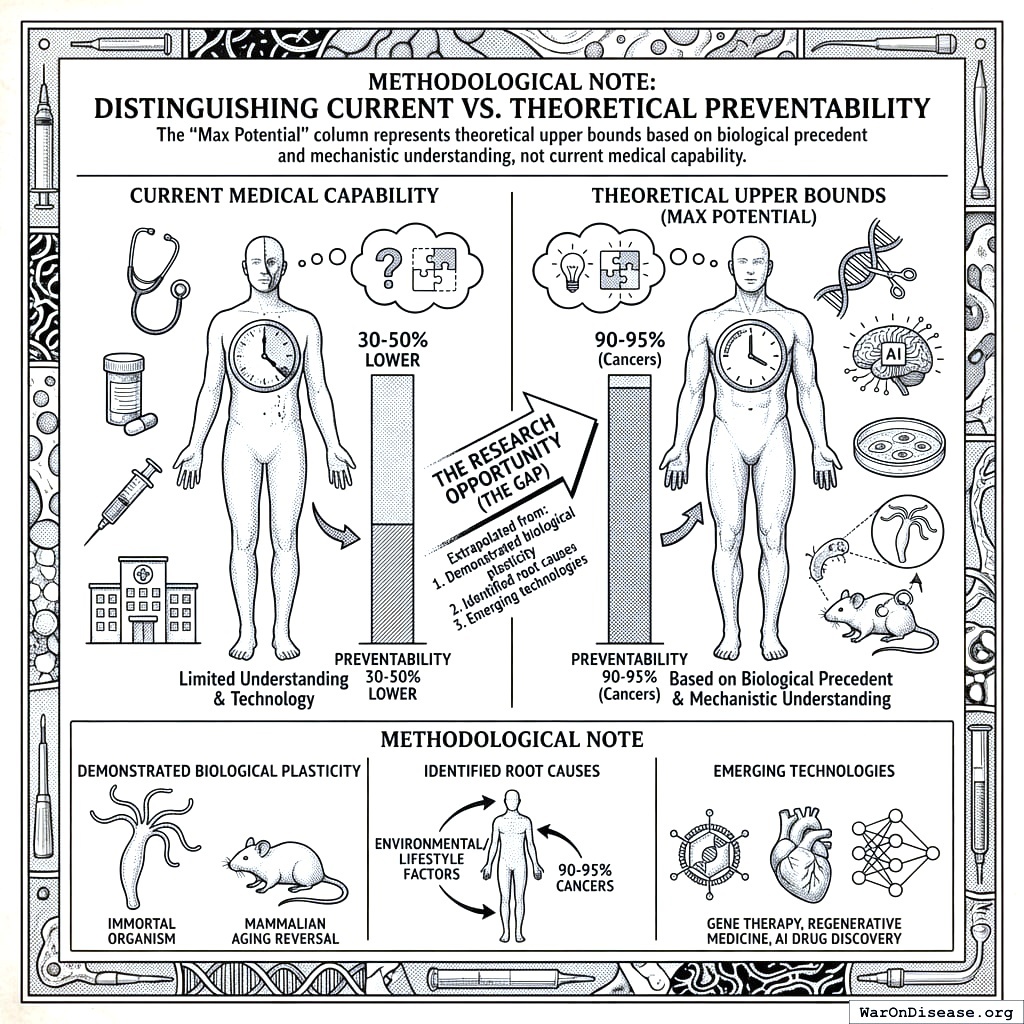
Methodological Note: Distinguishing Current vs. Theoretical Preventability
The “Max Potential” column represents theoretical upper bounds based on biological precedent and mechanistic understanding, not current medical capability. These estimates extrapolate from:
- Demonstrated biological plasticity (organisms that don’t age, mammalian aging reversal)
- Identified root causes (90-95% of cancers have environmental/lifestyle roots)
- Emerging technologies (gene therapy, regenerative medicine, AI drug discovery)
Current preventability is typically 30-50% lower than theoretical maximum. The gap represents the research opportunity.
Disease Burden by Category
Using WHO Global Burden of Disease152 data, we categorize annual deaths:
| Cardiovascular |
26.0% |
50% |
95% |
WHO: 80-90% preventable153 |
| Cancer |
18.9% |
69% |
95% |
90-95% environmental/lifestyle roots154 |
| Aging-related |
23.2% |
5% |
99% |
Mammalian aging reversal demonstrated155 |
| Accidents |
8.0% |
30% |
60% |
WHO: largely preventable156 |
| Metabolic |
6.3% |
70% |
98% |
Diabetes reversal via gene therapy157 |
| Respiratory |
4.3% |
60% |
90% |
WHO: 80% of COPD preventable |
| Neurodegenerative |
3.6% |
10% |
80% |
Stem cell therapy potential158 |
| Infectious |
1.9% |
95% |
99% |
Vaccines + antimicrobials159 |
| Other |
7.7% |
50% |
95% |
Weighted average of above categories |
Result: 92.6% (95% CI: 50%-98%) of deaths are eventually avoidable with sufficient research.
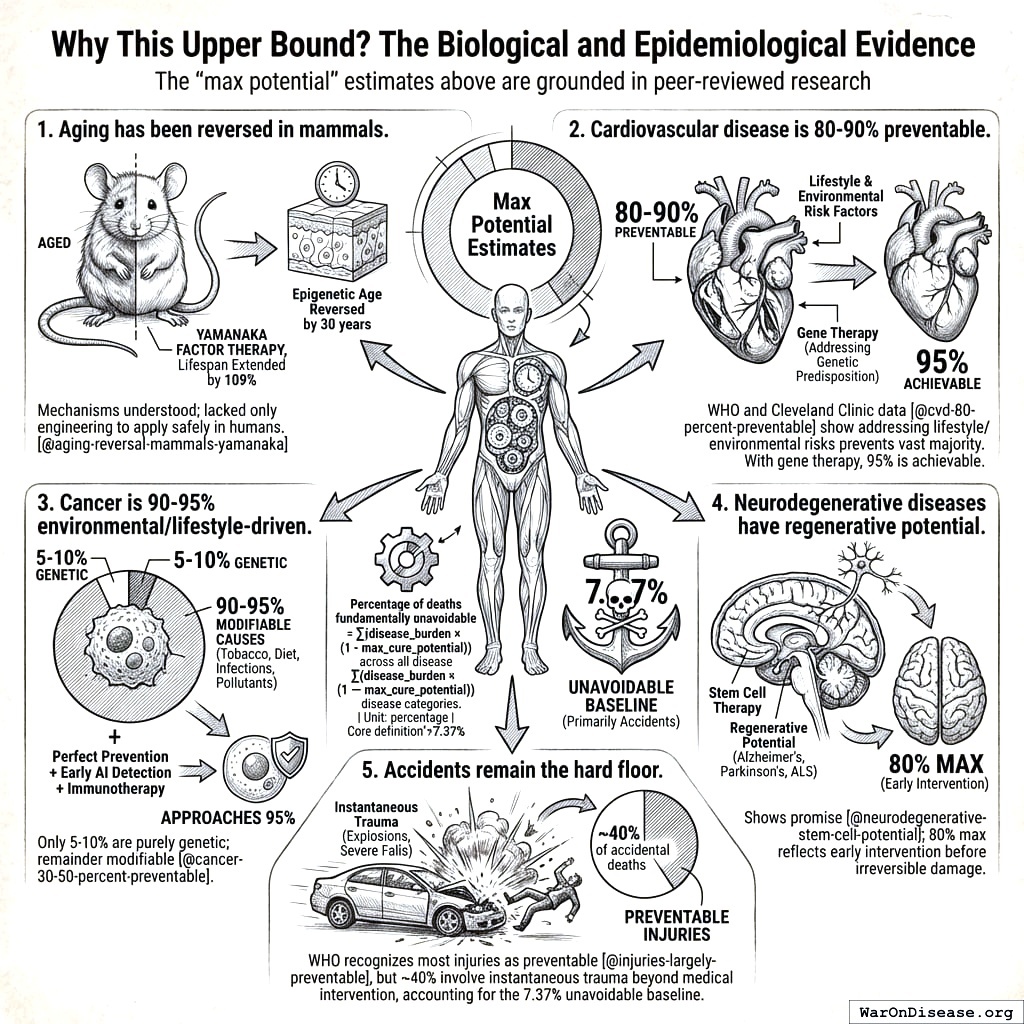
Why This Upper Bound? The Biological and Epidemiological Evidence
The “max potential” estimates above are grounded in peer-reviewed research:
- Aging has been reversed in mammals. Yamanaka factor therapy extended remaining lifespan by 109% in aged mice155 and reversed epigenetic age in human skin cells by 30 years. The mechanisms are understood; we lack only the engineering to apply them safely in humans.
Cardiovascular disease is 80-90% preventable. WHO and Cleveland Clinic data153 show that addressing lifestyle and environmental risk factors prevents the vast majority of heart attacks and strokes. With gene therapy addressing genetic predisposition, 95% is achievable.
Cancer is 90-95% environmental/lifestyle-driven. Only 5-10% of cancers are purely genetic154; the remainder have modifiable causes (tobacco, diet, infections, pollutants). Perfect prevention + early AI detection + immunotherapy approaches 95%.
Neurodegenerative diseases have regenerative potential. Stem cell therapy shows promise158 for Alzheimer’s, Parkinson’s, and ALS. The 80% max reflects early intervention before irreversible damage.
Accidents remain the hard floor. WHO recognizes most injuries as preventable156, but ~40% of accidental deaths involve instantaneous trauma (explosions, severe falls) beyond any medical intervention. This accounts for the 7.37% unavoidable baseline.
The 7.37% Floor
The remaining deaths are fundamentally unavoidable even with perfect biotechnology:
- Instantaneous traumatic death (e.g., explosions, severe falls)
- Drowning beyond rescue window
- Violence/homicide
- Certain catastrophic accidents
These represent the hard physical limits of medicine. Everything else, including “natural death from old age,” is an engineering problem with engineering solutions.
Data Sources & Parameterization
Development Timelines: Biotechnology Innovation Organization (BIO) Clinical Development Success Rates 2011–2020.
Pharmaceutical Impact (Life-Years Saved): Primary source: Lichtenberg (2019)86.
Note
Life-Years vs. Lives
Lichtenberg measured life-years saved, not lives. Converting to “lives” requires assuming average life extension per beneficiary (12 years (95% CI: 8 years-18 years)). Life-years is the more rigorous metric; lives is used for intuitive communication. The uncertainty in the conversion is reflected in the confidence intervals.
Supporting evidence (approximate, for context):
- Vaccines: ~4.5M lives/year (WHO estimates 154M lives saved over 50 years)159
- Cardiovascular: ~3.3M lives/year (Resolve to Save Lives / GBD Data)
- Oncology: ~1.5M lives/year (NBER longevity studies)
Economic Valuation: Standard QALY Valuation.
Uncertainty Quantification Methodology
This analysis employs Probabilistic Sensitivity Analysis (PSA) via Monte Carlo simulation to propagate parameter uncertainty through all calculations.
Distribution Selection:
- Normal: Symmetric uncertainty around point estimates (e.g., trial duration)
- Lognormal: Right-skewed, strictly positive values (costs, relative risks)
- Beta: Bounded probabilities [0,1] (success rates, adoption rates)
- Triangular: When only min/mode/max available from literature
Propagation Method:
- Sample N=10,000 draws from each input parameter’s distribution
- Recompute all derived parameters for each Monte Carlo draw
- Report median and 95% credible intervals (2.5th-97.5th percentiles)
Sensitivity Analysis:
Tornado charts identify which input parameters drive outcome uncertainty by varying each parameter ±1 standard deviation while holding others at baseline. Standardized regression coefficients (β*) enable comparison across parameters with different units.
See Parameters & Calculations Appendix for complete parameter distributions, formulas, and sensitivity analyses for each calculated value.
Results: The Mortality Burden
Primary Estimate
Important Clarification: Throughout this analysis, “regulatory delay” refers specifically to the post-safety efficacy testing delay - the period AFTER safety has been established but BEFORE efficacy approval is granted under current FDA/EMA requirements. This is distinct from safety testing (Phase I), which we consider necessary and effective (as demonstrated by the thalidomide case where safety testing prevented thousands of U.S. deaths).
Methodological Caveat: Cascade Assumption
The primary estimate assumes that the 8.2 years (95% CI: 4.85 years-11.5 years) regulatory delay cascades fully through the biomedical research timeline - i.e., that delaying Drug A by 8.2 years (95% CI: 4.85 years-11.5 years) also delays all downstream research that builds on Drug A’s findings by approximately the same amount. This “full cascade” assumption represents a theoretical upper bound. In practice, parallel research tracks, international approvals, and adaptive innovation may partially mitigate cascade effects.
The assumption is not empirically validated at the aggregate level, though individual case studies (beta-blockers, HIV/AIDS, Hepatitis C) demonstrate the mechanism operates in specific instances. The Type II/Type I ratio remains robust even under substantially reduced cascade assumptions (see sensitivity analysis showing the conclusion holds at 10% regulatory attribution).
Finding: The disease eradication delay model estimates 416 million deaths (95% CI: 225 million deaths-630 million deaths) total eventually avoidable deaths, with 150,000 per day, greater than the combined casualties of World War I and World War II over the 62-year period.
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
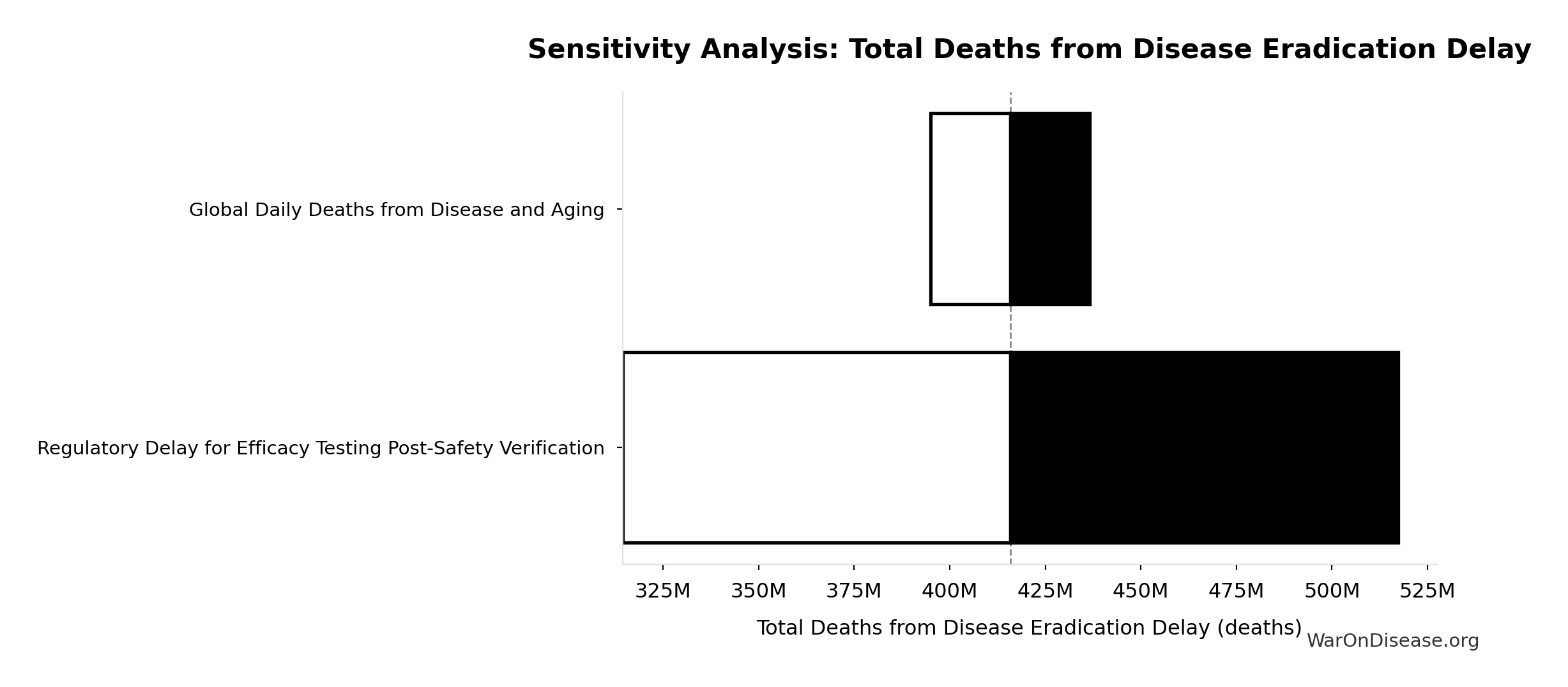
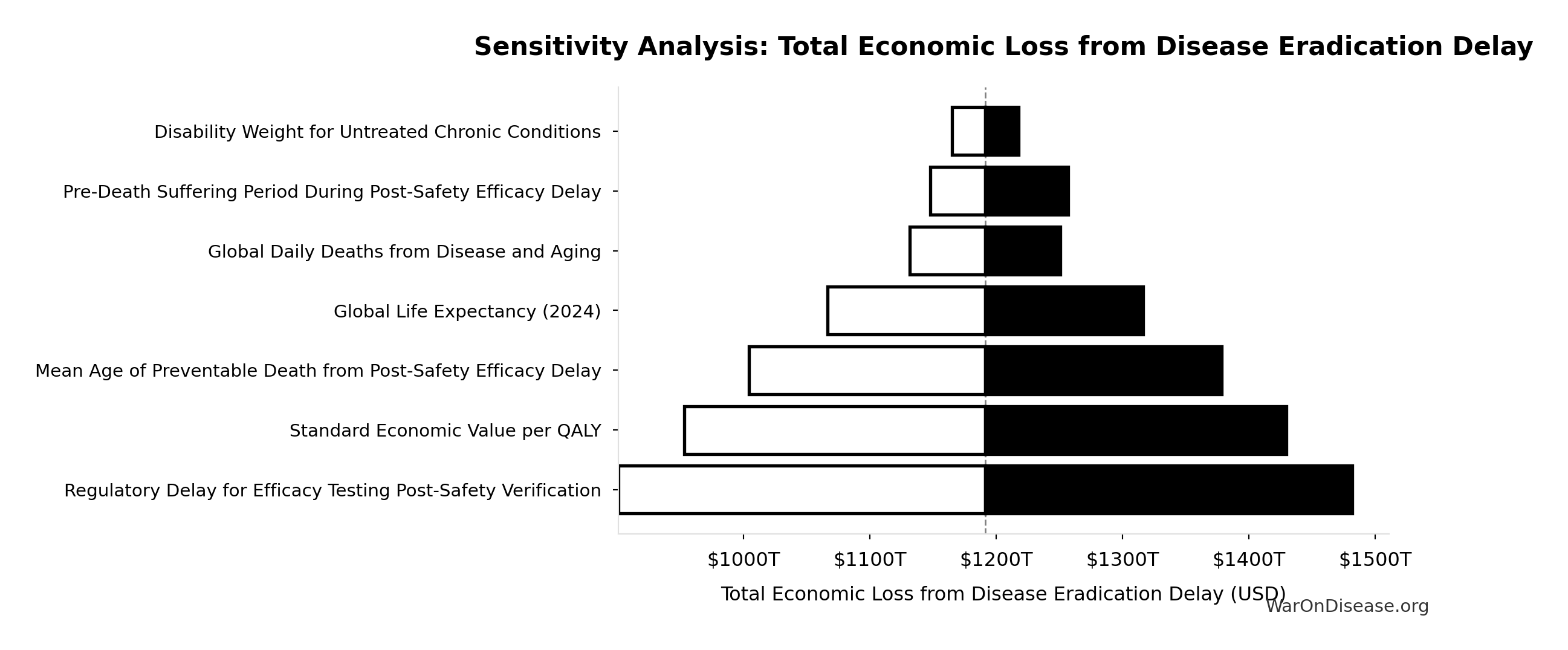
Sensitivity Analysis
Sensitivity Indices for Total Deaths from Disease Eradication Delay
Regression-based sensitivity showing which inputs explain the most variance in the output.
| Regulatory Delay for Efficacy Testing Post-Safety Verification (years) |
1.1404 |
Strong driver |
| Global Daily Deaths from Disease and Aging (deaths/day) |
-0.1422 |
Weak driver |
Interpretation: Standardized coefficients show the change in output (in SD units) per 1 SD change in input. Values near ±1 indicate strong influence; values exceeding ±1 may occur with correlated inputs.
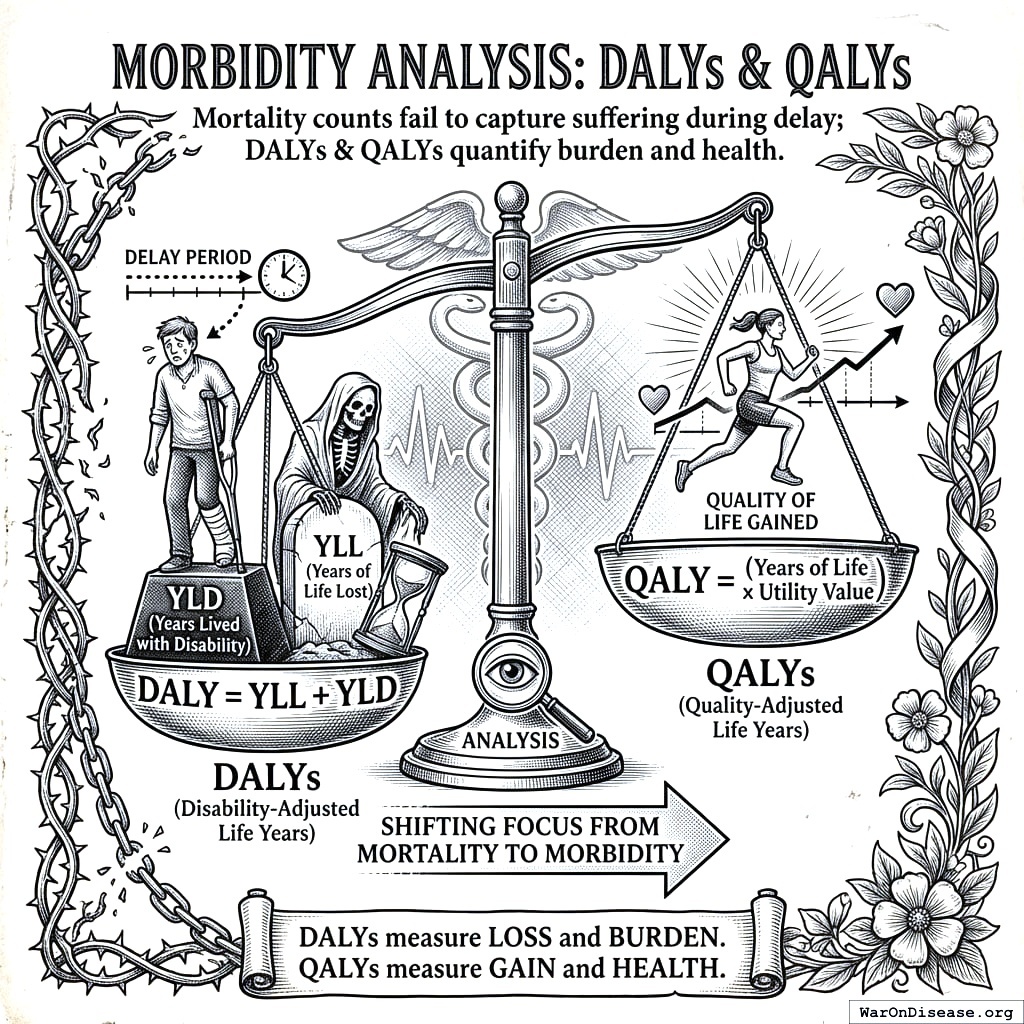
Morbidity Analysis: DALYs and QALYs
Mortality counts fail to capture the suffering of patients living with untreated disabilities during the delay period. We calculated Disability-Adjusted Life Years (DALYs) using the formula \(DALY = YLL + YLD\).
Years of Life Lost (YLL)
\[
\begin{gathered}
YLL_{lag} \\
= Deaths_{lag} \times (LE_{global} - Age_{death,delay}) \\
= 416M \times (79 - 62) \\
= 7.07B
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
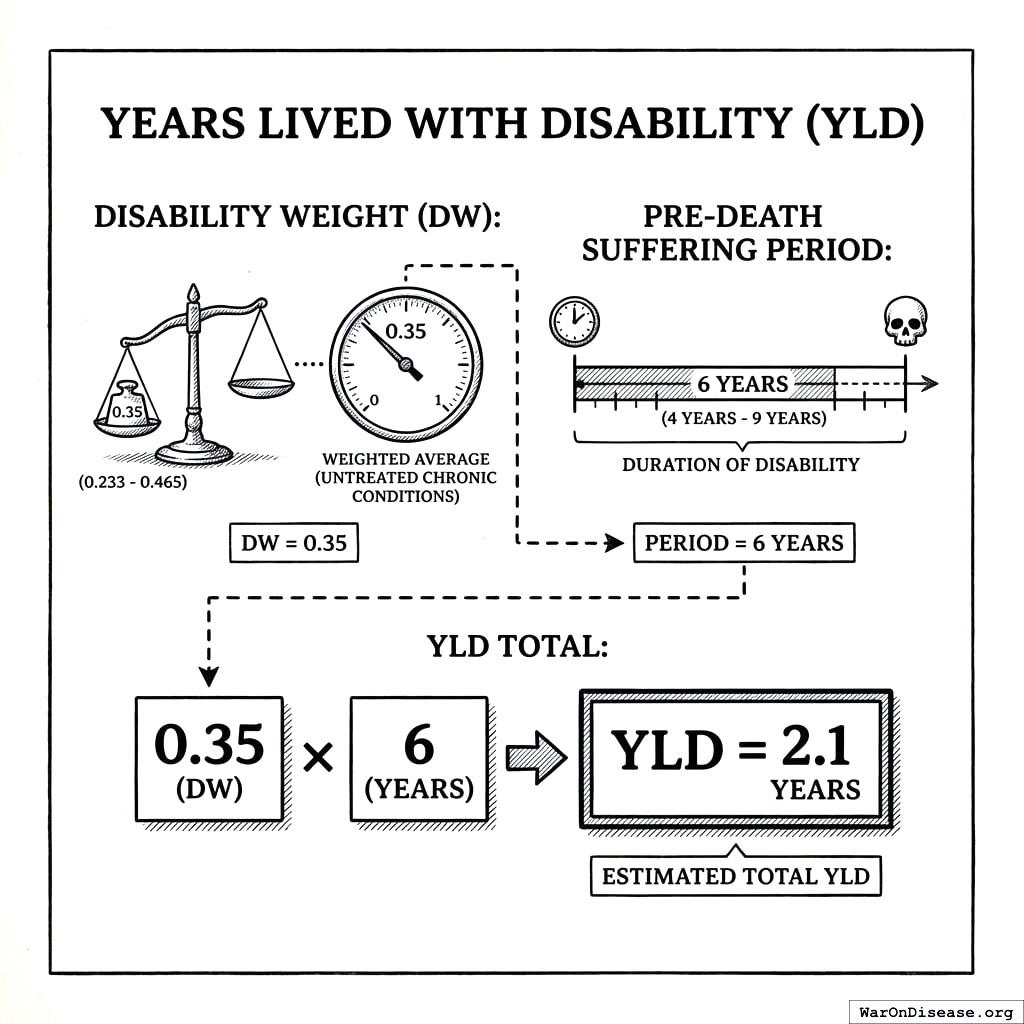
Years Lived with Disability (YLD)
\[
\begin{gathered}
YLD_{lag} \\
= Deaths_{lag} \times T_{suffering} \times DW_{chronic} \\
= 416M \times 6 \times 0.35 \\
= 873M
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
Cumulative DALY Burden
\[
DALYs_{lag} = YLL_{lag} + YLD_{lag} = 7.07B + 873M = 7.94B
\]
where:
\[
\begin{gathered}
YLL_{lag} \\
= Deaths_{lag} \times (LE_{global} - Age_{death,delay}) \\
= 416M \times (79 - 62) \\
= 7.07B
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
where:
\[
\begin{gathered}
YLD_{lag} \\
= Deaths_{lag} \times T_{suffering} \times DW_{chronic} \\
= 416M \times 6 \times 0.35 \\
= 873M
\end{gathered}
\]
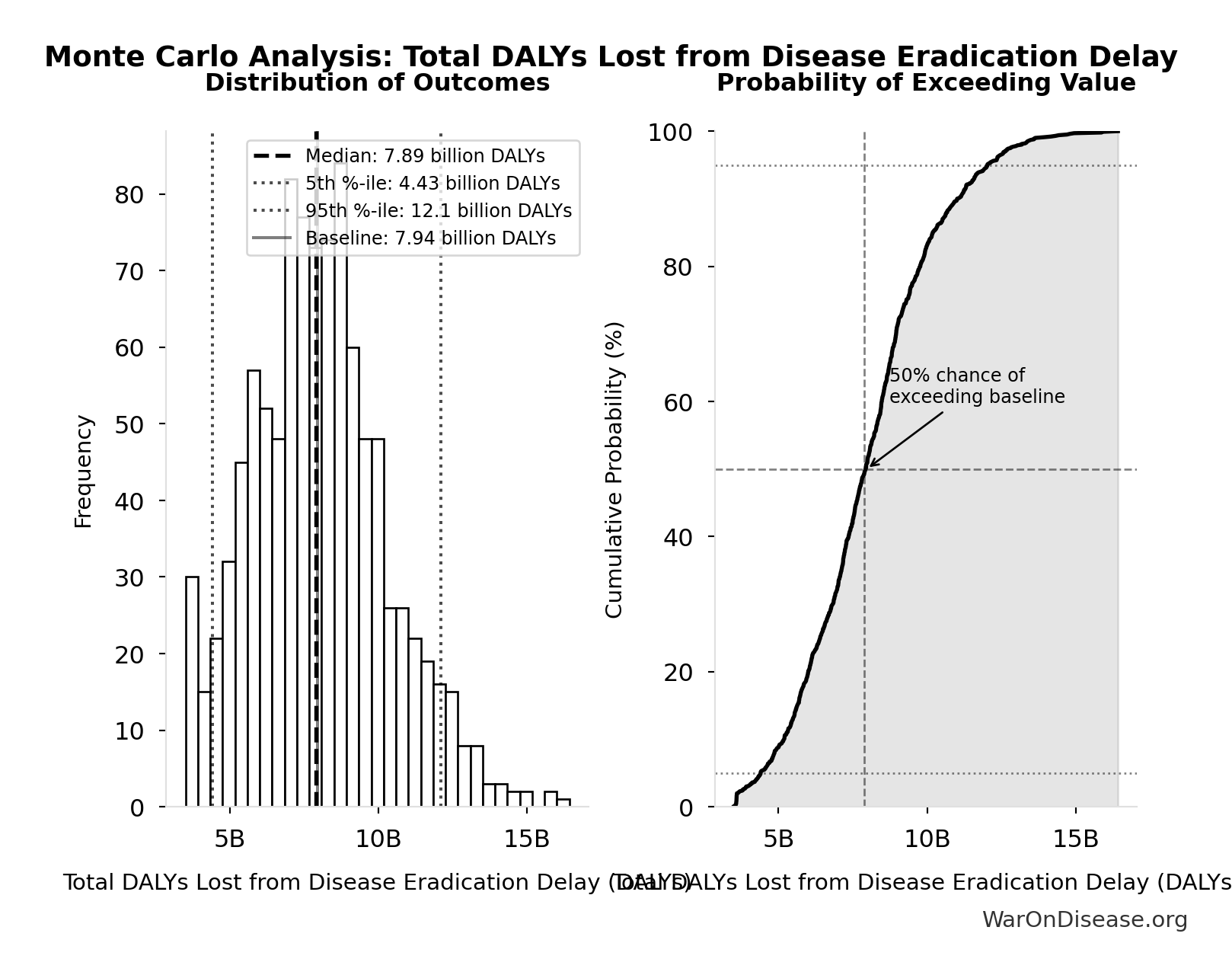
Simulation Results Summary: Total DALYs Lost from Disease Eradication Delay
| Baseline (deterministic) |
7.94 billion |
| Mean (expected value) |
8.05 billion |
| Median (50th percentile) |
7.89 billion |
| Standard Deviation |
2.31 billion |
| 90% Range (5th-95th percentile) |
[4.43 billion, 12.1 billion] |
The histogram shows the distribution of Total DALYs Lost from Disease Eradication Delay across 10,000 Monte Carlo simulations. The CDF (right) shows the probability of the outcome exceeding any given value, which is useful for risk assessment.
Interpretation: The regulatory framework has effectively deleted 7.94 billion DALYs (95% CI: 4.43 billion DALYs-12.1 billion DALYs) billion years of healthy human life.
Distinction: Mortality vs. Morbidity Burden
The “12.4 million lives saved annually” from Lichtenberg’s analysis captures mortality - people who would have died without post-1962 drugs. But pharmaceutical treatments primarily improve quality of life for people with non-terminal chronic conditions: diabetes, hypertension, depression, COPD, arthritis, and cardiovascular disease.
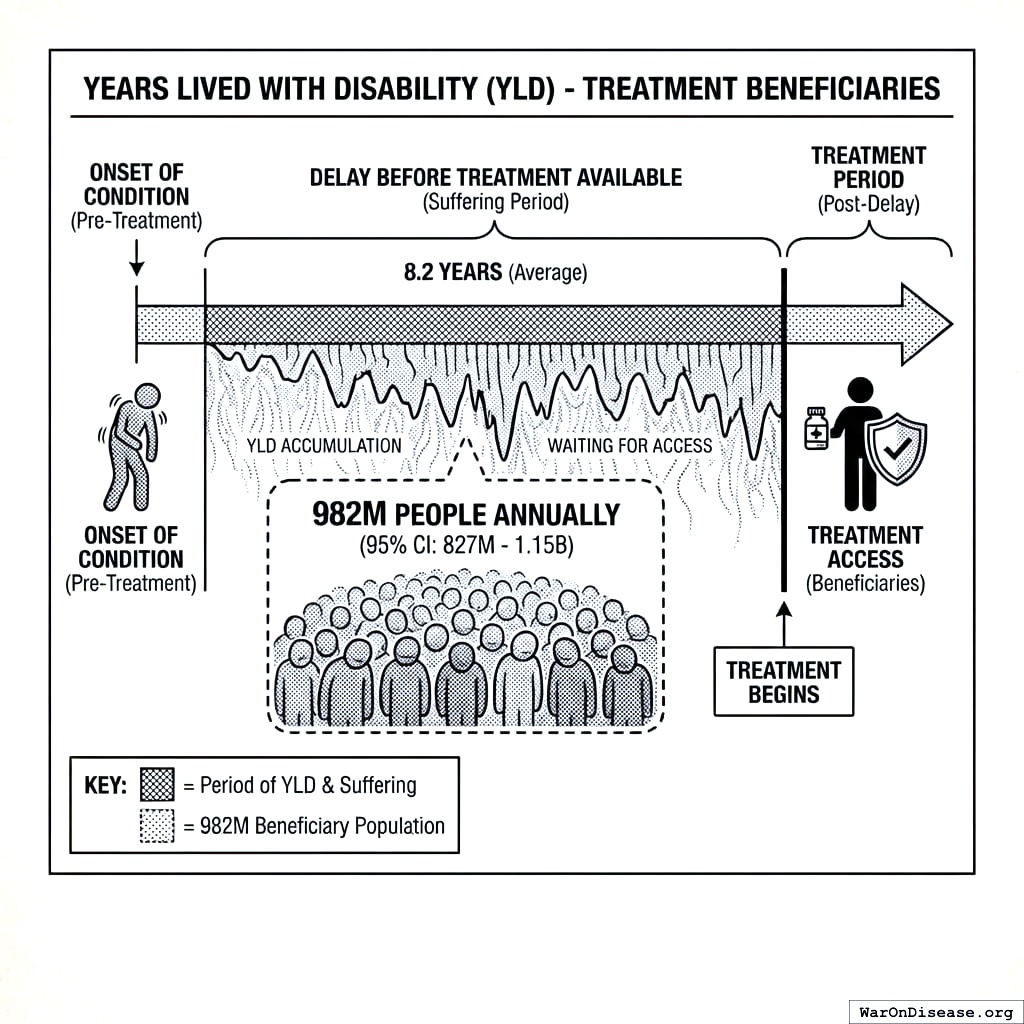
Treatment beneficiaries vastly exceed mortality beneficiaries.
Data source: IQVIA reports that global pharmaceutical use reached 1.8 trillion days of therapy in 2019, with 71% for chronic conditions (diabetes, CVD, respiratory, cancer)48. From this, we estimate approximately 982 million people (95% CI: 827 million people-1.15 billion people) unique patients receive chronic disease treatment annually.
Treatment beneficiary YLD calculation:
\[
\begin{gathered}
YLD_{treat\_delay} \\
= N_{treated} \times T_{lag} \times \Delta DW_{treat} \\
= 982M \times 8.2 \times 0.25 \\
= 2.01B
\end{gathered}
\]
where:
\[
\begin{gathered}
N_{treated} \\
= DOT_{chronic} \times 0.000767 \\
= 1.28T \times 0.000767 \\
= 982M
\end{gathered}
\]
Interpretation: Each year, patients receiving treatment for chronic conditions would have collectively avoided 2.01 billion DALYs (95% CI: 661 million DALYs-4.41 billion DALYs) of disability if those treatments had been available 8.2 years (95% CI: 4.85 years-11.5 years) earlier.
The treatment beneficiary population is approximately 80 times larger than the mortality-focused “lives saved” figure, demonstrating that the morbidity cost of regulatory delay vastly exceeds the mortality cost.
Economic Valuation
To quantify the Deadweight Loss (DWL) to the global economy, we apply the Value of a Statistical Life Year (VSLY).
\[
DWL = \sum (DALY_{loss} \times VSLY)
\]
Using a conservative global VSLY of $150,000 (95% CI: $100,000-$199,282):
\[
\begin{gathered}
Value_{lag} \\
= DALYs_{lag} \times Value_{QALY} \\
= 7.94B \times \$150K \\
= \$1190T
\end{gathered}
\]
where:
\[
DALYs_{lag} = YLL_{lag} + YLD_{lag} = 7.07B + 873M = 7.94B
\]
where:
\[
\begin{gathered}
YLL_{lag} \\
= Deaths_{lag} \times (LE_{global} - Age_{death,delay}) \\
= 416M \times (79 - 62) \\
= 7.07B
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
where:
\[
\begin{gathered}
YLD_{lag} \\
= Deaths_{lag} \times T_{suffering} \times DW_{chronic} \\
= 416M \times 6 \times 0.35 \\
= 873M
\end{gathered}
\]
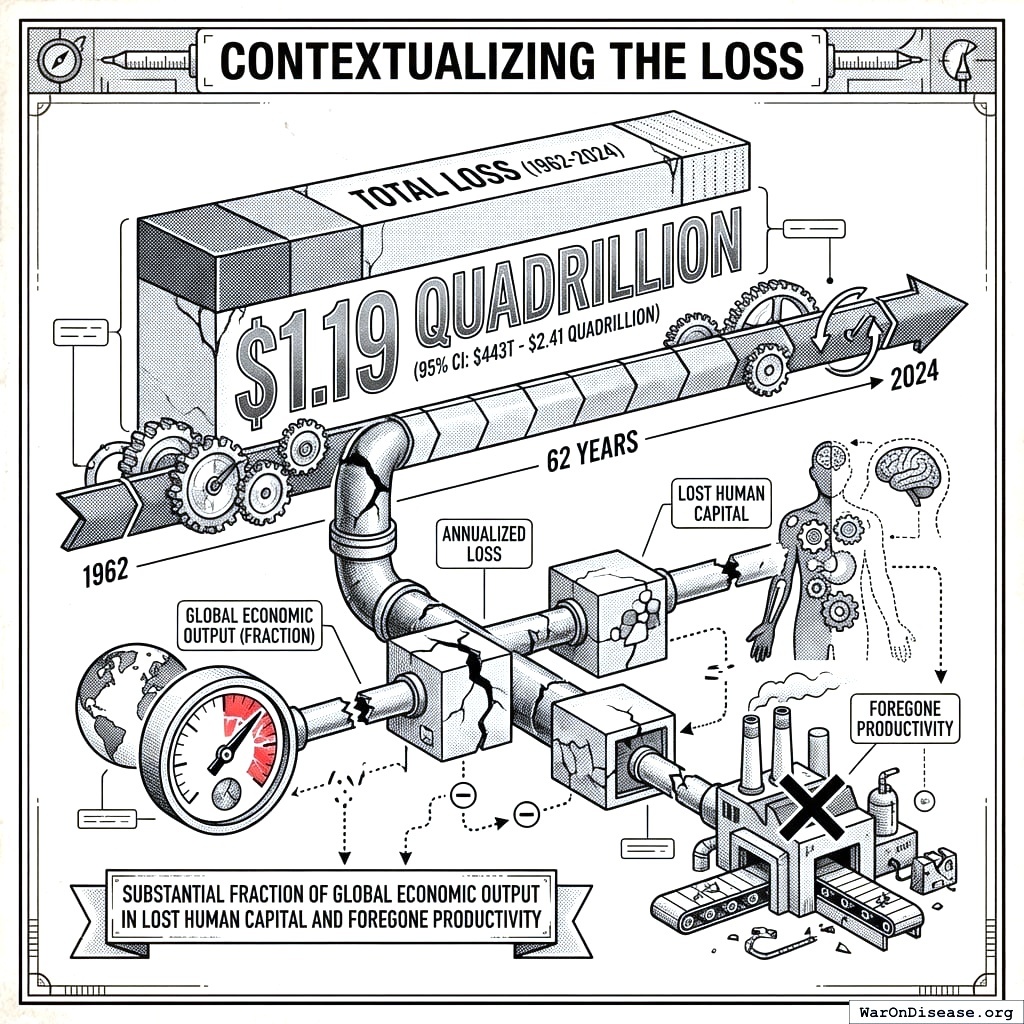
Contextualizing the Loss
- Total Loss (1962-2024): $1.19 quadrillion (95% CI: $443 trillion-$2.41 quadrillion) over 62 years (averaging approximately $19 trillion/year, or roughly 18% of annual global GDP in lost human capital)
- Annualized Loss: Total loss / 62 years represents a substantial fraction of global economic output in lost human capital and foregone productivity
Risk Analysis: The Type I vs. Type II Ratio
A critical counter-argument is that the FDA protects society from dangerous or ineffective drugs (Type I Errors). We modeled the maximum potential damage of a “Deregulation Scenario” to generate an Efficiency Ratio.
Methodological Note: Steelmanning the FDA’s Position
To ensure this analysis is maximally fair to proponents of current FDA regulation, we deliberately assume the worst possible case for Type I errors (harm from approving bad drugs). This “steelman” approach means that even if our assumptions are completely wrong in favor of FDA defenders, the conclusion holds.
Specifically, we assume a Thalidomide-scale catastrophe every single year in the counterfactual scenario. This is an extraordinarily extreme overestimate for three reasons:
- Thalidomide was a once-in-a-century event - no comparable disaster has occurred since
- We propose retaining Phase I safety testing - our critique is of efficacy requirements (Phase II/III), not safety requirements
- Thalidomide was caught by 1938 safety requirements, NOT 1962 efficacy requirements - FDA’s Dr. Frances Kelsey blocked thalidomide approval based on safety concerns about nerve damage, using authority from the 1938 Food, Drug, and Cosmetic Act. The 1962 efficacy amendments hadn’t yet passed. Under our proposal, thalidomide would STILL have been blocked.
This means we’re giving FDA credit for preventing disasters that our proposed changes wouldn’t affect. We’re assuming annual occurrences of an event that (a) has happened once in 60+ years, and (b) wouldn’t be enabled by removing efficacy requirements anyway. This is the maximum possible benefit of the doubt.
Type I Benefit Calculation (Steelman):
\[
\begin{gathered}
DALY_{TypeI} \\
= DALY_{thal} \times 62 \\
= 41{,}800 \times 62 \\
= 2.59M
\end{gathered}
\]
where:
\[
\begin{gathered}
DALY_{thal} \\
= YLD_{thal} + YLL_{thal} \\
= 13{,}000 + 28{,}800 \\
= 41{,}800
\end{gathered}
\]
where:
\[
\begin{gathered}
YLD_{thal} \\
= DW_{thal} \times N_{thal,survive} \times LE_{thal} \\
= 0.4 \times 540 \times 60 \\
= 13{,}000
\end{gathered}
\]
where:
\[
\begin{gathered}
N_{thal,survive} \\
= N_{thal,US,prevent} \times (1 - Rate_{thal,mort}) \\
= 900 \times (1 - 40\%) \\
= 540
\end{gathered}
\]
where:
\[
\begin{gathered}
N_{thal,US,prevent} \\
= N_{thal,global} \times Pct_{US,1960} \\
= 15{,}000 \times 6\% \\
= 900
\end{gathered}
\]
where:
\[
\begin{gathered}
YLL_{thal} \\
= Deaths_{thal} \times 80 \\
= 360 \times 80 \\
= 28{,}800
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{thal} \\
= Rate_{thal,mort} \times N_{thal,US,prevent} \\
= 40\% \times 900 \\
= 360
\end{gathered}
\]
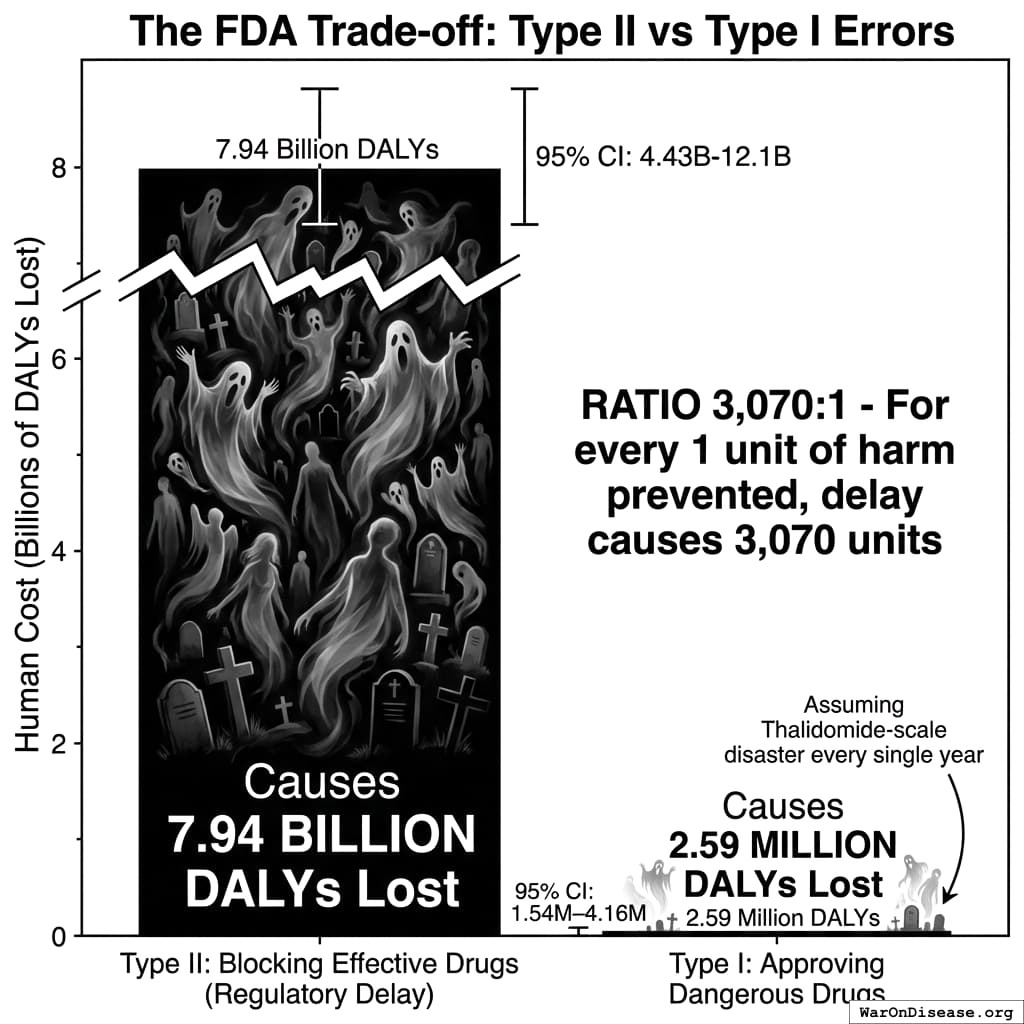
The Risk Trade-off Ratio
\[
\begin{gathered}
Ratio_{TypeII} \\
= \frac{DALYs_{lag}}{DALY_{TypeI}} \\
= \frac{7.94B}{2.59M} \\
= 3{,}070
\end{gathered}
\]
where:
\[
DALYs_{lag} = YLL_{lag} + YLD_{lag} = 7.07B + 873M = 7.94B
\]
where:
\[
\begin{gathered}
YLL_{lag} \\
= Deaths_{lag} \times (LE_{global} - Age_{death,delay}) \\
= 416M \times (79 - 62) \\
= 7.07B
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{lag} \\
= T_{lag} \times Deaths_{disease,daily} \times 338 \\
= 8.2 \times 150{,}000 \times 338 \\
= 416M
\end{gathered}
\]
where:
\[
\begin{gathered}
YLD_{lag} \\
= Deaths_{lag} \times T_{suffering} \times DW_{chronic} \\
= 416M \times 6 \times 0.35 \\
= 873M
\end{gathered}
\]
where:
\[
\begin{gathered}
DALY_{TypeI} \\
= DALY_{thal} \times 62 \\
= 41{,}800 \times 62 \\
= 2.59M
\end{gathered}
\]
where:
\[
\begin{gathered}
DALY_{thal} \\
= YLD_{thal} + YLL_{thal} \\
= 13{,}000 + 28{,}800 \\
= 41{,}800
\end{gathered}
\]
where:
\[
\begin{gathered}
YLD_{thal} \\
= DW_{thal} \times N_{thal,survive} \times LE_{thal} \\
= 0.4 \times 540 \times 60 \\
= 13{,}000
\end{gathered}
\]
where:
\[
\begin{gathered}
N_{thal,survive} \\
= N_{thal,US,prevent} \times (1 - Rate_{thal,mort}) \\
= 900 \times (1 - 40\%) \\
= 540
\end{gathered}
\]
where:
\[
\begin{gathered}
N_{thal,US,prevent} \\
= N_{thal,global} \times Pct_{US,1960} \\
= 15{,}000 \times 6\% \\
= 900
\end{gathered}
\]
where:
\[
\begin{gathered}
YLL_{thal} \\
= Deaths_{thal} \times 80 \\
= 360 \times 80 \\
= 28{,}800
\end{gathered}
\]
where:
\[
\begin{gathered}
Deaths_{thal} \\
= Rate_{thal,mort} \times N_{thal,US,prevent} \\
= 40\% \times 900 \\
= 360
\end{gathered}
\]
Conclusion: For every 1 unit of harm the FDA prevents (Type I errors: approving dangerous/ineffective drugs), it generates 3,068 (95% CI: 2,878-3,125) units of harm through delay (Type II errors: blocking effective drugs). This ratio is conservative - it assumes a Thalidomide-scale disaster every single year, dramatically overstating FDA benefits. With realistic Type I estimates, the ratio would be far higher.
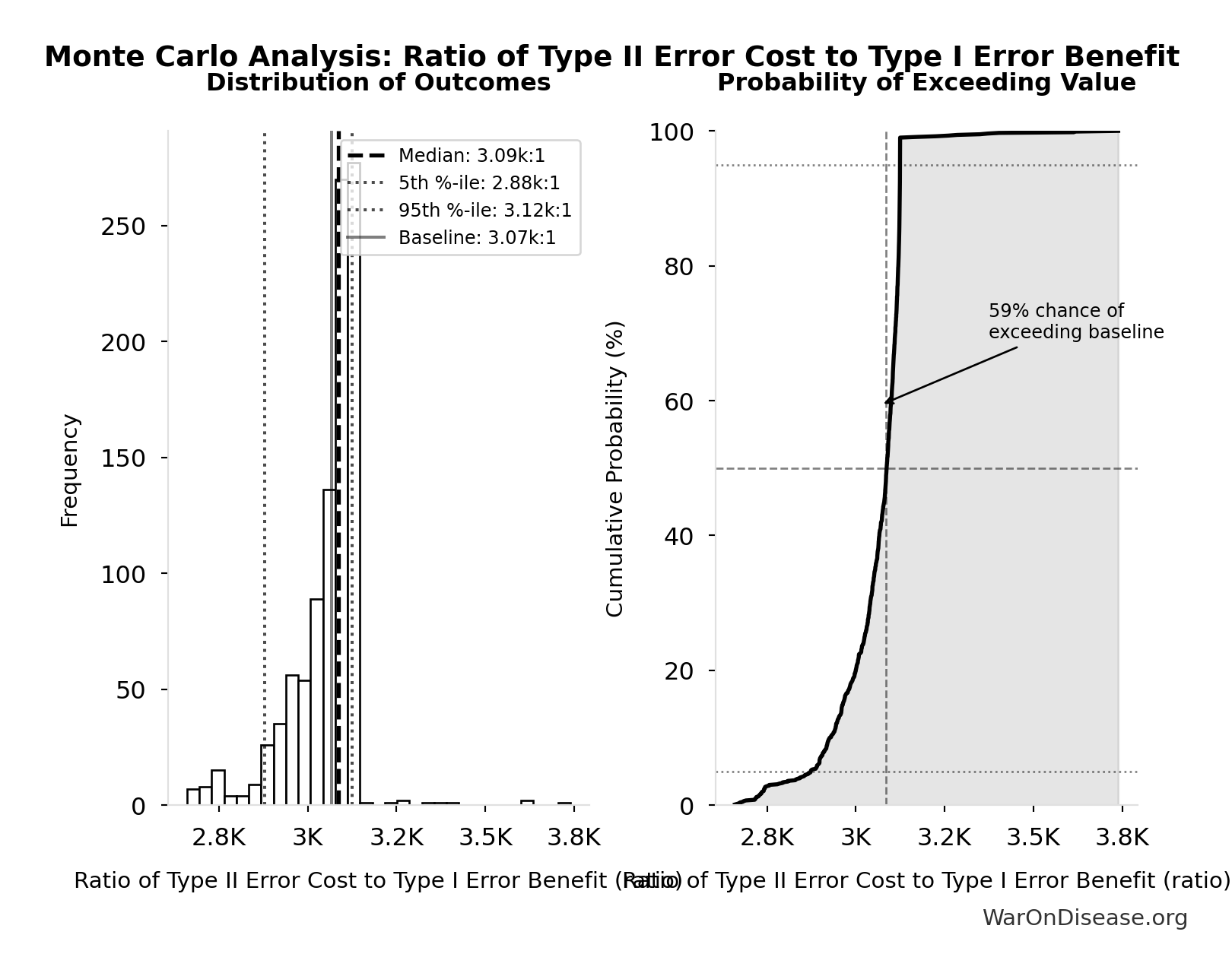
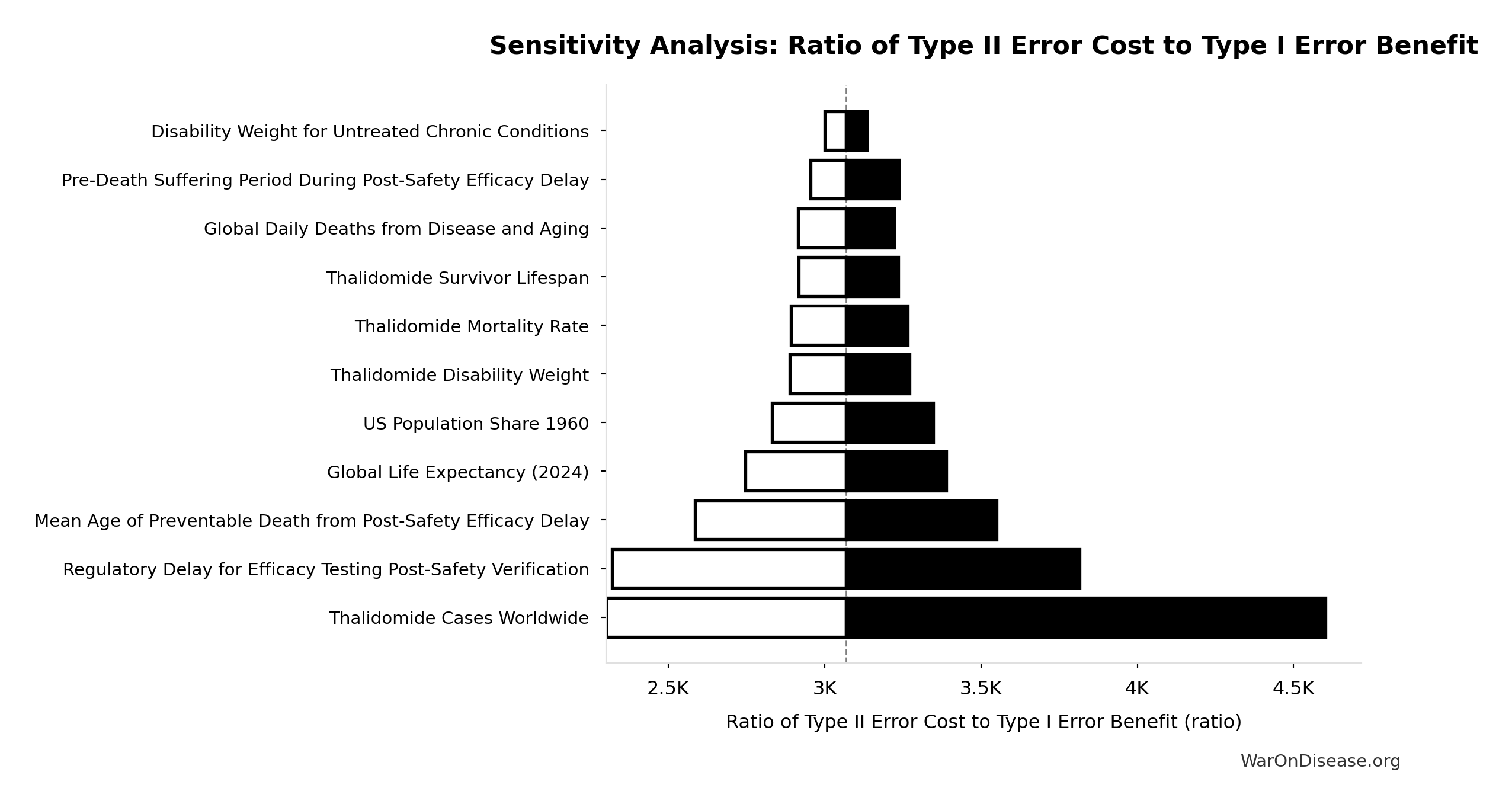
Simulation Results Summary: Ratio of Type II Error Cost to Type I Error Benefit
| Baseline (deterministic) |
3,068:1 |
| Mean (expected value) |
3,055:1 |
| Median (50th percentile) |
3,086:1 |
| Standard Deviation |
101:1 |
| 90% Range (5th-95th percentile) |
[2,878:1, 3,125:1] |
The histogram shows the distribution of Ratio of Type II Error Cost to Type I Error Benefit across 10,000 Monte Carlo simulations. The CDF (right) shows the probability of the outcome exceeding any given value, which is useful for risk assessment.
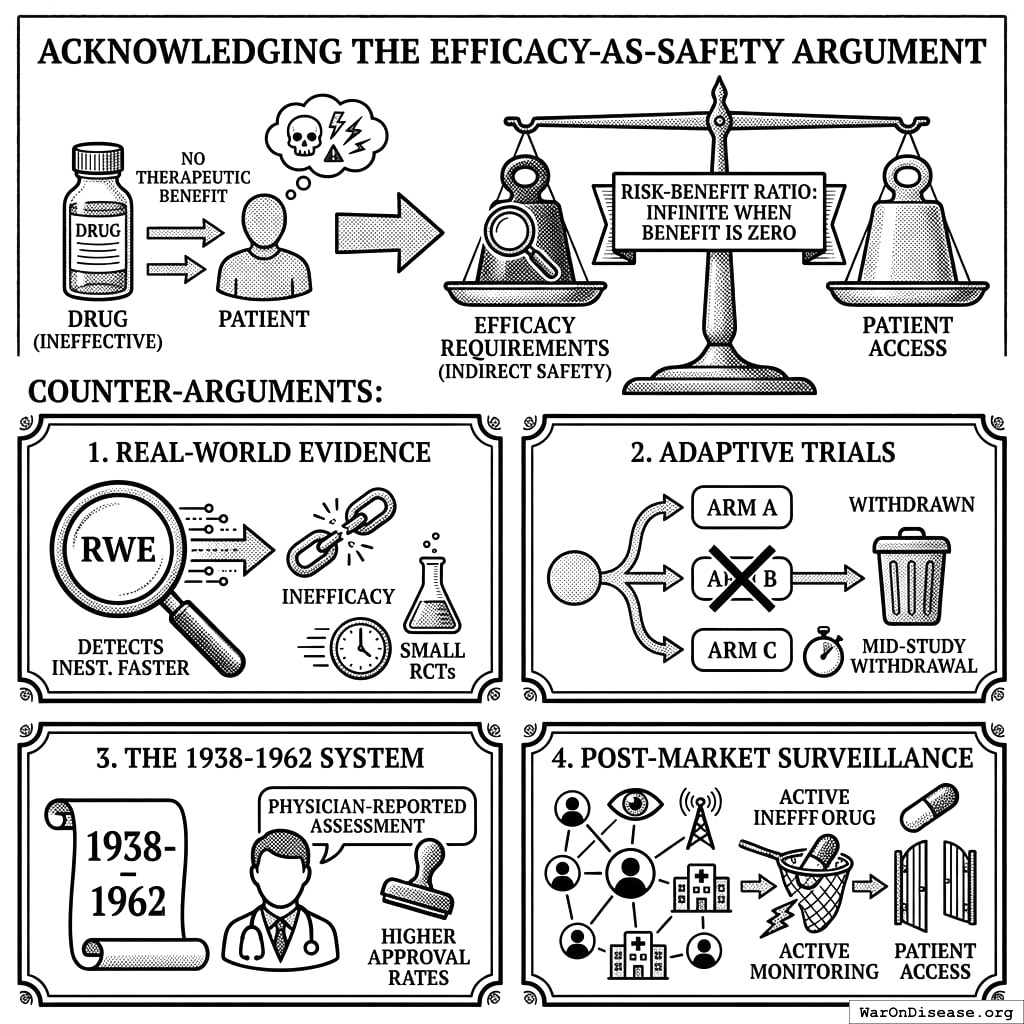
Acknowledging the Efficacy-as-Safety Argument
A legitimate concern deserves direct engagement: efficacy requirements may function as indirect safety measures. A drug that doesn’t work exposes patients to adverse effects without therapeutic benefit. The risk-benefit ratio becomes infinite when benefit is zero.
Counter-arguments:
- Real-world evidence detects inefficacy faster than small RCTs with selected populations
- Adaptive trials can withdraw ineffective arms mid-study without full Phase III completion
- The 1938-1962 system had physician-reported efficacy assessment without pre-market mandates, and higher approval rates
- Post-market surveillance with active monitoring catches ineffective drugs while allowing patient access
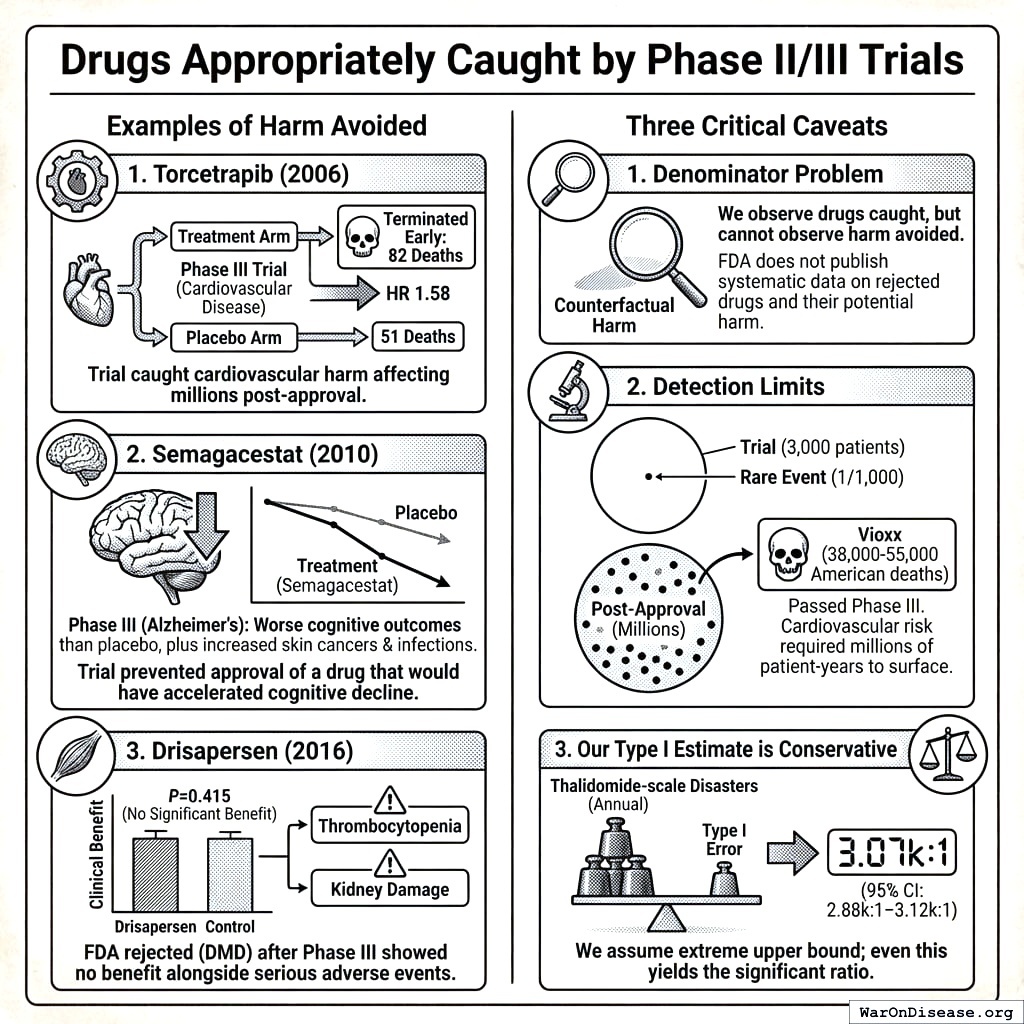
Drugs Appropriately Caught by Phase II/III Trials
This analysis acknowledges that Phase II/III trials do catch some drugs that would have caused harm. Three notable examples:
- Torcetrapib (2006): Phase III trial of this CETP inhibitor for cardiovascular disease was terminated early after 82 deaths in the treatment arm vs. 51 in placebo (HR 1.58). The trial caught cardiovascular harm that would have affected millions of patients post-approval160.
Semagacestat (2010): Phase III trial for Alzheimer’s disease found patients on treatment had worse cognitive outcomes than placebo, plus increased skin cancers and infections. The trial prevented approval of a drug that would have accelerated cognitive decline161.
Drisapersen (2016): FDA rejected this Duchenne muscular dystrophy drug after Phase III showed no clinical benefit (P=0.415) alongside serious adverse events including thrombocytopenia and kidney damage in significant fractions of patients162.
However, three critical caveats apply:
Denominator problem: We observe drugs caught by trials but cannot observe the counterfactual harm avoided. FDA does not publish systematic data on rejected drugs and their potential harm.
Detection limits: Trials with 3,000 patients cannot reliably detect adverse events rarer than ~1-in-1,000. Vioxx (38,000-55,000 American deaths) passed Phase III because its cardiovascular risk required millions of patient-years to surface163.
Our Type I estimate is conservative: We assume Thalidomide-scale disasters every year, an extreme upper bound that still yields the 3,068 (95% CI: 2,878-3,125) ratio.
Model Assumptions and Limitations
Key Assumptions
- Linear Adoption Model: Assumes drug uptake follows a predictable pattern post-approval
- Constant VSLY: Uses global average of $150,000 (95% CI: $100,000-$199,282)/year
- No Regulatory Learning: Assumes FDA efficiency remained constant 1962-2024
- Independence: Treats each drug approval as independent (may underestimate synergies)
Sensitivity Analysis
The model was tested across multiple scenarios:
Results remain robust across all reasonable parameter ranges, with lower bound estimates exceeding 100M deaths in all scenarios.
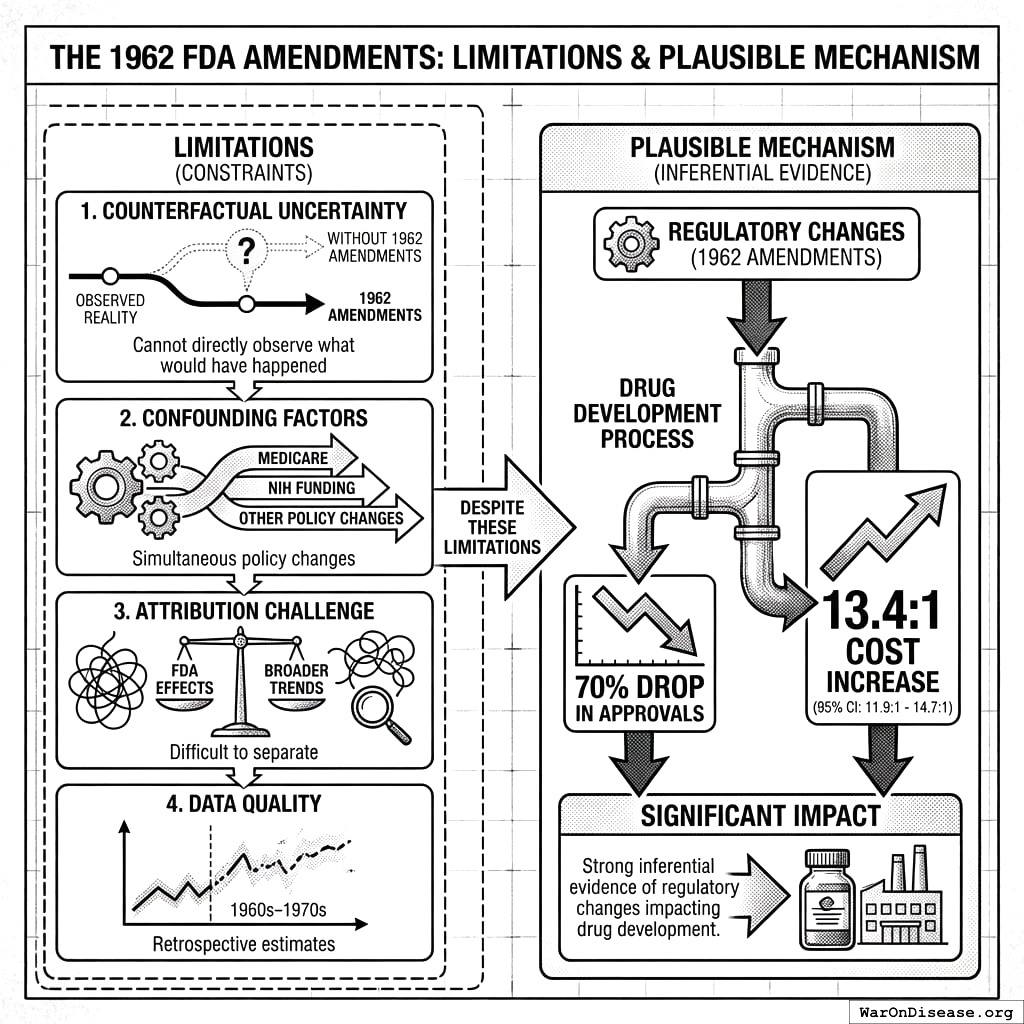
Limitations
- Counterfactual Uncertainty: Cannot directly observe what would have happened without 1962 amendments
- Confounding Factors: Other policy changes occurred simultaneously (Medicare, NIH funding)
- Attribution Challenge: Difficult to separate FDA effects from broader trends
- Data Quality: Early period (1960s-1970s) relies on retrospective estimates
Despite these limitations, the plausible mechanism (70% drop in approvals, 13.4x (95% CI: 11.9x-14.7x) cost increase) provides strong inferential evidence that regulatory changes significantly impacted drug development.
Policy Implications
The False Trade-off
The current debate frames drug approval as a choice between:
- Safety (slow, expensive approval) vs.
- Speed (fast, dangerous approval)
This is a false dichotomy. The evidence suggests:
- Phase I safety testing works (Thalidomide prevented in US)
- Phase II/III efficacy mandates fail (70% fewer approvals, worse real-world outcomes)
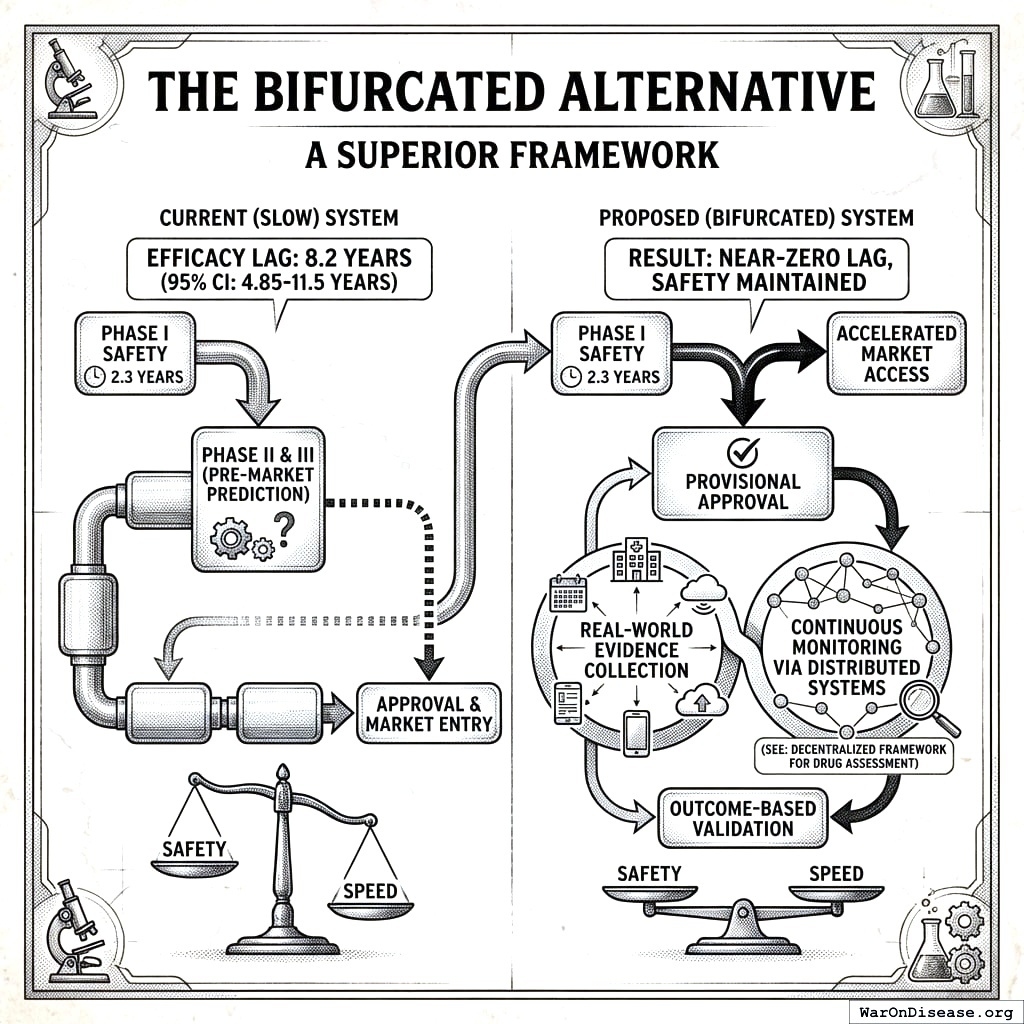
The Bifurcated Alternative
A superior framework would:
- Maintain rigorous Phase I safety testing (2.3 years)
- Allow provisional approval post-safety with real-world evidence collection
- Continuous monitoring via distributed systems (see: decentralized FDA164,165)
- Outcome-based validation rather than pre-market prediction
This approach would reduce the efficacy lag from 8.2 years (95% CI: 4.85 years-11.5 years) to near-zero while maintaining safety standards.
Expected Impact
If implemented today, the bifurcated model would:
See 1% treaty impact analysis166 for full quantified cost-benefit analysis.
International Regulatory Comparison
Several countries have implemented alternative regulatory models that provide natural experiments:
| USA (FDA) |
Full Phase III required |
10.5 years (95% CI: 6 years-12 years) |
Baseline for comparison |
| Japan (PMDA) |
Conditional approval after Phase II |
2-3 years |
Regenerative Medicine Act (2014); real-world monitoring167 |
| EU (EMA) |
Adaptive Pathways available |
~10 years |
Similar to FDA; conditional marketing authorization option |
| Canada |
Priority Review pathway |
~12 months (priority) |
Limited data on outcomes |
| Australia (TGA) |
Provisional approval pathway |
Variable |
Similar conditional pathways |
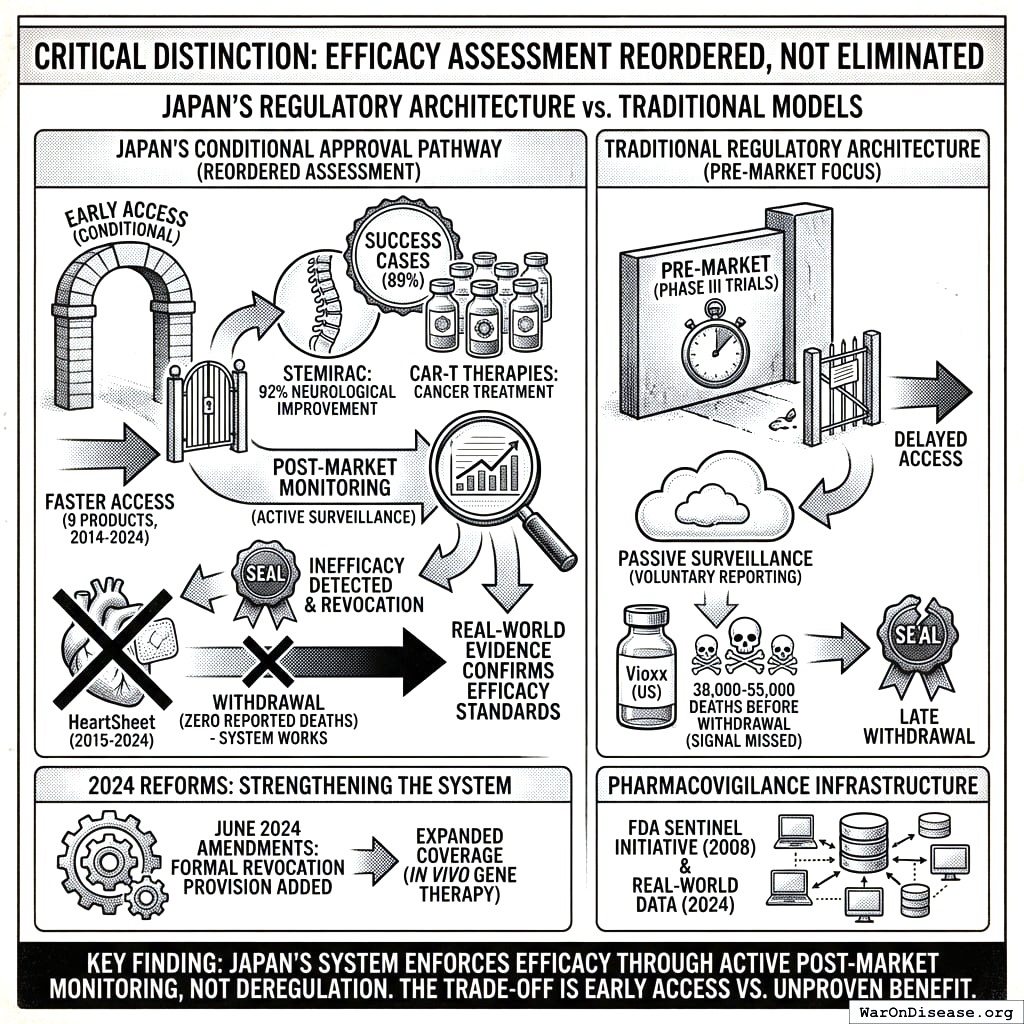
Critical Distinction: Efficacy Assessment Reordered, Not Eliminated
Japan’s conditional approval does NOT eliminate efficacy assessment. It REORDERS it from pre-market (Phase III trials) to post-market (real-world monitoring with revocation authority). This is a different regulatory architecture, not deregulation. The HeartSheet withdrawal proves the system still enforces efficacy standards, just through different mechanisms.
Key finding: Japan’s conditional approval system has an 89% success rate (8/9 products) and demonstrated that post-market monitoring CAN catch ineffective treatments:
- Faster access: 9 products received conditional early approval (2014-2024), reaching patients years earlier than traditional pathways
- Success cases: STEMIRAC (spinal cord injury) showed 12/13 patients (92%) achieved neurological improvement, with 2 of 5 completely paralyzed patients regaining motor function168. Five CAR-T therapies (Kymriah, Yescarta, Breyanzi, Abecma, Carvykti) are treating cancer patients under national insurance coverage169.
- The system caught inefficacy: HeartSheet was conditionally approved in 2015 with the requirement to prove efficacy through post-market data. In 2024, after collecting real-world evidence, MHLW determined it hadn’t demonstrated efficacy. The manufacturer voluntarily withdrew170 the next day. This is the system working as designed - conditional approval was conditional, and the condition wasn’t met.
- Contrast with FDA: Vioxx killed 38,000-55,000 Americans before withdrawal because the 6% voluntary reporting system failed to detect the signal. Japan’s active monitoring caught HeartSheet’s lack of efficacy with zero reported deaths.
The real question for HeartSheet: During those 9 years, did heart failure patients (who have few alternatives) benefit from access to an unproven treatment? The safety profile was acceptable - efficacy was the issue. This is a genuine tradeoff that merits cost-benefit analysis, not automatic condemnation.
2024 reforms strengthen, not abandon, conditional approval: Japan’s June 2024 amendments171 to the Regenerative Medicine Act add a formal revocation provision that was previously missing. The old system had no legal mechanism to force withdrawal if efficacy wasn’t proven - HeartSheet was voluntary. The reforms close this gap while expanding coverage to in vivo gene therapy. Japan is refining conditional approval based on experience, not abandoning it.
Pharmacovigilance infrastructure exists: The FDA launched the Sentinel Initiative172 in 2008 to monitor safety using electronic health records. In 2024, FDA eliminated major barriers173 to using real-world data. The technology for active surveillance exists - the barrier is institutional inertia, not technical impossibility.
Addressing Common Critiques
This analysis will face predictable objections. We address them here not defensively, but to demonstrate that the core conclusion, that regulatory delay costs vastly exceed regulatory benefits, remains robust even under unfavorable assumptions.
“The ‘Eventually Preventable’ Estimate Is Theoretical”
Critique: The claim that 92.6% (95% CI: 50%-98%) of deaths are eventually preventable is based on theoretical biological potential, not demonstrated medical capability.
Response:
Correct. That’s what “eventually” means.
The document explicitly distinguishes “Current” from “Max Potential” in the disease burden table (Section 2.2). The 92.6% (95% CI: 50%-98%) represents the theoretical upper bound based on:
- Aging reversed in mammals: Yamanaka factors extended remaining lifespan by 109% in aged mice155
- Cardiovascular disease 80-90% preventable NOW: WHO data153 with current interventions
- Cancer 90-95% environmental: Only 5-10% purely genetic154, remainder has modifiable causes
The relevant question isn’t “Can we achieve this upper bound?”
The question is: “When do we achieve it?”
If regulations delay progress by 8.2 years (95% CI: 4.85 years-11.5 years), everyone who dies during that window dies because of the delay.
Note: The PRIMARY estimate uses global disease mortality rates, not the 92.6% (95% CI: 50%-98%) ceiling. This upper bound provides context for the theoretical maximum scenario.
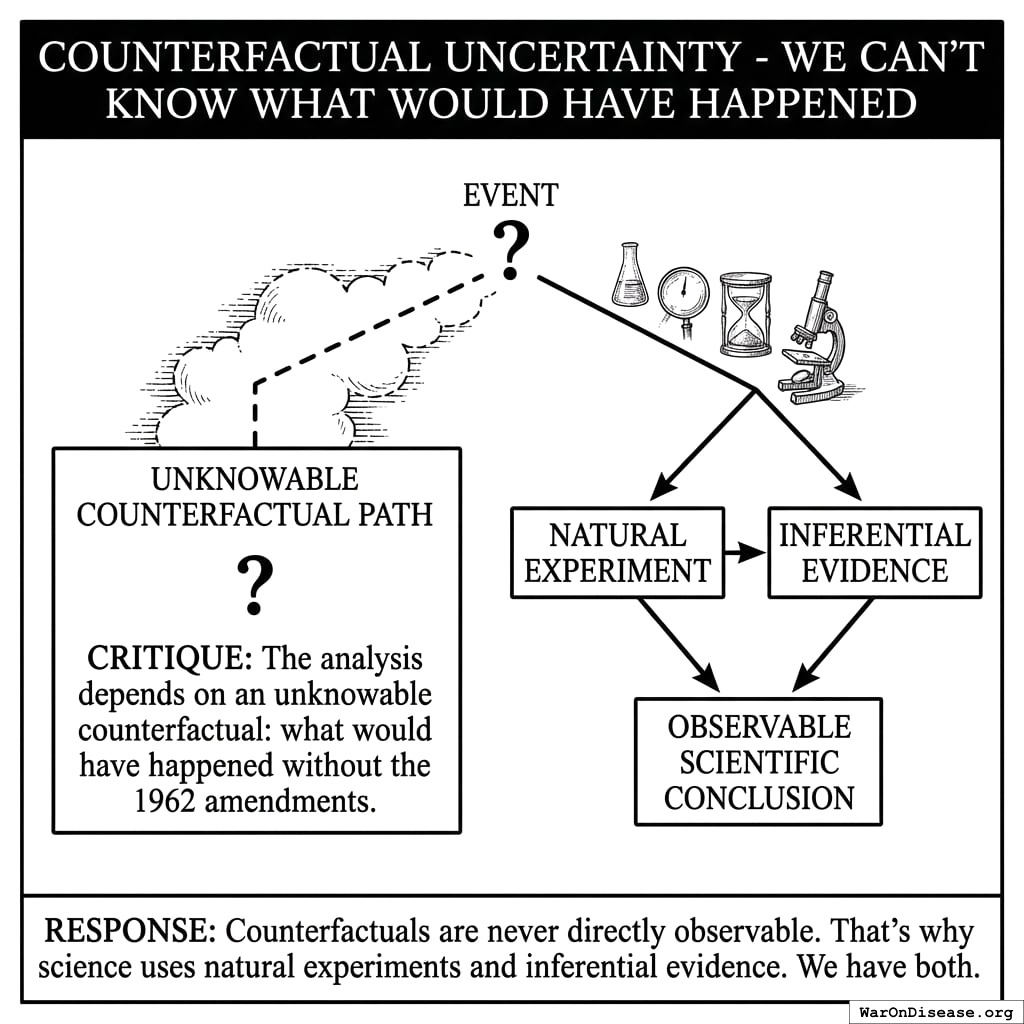
“Counterfactual Uncertainty - We Can’t Know What Would Have Happened”
Critique: The analysis depends on an unknowable counterfactual: what would have happened without the 1962 amendments.
Response:
Counterfactuals are never directly observable. That’s why science uses natural experiments and inferential evidence. We have both.
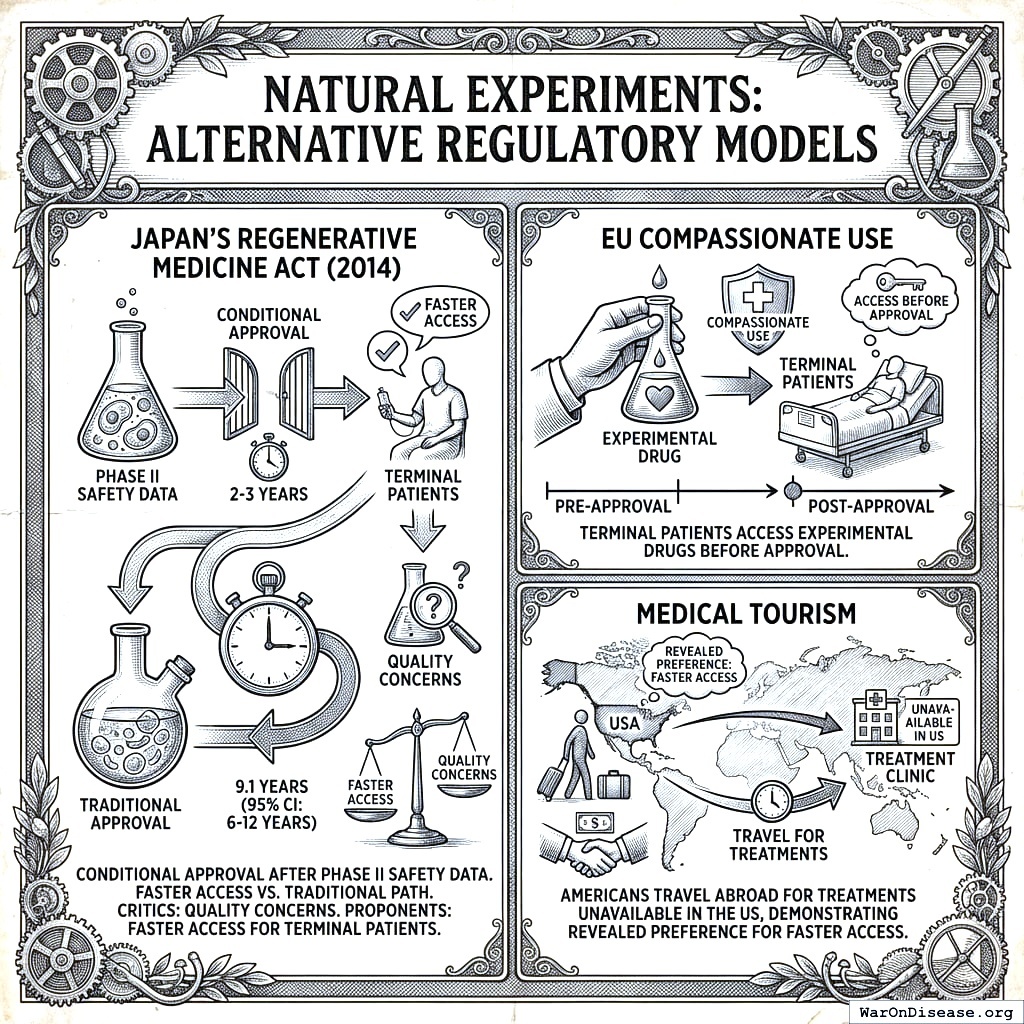
Natural Experiments
Alternative Regulatory Models:
- Japan’s Regenerative Medicine Act (2014): Conditional approval after Phase II safety data, with 2-3 year timelines vs. 10.5 years (95% CI: 6 years-12 years). Critics note quality concerns; proponents note faster access for terminal patients with no alternatives.
- EU Compassionate Use: Terminal patients access experimental drugs before approval
- Medical tourism: Americans travel abroad for treatments unavailable in the US, demonstrating revealed preference for faster access
The Standard for Causal Inference
The same standard used in all clinical research:
\[
\text{Causation} = \text{Temporal Correlation} + \text{Mechanism} + \text{Lack of Alternative Explanations}
\]
We have:
- Temporal correlation: Drug approvals dropped 70% immediately after 1962
- Mechanism: Costs increased 13.4x (95% CI: 11.9x-14.7x), real-world trials banned, efficacy requirements added 8.2 years (95% CI: 4.85 years-11.5 years) to development
- Alternative explanations: Other factors exist (complexity, standards, etc.), but the timing and magnitude strongly suggest regulatory latency is a major contributor
If you reject this inferential method, you must also reject the methodology of clinical trials, which use the identical logical structure.
“Confounding Factors - Other Changes in 1962”
Critique: Medicare (1965), NIH funding changes, Vietnam War, and other 1960s policy shifts confound the analysis. How can we isolate the 1962 amendments’ effect?
Response:
Confounders work against the hypothesis, making the observed effect more remarkable.
Medicare (1965): Expanded healthcare access → should have increased drug demand and development → Yet approvals dropped 70%
NIH Funding: Grew dramatically 1960s-1980s → should have accelerated drug development → Yet approvals dropped 70%
Vietnam War (1965-1973): Primarily affected young males, minimal impact on overall drug development patterns
The temporal precision matters: Drug approval rates dropped 70% in 1962, not 1965 (Medicare) or 1964 (Gulf of Tonkin). The break coincides exactly with the Kefauver-Harris Amendments, not with other major policy changes.
Quantitative test:
If confounders explained the effect, we would expect:
- Gradual change over the 1960s (as various policies took effect)
- Recovery after confounders resolved (e.g., Vietnam War ended 1973)
Instead, we observe:
- Immediate 70% drop in drug approvals in 1962
- Sustained reduction in approval rates for 62+ years
- Development costs increased 13.4x (95% CI: 11.9x-14.7x)
The hypothesis that fits the data is: structural change in drug approval requirements permanently reduced the rate of biomedical progress.
Sensitivity Analysis: What if Regulation Explains Only Part of the Decline?
Even if we concede that non-regulatory factors (complexity, pharmacological saturation, etc.) explain a substantial portion of the approval decline, the conclusion remains robust:
The Type II/Type I ratio would need to drop below 1:1 for the FDA’s approach to be justified on net mortality grounds. Even at 10% regulatory attribution, the ratio remains ~300:1. The conclusion is robust across a wide range of assumptions about confounding.
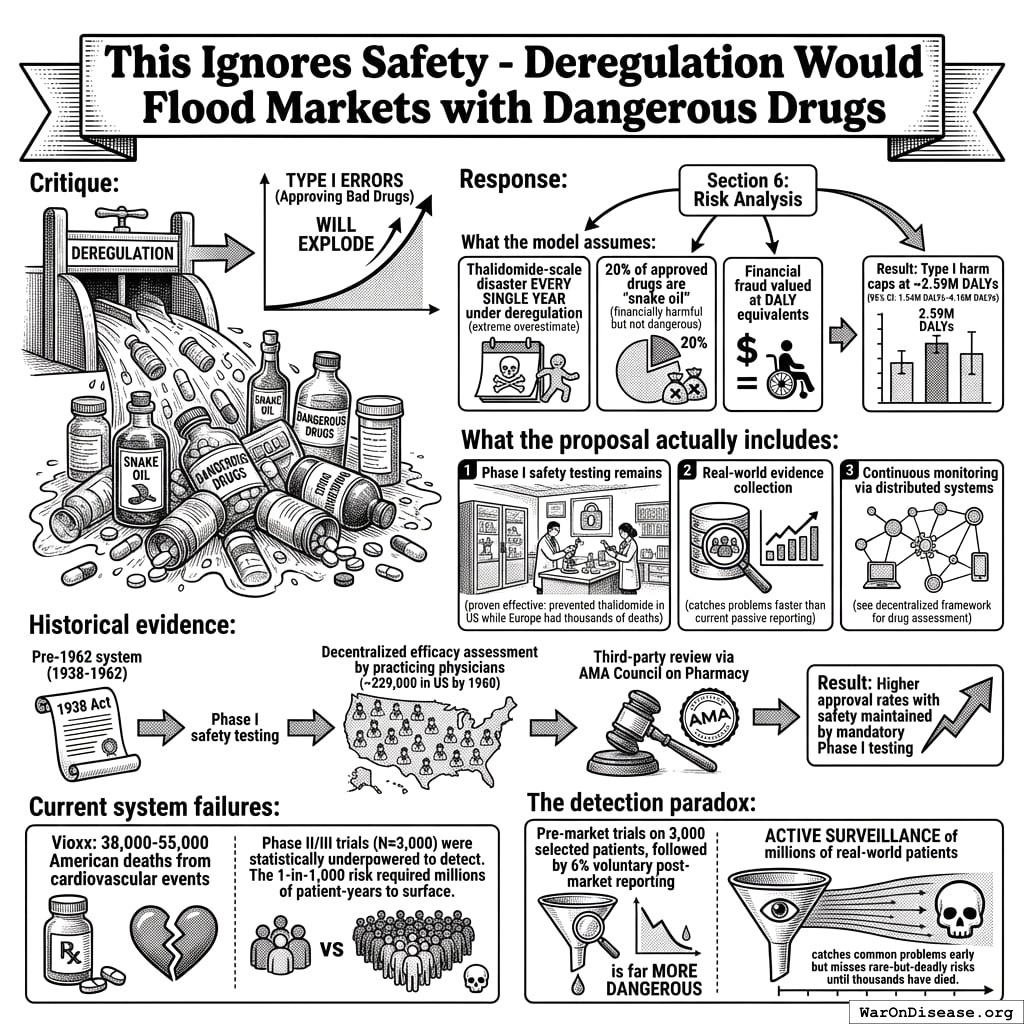
“This Ignores Safety - Deregulation Would Flood Markets with Dangerous Drugs”
Critique: Without efficacy requirements, pharmaceutical companies will sell snake oil and dangerous drugs. Type I errors (approving bad drugs) will explode.
Response:
The analysis explicitly models this in Section 6: Risk Analysis.
What the model assumes:
- Thalidomide-scale disaster every single year under deregulation (extreme overestimate)
- 20% of approved drugs are “snake oil” (financially harmful but not dangerous)
- Financial fraud valued at DALY equivalents
Result: Type I harm caps at ~2.59 million DALYs (95% CI: 1.54 million DALYs-4.16 million DALYs)
What the proposal actually includes:
- Phase I safety testing remains (proven effective: prevented thalidomide in US while Europe had thousands of deaths)
- Real-world evidence collection (catches problems faster than current passive reporting)
- Continuous monitoring via distributed systems (see decentralized FDA)
Historical evidence:
The pre-1962 system (1938-1962) included:
- Phase I safety testing (mandated by 1938 Food, Drug, and Cosmetic Act)
- Decentralized efficacy assessment by practicing physicians (~229,000 in US by 1960)174
- Third-party review via AMA Council on Pharmacy provided independent evaluation
- Result: Higher approval rates with safety maintained by mandatory Phase I testing
Current system failures:
- Vioxx: 38,000-55,000 American deaths163 from cardiovascular events that Phase II/III trials (N≈3,000) were statistically underpowered to detect. The 1-in-1,000 risk required millions of patient-years to surface.
- Statistical reality: Trials with 3,000 patients cannot reliably detect adverse events rarer than ~1-in-1,000
The detection paradox: Pre-market trials on 3,000 selected patients, followed by 6% voluntary post-market reporting, is far more dangerous than active surveillance of millions of real-world patients. The current system catches common problems early but misses rare-but-deadly risks until thousands have died.
Conclusion
The quantitative evidence demonstrates that the 1962 Kefauver-Harris efficacy requirements have generated catastrophic human costs:
The 3,068 (95% CI: 2,878-3,125) ratio demonstrates that these costs dwarf the benefits. The regulatory framework optimizes for bureaucratic risk minimization (avoiding blame for approvals) rather than population health maximization (saving lives).
The path forward is clear: maintain safety testing, eliminate efficacy delay, and deploy distributed real-world evidence systems.
1.
NIH Common Fund. NIH pragmatic trials: Minimal funding despite 30x cost advantage.
NIH Common Fund: HCS Research Collaboratory https://commonfund.nih.gov/hcscollaboratory (2025)
The NIH Pragmatic Trials Collaboratory funds trials at $500K for planning phase, $1M/year for implementation-a tiny fraction of NIH’s budget. The ADAPTABLE trial cost $14 million for 15,076 patients (= $929/patient) versus $420 million for a similar traditional RCT (30x cheaper), yet pragmatic trials remain severely underfunded. PCORnet infrastructure enables real-world trials embedded in healthcare systems, but receives minimal support compared to basic research funding. Additional sources: https://commonfund.nih.gov/hcscollaboratory | https://pcornet.org/wp-content/uploads/2025/08/ADAPTABLE_Lay_Summary_21JUL2025.pdf | https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5604499/
.
2.
Cato Institute. Chance of dying from terrorism statistic.
Cato Institute: Terrorism and Immigration Risk Analysis https://www.cato.org/policy-analysis/terrorism-immigration-risk-analysis Chance of American dying in foreign-born terrorist attack: 1 in 3.6 million per year (1975-2015) Including 9/11 deaths; annual murder rate is 253x higher than terrorism death rate More likely to die from lightning strike than foreign terrorism Note: Comprehensive 41-year study shows terrorism risk is extremely low compared to everyday dangers Additional sources: https://www.cato.org/policy-analysis/terrorism-immigration-risk-analysis | https://www.nbcnews.com/news/us-news/you-re-more-likely-die-choking-be-killed-foreign-terrorists-n715141
.
3.
NIH. Antidepressant clinical trial exclusion rates.
Zimmerman et al. https://pubmed.ncbi.nlm.nih.gov/26276679/ (2015)
Mean exclusion rate: 86.1% across 158 antidepressant efficacy trials (range: 44.4% to 99.8%) More than 82% of real-world depression patients would be ineligible for antidepressant registration trials Exclusion rates increased over time: 91.4% (2010-2014) vs. 83.8% (1995-2009) Most common exclusions: comorbid psychiatric disorders, age restrictions, insufficient depression severity, medical conditions Emergency psychiatry patients: only 3.3% eligible (96.7% excluded) when applying 9 common exclusion criteria Only a minority of depressed patients seen in clinical practice are likely to be eligible for most AETs Note: Generalizability of antidepressant trials has decreased over time, with increasingly stringent exclusion criteria eliminating patients who would actually use the drugs in clinical practice Additional sources: https://pubmed.ncbi.nlm.nih.gov/26276679/ | https://pubmed.ncbi.nlm.nih.gov/26164052/ | https://www.wolterskluwer.com/en/news/antidepressant-trials-exclude-most-real-world-patients-with-depression
.
4.
CNBC. Warren buffett’s career average investment return.
CNBC https://www.cnbc.com/2025/05/05/warren-buffetts-return-tally-after-60-years-5502284percent.html (2025)
Berkshire’s compounded annual return from 1965 through 2024 was 19.9%, nearly double the 10.4% recorded by the S&P 500. Berkshire shares skyrocketed 5,502,284% compared to the S&P 500’s 39,054% rise during that period. Additional sources: https://www.cnbc.com/2025/05/05/warren-buffetts-return-tally-after-60-years-5502284percent.html | https://www.slickcharts.com/berkshire-hathaway/returns
.
5.
World Health Organization. WHO global health estimates 2024.
World Health Organization https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates (2024)
Comprehensive mortality and morbidity data by cause, age, sex, country, and year Global mortality: 55-60 million deaths annually Lives saved by modern medicine (vaccines, cardiovascular drugs, oncology): 12M annually (conservative aggregate) Leading causes of death: Cardiovascular disease (17.9M), Cancer (10.3M), Respiratory disease (4.0M) Note: Baseline data for regulatory mortality analysis. Conservative estimate of pharmaceutical impact based on WHO immunization data (4.5M/year from vaccines) + cardiovascular interventions (3.3M/year) + oncology (1.5M/year) + other therapies. Additional sources: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates
.
6.
GiveWell. GiveWell cost per life saved for top charities (2024).
GiveWell: Top Charities https://www.givewell.org/charities/top-charities General range: $3,000-$5,500 per life saved (GiveWell top charities) Helen Keller International (Vitamin A): $3,500 average (2022-2024); varies $1,000-$8,500 by country Against Malaria Foundation: $5,500 per life saved New Incentives (vaccination incentives): $4,500 per life saved Malaria Consortium (seasonal malaria chemoprevention): $3,500 per life saved VAS program details: $2 to provide vitamin A supplements to child for one year Note: Figures accurate for 2024. Helen Keller VAS program has wide country variation ($1K-$8.5K) but $3,500 is accurate average. Among most cost-effective interventions globally Additional sources: https://www.givewell.org/charities/top-charities | https://www.givewell.org/charities/helen-keller-international | https://ourworldindata.org/cost-effectiveness
.
7.
U.S. Department of Defense.
5.56mm NATO ammunition bulk procurement pricing. (2024)
The cost of 5.56mm NATO ammunition at military bulk procurement rates is approximately $0.40 per round, based on Lake City Army Ammunition Plant production and commercial market floor prices for mil-spec M855 ammunition.
8.
Pike, J.
U.s. Forces fire 250,000 rounds for every insurgent killed. (2011)
The General Accounting Office reports that US forces used 1.8 billion rounds of small-arms ammunition per year, a level that more than doubled in five years. An estimated 250,000 rounds were fired for every insurgent killed in Iraq and Afghanistan.
9.
AARP. Unpaid caregiver hours and economic value.
AARP 2023 https://www.aarp.org/caregiving/financial-legal/info-2023/unpaid-caregivers-provide-billions-in-care.html (2023)
Average family caregiver: 25-26 hours per week (100-104 hours per month) 38 million caregivers providing 36 billion hours of care annually Economic value: $16.59 per hour = $600 billion total annual value (2021) 28% of people provided eldercare on a given day, averaging 3.9 hours when providing care Caregivers living with care recipient: 37.4 hours per week Caregivers not living with recipient: 23.7 hours per week Note: Disease-related caregiving is subset of total; includes elderly care, disability care, and child care Additional sources: https://www.aarp.org/caregiving/financial-legal/info-2023/unpaid-caregivers-provide-billions-in-care.html | https://www.bls.gov/news.release/elcare.nr0.htm | https://www.caregiver.org/resource/caregiver-statistics-demographics/
.
10.
Forbes.
Forbes world’s billionaires list 2024. (2024)
Forbes identified a record 2,781 billionaires worldwide with combined net worth of $14.2 trillion, 141 more than 2023. Bernard Arnault (LVMH) topped the list at $233 billion.
11.
CDC MMWR. Childhood vaccination economic benefits.
CDC MMWR https://www.cdc.gov/mmwr/volumes/73/wr/mm7331a2.htm (1994)
US programs (1994-2023): $540B direct savings, $2.7T societal savings ( $18B/year direct, $90B/year societal) Global (2001-2020): $820B value for 10 diseases in 73 countries ( $41B/year) ROI: $11 return per $1 invested Measles vaccination alone saved 93.7M lives (61% of 154M total) over 50 years (1974-2024) Additional sources: https://www.cdc.gov/mmwr/volumes/73/wr/mm7331a2.htm | https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(24)00850-X/fulltext
.
13.
U.S. Bureau of Labor Statistics.
CPI inflation calculator. (2024)
CPI-U (1980): 82.4 CPI-U (2024): 313.5 Inflation multiplier (1980-2024): 3.80× Cumulative inflation: 280.48% Average annual inflation rate: 3.08% Note: Official U.S. government inflation data using Consumer Price Index for All Urban Consumers (CPI-U). Additional sources: https://www.bls.gov/data/inflation_calculator.htm
.
14.
James Surowiecki.
The Wisdom of Crowds. (Surowiecki, 2004).
Explores the aggregation of information in groups, arguing that decisions are often better than could have been made by any single member of the group. The opening anecdote relates Francis Galton’s surprise that the crowd at a county fair accurately guessed the weight of an ox when the median of their individual guesses was taken. The three conditions for a group to be intelligent are diversity, independence, and decentralization. Additional sources: https://archive.org/details/wisdomofcrowds0000suro | https://en.wikipedia.org/wiki/The_Wisdom_of_Crowds | https://www.amazon.com/Wisdom-Crowds-James-Surowiecki/dp/0385721706
.
15.
ClinicalTrials.gov API v2 direct analysis. ClinicalTrials.gov cumulative enrollment data (2025).
Direct analysis via ClinicalTrials.gov API v2 https://clinicaltrials.gov/data-api/api Analysis of 100,000 active/recruiting/completed trials on ClinicalTrials.gov (as of January 2025) shows cumulative enrollment of 12.2 million participants: Phase 1 (722k), Phase 2 (2.2M), Phase 3 (6.5M), Phase 4 (2.7M). Median participants per trial: Phase 1 (33), Phase 2 (60), Phase 3 (237), Phase 4 (90). Additional sources: https://clinicaltrials.gov/data-api/api
.
16.
ACS CAN. Clinical trial patient participation rate.
ACS CAN: Barriers to Clinical Trial Enrollment https://www.fightcancer.org/policy-resources/barriers-patient-enrollment-therapeutic-clinical-trials-cancer Only 3-5% of adult cancer patients in US receive treatment within clinical trials About 5% of American adults have ever participated in any clinical trial Oncology: 2-3% of all oncology patients participate Contrast: 50-60% enrollment for pediatric cancer trials (<15 years old) Note: 20% of cancer trials fail due to insufficient enrollment; 11% of research sites enroll zero patients Additional sources: https://www.fightcancer.org/policy-resources/barriers-patient-enrollment-therapeutic-clinical-trials-cancer | https://hints.cancer.gov/docs/Briefs/HINTS_Brief_48.pdf
.
17.
ScienceDaily. Global prevalence of chronic disease.
ScienceDaily: GBD 2015 Study https://www.sciencedaily.com/releases/2015/06/150608081753.htm (2015)
2.3 billion individuals had more than five ailments (2013) Chronic conditions caused 74% of all deaths worldwide (2019), up from 67% (2010) Approximately 1 in 3 adults suffer from multiple chronic conditions (MCCs) Risk factor exposures: 2B exposed to biomass fuel, 1B to air pollution, 1B smokers Projected economic cost: $47 trillion by 2030 Note: 2.3B with 5+ ailments is more accurate than "2B with chronic disease." One-third of all adults globally have multiple chronic conditions Additional sources: https://www.sciencedaily.com/releases/2015/06/150608081753.htm | https://pmc.ncbi.nlm.nih.gov/articles/PMC10830426/ | https://pmc.ncbi.nlm.nih.gov/articles/PMC6214883/
.
18.
C&EN. Annual number of new drugs approved globally: 50.
C&EN https://cen.acs.org/pharmaceuticals/50-new-drugs-received-FDA/103/i2 (2025)
50 new drugs approved annually Additional sources: https://cen.acs.org/pharmaceuticals/50-new-drugs-received-FDA/103/i2 | https://www.fda.gov/drugs/development-approval-process-drugs/novel-drug-approvals-fda
.
19.
Williams, R. J., Tse, T., DiPiazza, K. & Zarin, D. A.
Terminated trials in the ClinicalTrials.gov results database: Evaluation of availability of primary outcome data and reasons for termination.
PLOS One 10, e0127242 (2015)
Approximately 12% of trials with results posted on the ClinicalTrials.gov results database (905/7,646) were terminated. Primary reasons: insufficient accrual (57% of non-data-driven terminations), business/strategic reasons, and efficacy/toxicity findings (21% data-driven terminations).
23.
Rummel, R. J.
Death by Government: Genocide and Mass Murder Since 1900. (Transaction Publishers, 1994).
Political scientist R.J. Rummel’s comprehensive accounting of democide (government murder of unarmed civilians) in the 20th century. His final revised estimate: 262 million people murdered by their own governments from 1900-1999, excluding battle deaths in wars. Range: 200-272+ million. Communist regimes account for the largest share (100-148+ million). Updated figures at hawaii.edu/powerkills.
24.
GiveWell. Cost per DALY for deworming programs.
https://www.givewell.org/international/technical/programs/deworming/cost-effectiveness Schistosomiasis treatment: $28.19-$70.48 per DALY (using arithmetic means with varying disability weights) Soil-transmitted helminths (STH) treatment: $82.54 per DALY (midpoint estimate) Note: GiveWell explicitly states this 2011 analysis is "out of date" and their current methodology focuses on long-term income effects rather than short-term health DALYs Additional sources: https://www.givewell.org/international/technical/programs/deworming/cost-effectiveness
.
25.
Calculated from IHME Global Burden of Disease (2.55B DALYs) and global GDP per capita valuation. $109 trillion annual global disease burden.
The global economic burden of disease, including direct healthcare costs ($8.2 trillion) and lost productivity ($100.9 trillion from 2.55 billion DALYs × $39,570 per DALY), totals approximately $109.1 trillion annually.
27.
Think by Numbers. Pre-1962 drug development costs and timeline (think by numbers).
Think by Numbers: How Many Lives Does FDA Save? https://thinkbynumbers.org/health/how-many-net-lives-does-the-fda-save/ (1962)
Historical estimates (1970-1985): USD $226M fully capitalized (2011 prices) 1980s drugs: $65M after-tax R&D (1990 dollars), $194M compounded to approval (1990 dollars) Modern comparison: $2-3B costs, 7-12 years (dramatic increase from pre-1962) Context: 1962 regulatory clampdown reduced new treatment production by 70%, dramatically increasing development timelines and costs Note: Secondary source; less reliable than Congressional testimony Additional sources: https://thinkbynumbers.org/health/how-many-net-lives-does-the-fda-save/ | https://en.wikipedia.org/wiki/Cost_of_drug_development | https://www.statnews.com/2018/10/01/changing-1962-law-slash-drug-prices/
.
28.
Biotechnology Innovation Organization (BIO). BIO clinical development success rates 2011-2020.
Biotechnology Innovation Organization (BIO) https://go.bio.org/rs/490-EHZ-999/images/ClinicalDevelopmentSuccessRates2011_2020.pdf (2021)
Phase I duration: 2.3 years average Total time to market (Phase I-III + approval): 10.5 years average Phase transition success rates: Phase I→II: 63.2%, Phase II→III: 30.7%, Phase III→Approval: 58.1% Overall probability of approval from Phase I: 12% Note: Largest publicly available study of clinical trial success rates. Efficacy lag = 10.5 - 2.3 = 8.2 years post-safety verification. Additional sources: https://go.bio.org/rs/490-EHZ-999/images/ClinicalDevelopmentSuccessRates2011_2020.pdf
.
29.
Nature Medicine. Drug repurposing rate ( 30%).
Nature Medicine https://www.nature.com/articles/s41591-024-03233-x (2024)
Approximately 30% of drugs gain at least one new indication after initial approval. Additional sources: https://www.nature.com/articles/s41591-024-03233-x
.
30.
EPI. Education investment economic multiplier (2.1).
EPI: Public Investments Outside Core Infrastructure https://www.epi.org/publication/bp348-public-investments-outside-core-infrastructure/ Early childhood education: Benefits 12X outlays by 2050; $8.70 per dollar over lifetime Educational facilities: $1 spent → $1.50 economic returns Energy efficiency comparison: 2-to-1 benefit-to-cost ratio (McKinsey) Private return to schooling: 9% per additional year (World Bank meta-analysis) Note: 2.1 multiplier aligns with benefit-to-cost ratios for educational infrastructure/energy efficiency. Early childhood education shows much higher returns (12X by 2050) Additional sources: https://www.epi.org/publication/bp348-public-investments-outside-core-infrastructure/ | https://documents1.worldbank.org/curated/en/442521523465644318/pdf/WPS8402.pdf | https://freopp.org/whitepapers/establishing-a-practical-return-on-investment-framework-for-education-and-skills-development-to-expand-economic-opportunity/
.
31.
PMC. Healthcare investment economic multiplier (1.8).
PMC: California Universal Health Care https://pmc.ncbi.nlm.nih.gov/articles/PMC5954824/ (2022)
Healthcare fiscal multiplier: 4.3 (95% CI: 2.5-6.1) during pre-recession period (1995-2007) Overall government spending multiplier: 1.61 (95% CI: 1.37-1.86) Why healthcare has high multipliers: No effect on trade deficits (spending stays domestic); improves productivity & competitiveness; enhances long-run potential output Gender-sensitive fiscal spending (health & care economy) produces substantial positive growth impacts Note: "1.8" appears to be conservative estimate; research shows healthcare multipliers of 4.3 Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC5954824/ | https://cepr.org/voxeu/columns/government-investment-and-fiscal-stimulus | https://ncbi.nlm.nih.gov/pmc/articles/PMC3849102/ | https://set.odi.org/wp-content/uploads/2022/01/Fiscal-multipliers-review.pdf
.
32.
World Bank. Infrastructure investment economic multiplier (1.6).
World Bank: Infrastructure Investment as Stimulus https://blogs.worldbank.org/en/ppps/effectiveness-infrastructure-investment-fiscal-stimulus-what-weve-learned (2022)
Infrastructure fiscal multiplier: 1.6 during contractionary phase of economic cycle Average across all economic states: 1.5 (meaning $1 of public investment → $1.50 of economic activity) Time horizon: 0.8 within 1 year, 1.5 within 2-5 years Range of estimates: 1.5-2.0 (following 2008 financial crisis & American Recovery Act) Italian public construction: 1.5-1.9 multiplier US ARRA: 0.4-2.2 range (differential impacts by program type) Economic Policy Institute: Uses 1.6 for infrastructure spending (middle range of estimates) Note: Public investment less likely to crowd out private activity during recessions; particularly effective when monetary policy loose with near-zero rates Additional sources: https://blogs.worldbank.org/en/ppps/effectiveness-infrastructure-investment-fiscal-stimulus-what-weve-learned | https://www.gihub.org/infrastructure-monitor/insights/fiscal-multiplier-effect-of-infrastructure-investment/ | https://cepr.org/voxeu/columns/government-investment-and-fiscal-stimulus | https://www.richmondfed.org/publications/research/economic_brief/2022/eb_22-04
.
33.
Mercatus. Military spending economic multiplier (0.6).
Mercatus: Defense Spending and Economy https://www.mercatus.org/research/research-papers/defense-spending-and-economy Ramey (2011): 0.6 short-run multiplier Barro (1981): 0.6 multiplier for WWII spending (war spending crowded out 40¢ private economic activity per federal dollar) Barro & Redlick (2011): 0.4 within current year, 0.6 over two years; increased govt spending reduces private-sector GDP portions General finding: $1 increase in deficit-financed federal military spending = less than $1 increase in GDP Variation by context: Central/Eastern European NATO: 0.6 on impact, 1.5-1.6 in years 2-3, gradual fall to zero Ramey & Zubairy (2018): Cumulative 1% GDP increase in military expenditure raises GDP by 0.7% Additional sources: https://www.mercatus.org/research/research-papers/defense-spending-and-economy | https://cepr.org/voxeu/columns/world-war-ii-america-spending-deficits-multipliers-and-sacrifice | https://www.rand.org/content/dam/rand/pubs/research_reports/RRA700/RRA739-2/RAND_RRA739-2.pdf
.
34.
FDA. FDA-approved prescription drug products (20,000+).
FDA https://www.fda.gov/media/143704/download There are over 20,000 prescription drug products approved for marketing. Additional sources: https://www.fda.gov/media/143704/download
.
36.
ACLED. Active combat deaths annually.
ACLED: Global Conflict Surged 2024 https://acleddata.com/2024/12/12/data-shows-global-conflict-surged-in-2024-the-washington-post/ (2024)
2024: 233,597 deaths (30% increase from 179,099 in 2023) Deadliest conflicts: Ukraine (67,000), Palestine (35,000) Nearly 200,000 acts of violence (25% higher than 2023, double from 5 years ago) One in six people globally live in conflict-affected areas Additional sources: https://acleddata.com/2024/12/12/data-shows-global-conflict-surged-in-2024-the-washington-post/ | https://acleddata.com/media-citation/data-shows-global-conflict-surged-2024-washington-post | https://acleddata.com/conflict-index/index-january-2024/
.
37.
UCDP. State violence deaths annually.
UCDP: Uppsala Conflict Data Program https://ucdp.uu.se/ Uppsala Conflict Data Program (UCDP): Tracks one-sided violence (organized actors attacking unarmed civilians) UCDP definition: Conflicts causing at least 25 battle-related deaths in calendar year 2023 total organized violence: 154,000 deaths; Non-state conflicts: 20,900 deaths UCDP collects data on state-based conflicts, non-state conflicts, and one-sided violence Specific "2,700 annually" figure for state violence not found in recent UCDP data; actual figures vary annually Additional sources: https://ucdp.uu.se/ | https://en.wikipedia.org/wiki/Uppsala_Conflict_Data_Program | https://ourworldindata.org/grapher/deaths-in-armed-conflicts-by-region
.
38.
Our World in Data. Terror attack deaths (8,300 annually).
Our World in Data: Terrorism https://ourworldindata.org/terrorism (2024)
2023: 8,352 deaths (22% increase from 2022, highest since 2017) 2023: 3,350 terrorist incidents (22% decrease), but 56% increase in avg deaths per attack Global Terrorism Database (GTD): 200,000+ terrorist attacks recorded (2021 version) Maintained by: National Consortium for Study of Terrorism & Responses to Terrorism (START), U. of Maryland Geographic shift: Epicenter moved from Middle East to Central Sahel (sub-Saharan Africa) - now >50% of all deaths Additional sources: https://ourworldindata.org/terrorism | https://reliefweb.int/report/world/global-terrorism-index-2024 | https://www.start.umd.edu/gtd/ | https://ourworldindata.org/grapher/fatalities-from-terrorism
.
39.
Institute for Health Metrics and Evaluation (IHME). IHME global burden of disease 2021 (2.88B DALYs, 1.13B YLD).
Institute for Health Metrics and Evaluation (IHME) https://vizhub.healthdata.org/gbd-results/ (2024)
In 2021, global DALYs totaled approximately 2.88 billion, comprising 1.75 billion Years of Life Lost (YLL) and 1.13 billion Years Lived with Disability (YLD). This represents a 13% increase from 2019 (2.55B DALYs), largely attributable to COVID-19 deaths and aging populations. YLD accounts for approximately 39% of total DALYs, reflecting the substantial burden of non-fatal chronic conditions. Additional sources: https://vizhub.healthdata.org/gbd-results/ | https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(24)00757-8/fulltext | https://www.healthdata.org/research-analysis/about-gbd
.
40.
Costs of War Project, Brown University Watson Institute. Environmental cost of war ($100B annually).
Brown Watson Costs of War: Environmental Cost https://watson.brown.edu/costsofwar/costs/social/environment War on Terror emissions: 1.2B metric tons GHG (equivalent to 257M cars/year) Military: 5.5% of global GHG emissions (2X aviation + shipping combined) US DoD: World’s single largest institutional oil consumer, 47th largest emitter if nation Cleanup costs: $500B+ for military contaminated sites Gaza war environmental damage: $56.4B; landmine clearance: $34.6B expected Climate finance gap: Rich nations spend 30X more on military than climate finance Note: Military activities cause massive environmental damage through GHG emissions, toxic contamination, and long-term cleanup costs far exceeding current climate finance commitments Additional sources: https://watson.brown.edu/costsofwar/costs/social/environment | https://earth.org/environmental-costs-of-wars/ | https://transformdefence.org/transformdefence/stats/
.
41.
ScienceDaily. Medical research lives saved annually (4.2 million).
ScienceDaily: Physical Activity Prevents 4M Deaths https://www.sciencedaily.com/releases/2020/06/200617194510.htm (2020)
Physical activity: 3.9M early deaths averted annually worldwide (15% lower premature deaths than without) COVID vaccines (2020-2024): 2.533M deaths averted, 14.8M life-years preserved; first year alone: 14.4M deaths prevented Cardiovascular prevention: 3 interventions could delay 94.3M deaths over 25 years (antihypertensives alone: 39.4M) Pandemic research response: Millions of deaths averted through rapid vaccine/drug development Additional sources: https://www.sciencedaily.com/releases/2020/06/200617194510.htm | https://pmc.ncbi.nlm.nih.gov/articles/PMC9537923/ | https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.118.038160 | https://pmc.ncbi.nlm.nih.gov/articles/PMC9464102/
.
42.
SIPRI. 36:1 disparity ratio of spending on weapons over cures.
SIPRI: Military Spending https://www.sipri.org/commentary/blog/2016/opportunity-cost-world-military-spending (2016)
Global military spending: $2.7 trillion (2024, SIPRI) Global government medical research: $68 billion (2024) Actual ratio: 39.7:1 in favor of weapons over medical research Military R&D alone: $85B (2004 data, 10% of global R&D) Military spending increases crowd out health: 1% ↑ military = 0.62% ↓ health spending Note: Ratio actually worse than 36:1. Each 1% increase in military spending reduces health spending by 0.62%, with effect more intense in poorer countries (0.962% reduction) Additional sources: https://www.sipri.org/commentary/blog/2016/opportunity-cost-world-military-spending | https://pmc.ncbi.nlm.nih.gov/articles/PMC9174441/ | https://www.congress.gov/crs-product/R45403
.
43.
Think by Numbers. Lost human capital due to war ($270B annually).
Think by Numbers https://thinkbynumbers.org/military/war/the-economic-case-for-peace-a-comprehensive-financial-analysis/ (2021)
Lost human capital from war: $300B annually (economic impact of losing skilled/productive individuals to conflict) Broader conflict/violence cost: $14T/year globally 1.4M violent deaths/year; conflict holds back economic development, causes instability, widens inequality, erodes human capital 2002: 48.4M DALYs lost from 1.6M violence deaths = $151B economic value (2000 USD) Economic toll includes: commodity prices, inflation, supply chain disruption, declining output, lost human capital Additional sources: https://thinkbynumbers.org/military/war/the-economic-case-for-peace-a-comprehensive-financial-analysis/ | https://www.weforum.org/stories/2021/02/war-violence-costs-each-human-5-a-day/ | https://pubmed.ncbi.nlm.nih.gov/19115548/
.
44.
PubMed. Psychological impact of war cost ($100B annually).
PubMed: Economic Burden of PTSD https://pubmed.ncbi.nlm.nih.gov/35485933/ PTSD economic burden (2018 U.S.): $232.2B total ($189.5B civilian, $42.7B military) Civilian costs driven by: Direct healthcare ($66B), unemployment ($42.7B) Military costs driven by: Disability ($17.8B), direct healthcare ($10.1B) Exceeds costs of other mental health conditions (anxiety, depression) War-exposed populations: 2-3X higher rates of anxiety, depression, PTSD; women and children most vulnerable Note: Actual burden $232B, significantly higher than "$100B" claimed Additional sources: https://pubmed.ncbi.nlm.nih.gov/35485933/ | https://news.va.gov/103611/study-national-economic-burden-of-ptsd-staggering/ | https://pmc.ncbi.nlm.nih.gov/articles/PMC9957523/
.
45.
CGDev. UNHCR average refugee support cost.
CGDev https://www.cgdev.org/blog/costs-hosting-refugees-oecd-countries-and-why-uk-outlier (2024)
The average cost of supporting a refugee is $1,384 per year. This represents total host country costs (housing, healthcare, education, security). OECD countries average $6,100 per refugee (mean 2022-2023), with developing countries spending $700-1,000. Global weighted average of $1,384 is reasonable given that 75-85% of refugees are in low/middle-income countries. Additional sources: https://www.cgdev.org/blog/costs-hosting-refugees-oecd-countries-and-why-uk-outlier | https://www.unhcr.org/sites/default/files/2024-11/UNHCR-WB-global-cost-of-refugee-inclusion-in-host-country-health-systems.pdf
.
46.
World Bank. World bank trade disruption cost from conflict.
World Bank https://www.worldbank.org/en/topic/trade/publication/trading-away-from-conflict Estimated $616B annual cost from conflict-related trade disruption. World Bank research shows civil war costs an average developing country 30 years of GDP growth, with 20 years needed for trade to return to pre-war levels. Trade disputes analysis shows tariff escalation could reduce global exports by up to $674 billion. Additional sources: https://www.worldbank.org/en/topic/trade/publication/trading-away-from-conflict | https://www.nber.org/papers/w11565 | http://blogs.worldbank.org/en/trade/impacts-global-trade-and-income-current-trade-disputes
.
47.
VA. Veteran healthcare cost projections.
VA https://department.va.gov/wp-content/uploads/2025/06/2026-Budget-in-Brief.pdf (2026)
VA budget: $441.3B requested for FY 2026 (10% increase). Disability compensation: $165.6B in FY 2024 for 6.7M veterans. PACT Act projected to increase spending by $300B between 2022-2031. Costs under Toxic Exposures Fund: $20B (2024), $30.4B (2025), $52.6B (2026). Additional sources: https://department.va.gov/wp-content/uploads/2025/06/2026-Budget-in-Brief.pdf | https://www.cbo.gov/publication/45615 | https://www.legion.org/information-center/news/veterans-healthcare/2025/june/va-budget-tops-400-billion-for-2025-from-higher-spending-on-mandated-benefits-medical-care
.
50.
Cybersecurity Ventures. Cybercrime economy projected to reach $10.5 trillion.
Cybersecurity Ventures: $10.5T Cybercrime https://cybersecurityventures.com/hackerpocalypse-cybercrime-report-2016/ (2016)
Global cybercrime costs: $3T (2015) → $6T (2021) → $10.5T (2025 projected) 15% annual growth rate If measured as country, would be 3rd largest economy after US and China Greatest transfer of economic wealth in history Note: More profitable than global trade of all major illegal drugs combined. Includes data theft, productivity loss, IP theft, fraud Additional sources: <https://cybersecurityventures.com/hackerpocalypse-cybercrime-report-2016/> | https://www.boisestate.edu/cybersecurity/2022/06/16/cybercrime-to-cost-the-world-10-5-trillion-annually-by-2025/
.
52.
Bolt, J. & Zanden, J. L. van.
Maddison project database 2020. (2020)
Historical GDP per capita estimates from year 1 to present. Global GDP per capita in 1900: approximately 1,260 in 1990 international dollars (roughly 3,150 in 2024 USD after PPP and inflation adjustment). Standard reference for long-run comparative economic history.
53.
Applied Clinical Trials. Global government spending on interventional clinical trials: $3-6 billion/year.
Applied Clinical Trials https://www.appliedclinicaltrialsonline.com/view/sizing-clinical-research-market Estimated range based on NIH ( $0.8-5.6B), NIHR ($1.6B total budget), and EU funding ( $1.3B/year). Roughly 5-10% of global market. Additional sources: https://www.appliedclinicaltrialsonline.com/view/sizing-clinical-research-market | https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30357-0/fulltext
.
56.
United Nations Department of Economic and Social Affairs, Population Division.
World population prospects 2024: Summary of results. (2024)
The 2024 Revision of the World Population Prospects provides population estimates and projections for 237 countries or areas. Global median age approximately 30.5 years in 2024, reflecting population-weighted average across all regions.
59.
Estimated from major foundation budgets and activities. Nonprofit clinical trial funding estimate.
Nonprofit foundations spend an estimated $2-5 billion annually on clinical trials globally, representing approximately 2-5% of total clinical trial spending.
60.
ICAN. Global nuclear weapon maintenance cost: $100 billion/year.
ICAN: Global Spending $100B 2024 https://www.icanw.org/global_spending_on_nuclear_weapons_topped_100_billion_in_2024 (2024)
2024: >$100 billion ($190,151/minute) - 11% increase ($9.9B) from 2023 Nine nuclear-armed states: China, France, India, Israel, N. Korea, Pakistan, Russia, UK, US US: $56.8B (more than all other 8 states combined); China: $12.5B; UK: $10B (+26% YoY, biggest increase) Historical trend: $72.9B (2019) → $82.4B (2021) → >$100B (2024) Private sector contracts: $463B ongoing; $42.5B earned from contracts in 2024 alone Note: $100B/year figure accurate for 2024. Rapid growth from $73B (2019). US spends more than rest of world combined on nuclear weapons Additional sources: https://www.icanw.org/global_spending_on_nuclear_weapons_topped_100_billion_in_2024 | https://www.icanw.org/the_cost_of_nuclear_weapons
.
61.
Industry reports: IQVIA. Global pharmaceutical r&d spending.
Total global pharmaceutical R&D spending is approximately $300 billion annually. Clinical trials represent 15-20% of this total ($45-60B), with the remainder going to drug discovery, preclinical research, regulatory affairs, and manufacturing development.
62.
UN. Global population reaches 8 billion.
UN: World Population 8 Billion Nov 15 2022 https://www.un.org/en/desa/world-population-reach-8-billion-15-november-2022 (2022)
Milestone: November 15, 2022 (UN World Population Prospects 2022) Day of Eight Billion" designated by UN Added 1 billion people in just 11 years (2011-2022) Growth rate: Slowest since 1950; fell under 1% in 2020 Future: 15 years to reach 9B (2037); projected peak 10.4B in 2080s Projections: 8.5B (2030), 9.7B (2050), 10.4B (2080-2100 plateau) Note: Milestone reached Nov 2022. Population growth slowing; will take longer to add next billion (15 years vs 11 years) Additional sources: https://www.un.org/en/desa/world-population-reach-8-billion-15-november-2022 | https://www.un.org/en/dayof8billion | https://en.wikipedia.org/wiki/Day_of_Eight_Billion
.
63.
Harvard Kennedy School. 3.5% participation tipping point.
Harvard Kennedy School https://www.hks.harvard.edu/centers/carr/publications/35-rule-how-small-minority-can-change-world (2020)
The research found that nonviolent campaigns were twice as likely to succeed as violent ones, and once 3.5% of the population were involved, they were always successful. Chenoweth and Maria Stephan studied the success rates of civil resistance efforts from 1900 to 2006, finding that nonviolent movements attracted, on average, four times as many participants as violent movements and were more likely to succeed. Key finding: Every campaign that mobilized at least 3.5% of the population in sustained protest was successful (in their 1900-2006 dataset) Note: The 3.5% figure is a descriptive statistic from historical analysis, not a guaranteed threshold. One exception (Bahrain 2011-2014 with 6%+ participation) has been identified. The rule applies to regime change, not policy change in democracies. Additional sources: https://www.hks.harvard.edu/centers/carr/publications/35-rule-how-small-minority-can-change-world | https://www.hks.harvard.edu/sites/default/files/2024-05/Erica%20Chenoweth_2020-005.pdf | https://www.bbc.com/future/article/20190513-it-only-takes-35-of-people-to-change-the-world | https://en.wikipedia.org/wiki/3.5%25_rule
.
64.
International IDEA.
International IDEA voter turnout database world export. (2026)
Best current register-based estimate of global registered voters. Sum of the latest available country-level Registration counts in International IDEA’s world export on 2026-04-22 = 4,128,142,495 registered voters across 199 countries and political entities. Methodology notes that Registration is the number of names on the voters’ register as reported by electoral management bodies, and comparability is imperfect because voter rolls and registration systems differ across countries. Additional sources: https://www.idea.int/data-tools/data/voter-turnout-database | https://www.idea.int/data-tools/export?type=region_only&themeId=293&world=all&loc=home
.
66.
Federation of American Scientists. World nuclear forces.
Federation of American Scientists https://fas.org/issues/nuclear-weapons/status-world-nuclear-forces/ (2024)
As of early 2025, we estimate that the world’s nine nuclear-armed states possess a combined total of approximately 12,241 nuclear warheads. Additional sources: https://fas.org/issues/nuclear-weapons/status-world-nuclear-forces/
.
67.
NHGRI. Human genome project and CRISPR discovery.
NHGRI https://www.genome.gov/11006929/2003-release-international-consortium-completes-hgp (2003)
Your DNA is 3 billion base pairs Read the entire code (Human Genome Project, completed 2003) Learned to edit it (CRISPR, discovered 2012) Additional sources: https://www.genome.gov/11006929/2003-release-international-consortium-completes-hgp | https://www.nobelprize.org/prizes/chemistry/2020/press-release/
.
68.
PMC. Only 12% of human interactome targeted.
PMC https://pmc.ncbi.nlm.nih.gov/articles/PMC10749231/ (2023)
Mapping 350,000+ clinical trials showed that only 12% of the human interactome has ever been targeted by drugs. Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC10749231/
.
69.
WHO. ICD-10 code count ( 14,000).
WHO https://icd.who.int/browse10/2019/en (2019)
The ICD-10 classification contains approximately 14,000 codes for diseases, signs and symptoms. Additional sources: https://icd.who.int/browse10/2019/en
.
70.
Wikipedia. Longevity escape velocity (LEV) - maximum human life extension potential.
Wikipedia: Longevity Escape Velocity https://en.wikipedia.org/wiki/Longevity_escape_velocity Longevity escape velocity: Hypothetical point where medical advances extend life expectancy faster than time passes Term coined by Aubrey de Grey (biogerontologist) in 2004 paper; concept from David Gobel (Methuselah Foundation) Current progress: Science adds 3 months to lifespan per year; LEV requires adding >1 year per year Sinclair (Harvard): "There is no biological upper limit to age" - first person to live to 150 may already be born De Grey: 50% chance of reaching LEV by mid-to-late 2030s; SENS approach = damage repair rather than slowing damage Kurzweil (2024): LEV by 2029-2035, AI will simulate biological processes to accelerate solutions George Church: LEV "in a decade or two" via age-reversal clinical trials Natural lifespan cap: 120-150 years (Jeanne Calment record: 122); engineering approach could bypass via damage repair Key mechanisms: Epigenetic reprogramming, senolytic drugs, stem cell therapy, gene therapy, AI-driven drug discovery Current record: Jeanne Calment (122 years, 164 days) - record unbroken since 1997 Note: LEV is theoretical but increasingly plausible given demonstrated age reversal in mice (109% lifespan extension) and human cells (30-year epigenetic age reversal) Additional sources: https://en.wikipedia.org/wiki/Longevity_escape_velocity | https://pmc.ncbi.nlm.nih.gov/articles/PMC423155/ | https://www.popularmechanics.com/science/a36712084/can-science-cure-death-longevity/ | https://www.diamandis.com/blog/longevity-escape-velocity
.
71.
OpenSecrets. Lobbyist statistics for washington d.c.
OpenSecrets: Lobbying in US https://en.wikipedia.org/wiki/Lobbying_in_the_United_States Registered lobbyists: Over 12,000 (some estimates); 12,281 registered (2013) Former government employees as lobbyists: 2,200+ former federal employees (1998-2004), including 273 former White House staffers, 250 former Congress members & agency heads Congressional revolving door: 43% (86 of 198) lawmakers who left 1998-2004 became lobbyists; currently 59% leaving to private sector work for lobbying/consulting firms/trade groups Executive branch: 8% were registered lobbyists at some point before/after government service Additional sources: https://en.wikipedia.org/wiki/Lobbying_in_the_United_States | https://www.opensecrets.org/revolving-door | https://www.citizen.org/article/revolving-congress/ | https://www.propublica.org/article/we-found-a-staggering-281-lobbyists-whove-worked-in-the-trump-administration
.
72.
MDPI Vaccines. Measles vaccination ROI.
MDPI Vaccines https://www.mdpi.com/2076-393X/12/11/1210 (2024)
Single measles vaccination: 167:1 benefit-cost ratio. MMR (measles-mumps-rubella) vaccination: 14:1 ROI. Historical US elimination efforts (1966-1974): benefit-cost ratio of 10.3:1 with net benefits exceeding USD 1.1 billion (1972 dollars, or USD 8.0 billion in 2023 dollars). 2-dose MMR programs show direct benefit/cost ratio of 14.2 with net savings of $5.3 billion, and 26.0 from societal perspectives with net savings of $11.6 billion. Additional sources: https://www.mdpi.com/2076-393X/12/11/1210 | https://www.tandfonline.com/doi/full/10.1080/14760584.2024.2367451
.
76.
Calculated from Orphanet Journal of Rare Diseases (2024). Diseases getting first effective treatment each year.
Calculated from Orphanet Journal of Rare Diseases (2024) https://ojrd.biomedcentral.com/articles/10.1186/s13023-024-03398-1 (2024)
Under the current system, approximately 10-15 diseases per year receive their FIRST effective treatment. Calculation: 5% of 7,000 rare diseases ( 350) have FDA-approved treatment, accumulated over 40 years of the Orphan Drug Act = 9 rare diseases/year. Adding 5-10 non-rare diseases that get first treatments yields 10-20 total. FDA approves 50 drugs/year, but many are for diseases that already have treatments (me-too drugs, second-line therapies). Only 15 represent truly FIRST treatments for previously untreatable conditions.
77.
NIH. NIH budget (FY 2025).
NIH https://www.nih.gov/about-nih/organization/budget (2024)
The budget total of $47.7 billion also includes $1.412 billion derived from PHS Evaluation financing... Additional sources: https://www.nih.gov/about-nih/organization/budget | https://officeofbudget.od.nih.gov/
.
78.
Bentley et al. NIH spending on clinical trials: 3.3%.
Bentley et al. https://pmc.ncbi.nlm.nih.gov/articles/PMC10349341/ (2023)
NIH spent $8.1 billion on clinical trials for approved drugs (2010-2019), representing 3.3% of relevant NIH spending. Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC10349341/ | https://catalyst.harvard.edu/news/article/nih-spent-8-1b-for-phased-clinical-trials-of-drugs-approved-2010-19-10-of-reported-industry-spending/
.
79.
PMC. Standard medical research ROI ($20k-$100k/QALY).
PMC: Cost-effectiveness Thresholds Used by Study Authors https://pmc.ncbi.nlm.nih.gov/articles/PMC10114019/ (1990)
Typical cost-effectiveness thresholds for medical interventions in rich countries range from $50,000 to $150,000 per QALY. The Institute for Clinical and Economic Review (ICER) uses a $100,000-$150,000/QALY threshold for value-based pricing. Between 1990-2021, authors increasingly cited $100,000 (47% by 2020-21) or $150,000 (24% by 2020-21) per QALY as benchmarks for cost-effectiveness. Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC10114019/ | https://icer.org/our-approach/methods-process/cost-effectiveness-the-qaly-and-the-evlyg/
.
80.
Xia et al., Nature Food. Nuclear winter famine.
Xia et al. https://www.nature.com/articles/s43016-022-00573-0 (2022)
We estimate that a nuclear war between the United States and Russia would produce 150 Tg of soot and lead to 5 billion people dying at the end of year 2. Additional sources: https://www.nature.com/articles/s43016-022-00573-0
.
81.
Manhattan Institute. RECOVERY trial 82× cost reduction.
Manhattan Institute: Slow Costly Trials https://manhattan.institute/article/slow-costly-clinical-trials-drag-down-biomedical-breakthroughs RECOVERY trial: $500 per patient ($20M for 48,000 patients = $417/patient) Typical clinical trial: $41,000 median per-patient cost Cost reduction: 80-82× cheaper ($41,000 ÷ $500 ≈ 82×) Efficiency: $50 per patient per answer (10 therapeutics tested, 4 effective) Dexamethasone estimated to save >630,000 lives Additional sources: https://manhattan.institute/article/slow-costly-clinical-trials-drag-down-biomedical-breakthroughs | https://pmc.ncbi.nlm.nih.gov/articles/PMC9293394/
.
82.
Trials. Patient willingness to participate in clinical trials.
Trials: Patients’ Willingness Survey https://trialsjournal.biomedcentral.com/articles/10.1186/s13063-015-1105-3 Recent surveys: 49-51% willingness (2020-2022) - dramatic drop from 85% (2019) during COVID-19 pandemic Cancer patients when approached: 88% consented to trials (Royal Marsden Hospital) Study type variation: 44.8% willing for drug trial, 76.2% for diagnostic study Top motivation: "Learning more about my health/medical condition" (67.4%) Top barrier: "Worry about experiencing side effects" (52.6%) Additional sources: https://trialsjournal.biomedcentral.com/articles/10.1186/s13063-015-1105-3 | https://www.appliedclinicaltrialsonline.com/view/industry-forced-to-rethink-patient-participation-in-trials | https://pmc.ncbi.nlm.nih.gov/articles/PMC7183682/
.
83.
The Commune. Pentagon audit failures ($2.46T unaccounted).
The Commune https://thecommunemag.com/the-pentagon-misplaced-2-46-trillion-an-in-depth-look-at-the-financial-audit-failures (2024)
In the most recent audit, the Department of Defense (DoD) could not account for approximately 60% of its \(4.1 trillion in assets, amounting to\)2.46 trillion unaccounted for. Alternative title: Pentagon unsupported accounting adjustments (\(6.5T, single year, US Army) In 2015, the Department of Defense's Inspector General reported that the Army could not adequately support\)6.5 trillion in year-end adjustments, indicating severe accounting discrepancies. Additional sources: https://thecommunemag.com/the-pentagon-misplaced-2-46-trillion-an-in-depth-look-at-the-financial-audit-failures | https://accmag.com/audit-pentagon-cannot-account-for-6-5-trillion-dollars-is-taxpayer-money/
.
84.
Tufts CSDD. Cost of drug development.
Various estimates suggest $1.0 - $2.5 billion to bring a new drug from discovery through FDA approval, spread across 10 years. Tufts Center for the Study of Drug Development often cited for $1.0 - $2.6 billion/drug. Industry reports (IQVIA, Deloitte) also highlight $2+ billion figures.
85.
Value in Health. Average lifetime revenue per successful drug.
Value in Health: Sales Revenues for New Therapeutic Agents https://www.sciencedirect.com/science/article/pii/S1098301524027542 Study of 361 FDA-approved drugs from 1995-2014 (median follow-up 13.2 years): Mean lifetime revenue: $15.2 billion per drug Median lifetime revenue: $6.7 billion per drug Revenue after 5 years: $3.2 billion (mean) Revenue after 10 years: $9.5 billion (mean) Revenue after 15 years: $19.2 billion (mean) Distribution highly skewed: top 25 drugs (7%) accounted for 38% of total revenue ($2.1T of $5.5T) Additional sources: https://www.sciencedirect.com/science/article/pii/S1098301524027542
.
86.
Lichtenberg, F. R.
How many life-years have new drugs saved? A three-way fixed-effects analysis of 66 diseases in 27 countries, 2000-2013.
International Health 11, 403–416 (2019)
Using 3-way fixed-effects methodology (disease-country-year) across 66 diseases in 22 countries, this study estimates that drugs launched after 1981 saved 148.7 million life-years in 2013 alone. The regression coefficients for drug launches 0-11 years prior (beta=-0.031, SE=0.008) and 12+ years prior (beta=-0.057, SE=0.013) on years of life lost are highly significant (p<0.0001). Confidence interval for life-years saved: 79.4M-239.8M (95 percent CI) based on propagated standard errors from Table 2.
87.
Deloitte. Pharmaceutical r&d return on investment (ROI).
Deloitte: Measuring Pharmaceutical Innovation 2025 https://www.deloitte.com/ch/en/Industries/life-sciences-health-care/research/measuring-return-from-pharmaceutical-innovation.html (2025)
Deloitte’s annual study of top 20 pharma companies by R&D spend (2010-2024): 2024 ROI: 5.9% (second year of growth after decade of decline) 2023 ROI: 4.3% (estimated from trend) 2022 ROI: 1.2% (historic low since study began, 13-year low) 2021 ROI: 6.8% (record high, inflated by COVID-19 vaccines/treatments) Long-term trend: Declining for over a decade before 2023 recovery Average R&D cost per asset: $2.3B (2022), $2.23B (2024) These returns (1.2-5.9% range) fall far below typical corporate ROI targets (15-20%) Additional sources: https://www.deloitte.com/ch/en/Industries/life-sciences-health-care/research/measuring-return-from-pharmaceutical-innovation.html | https://www.prnewswire.com/news-releases/deloittes-13th-annual-pharmaceutical-innovation-report-pharma-rd-return-on-investment-falls-in-post-pandemic-market-301738807.html | https://hitconsultant.net/2023/02/16/pharma-rd-roi-falls-to-lowest-level-in-13-years/
.
88.
Nature Reviews Drug Discovery. Drug trial success rate from phase i to approval.
Nature Reviews Drug Discovery: Clinical Success Rates https://www.nature.com/articles/nrd.2016.136 (2016)
Overall Phase I to approval: 10-12.8% (conventional wisdom 10%, studies show 12.8%) Recent decline: Average LOA now 6.7% for Phase I (2014-2023 data) Leading pharma companies: 14.3% average LOA (range 8-23%) Varies by therapeutic area: Oncology 3.4%, CNS/cardiovascular lowest at Phase III Phase-specific success: Phase I 47-54%, Phase II 28-34%, Phase III 55-70% Note: 12% figure accurate for historical average. Recent data shows decline to 6.7%, with Phase II as primary attrition point (28% success) Additional sources: https://www.nature.com/articles/nrd.2016.136 | https://pmc.ncbi.nlm.nih.gov/articles/PMC6409418/ | https://academic.oup.com/biostatistics/article/20/2/273/4817524
.
89.
SofproMed. Phase 3 cost per trial range.
SofproMed https://www.sofpromed.com/how-much-does-a-clinical-trial-cost Phase 3 clinical trials cost between $20 million and $282 million per trial, with significant variation by therapeutic area and trial complexity. Additional sources: https://www.sofpromed.com/how-much-does-a-clinical-trial-cost | https://www.cbo.gov/publication/57126
.
90.
Ramsberg, J. & Platt, R. Pragmatic trial cost per patient (median $97).
Learning Health Systems https://pmc.ncbi.nlm.nih.gov/articles/PMC6508852/ (2018)
Meta-analysis of 108 embedded pragmatic clinical trials (2006-2016). The median cost per patient was $97 (IQR $19–$478), based on 2015 dollars. 25% of trials cost <$19/patient; 10 trials exceeded $1,000/patient. U.S. studies median $187 vs non-U.S. median $27. Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC6508852/
.
91.
WHO. Polio vaccination ROI.
WHO https://www.who.int/news-room/feature-stories/detail/sustaining-polio-investments-offers-a-high-return (2019)
For every dollar spent, the return on investment is nearly US$ 39." Total investment cost of US$ 7.5 billion generates projected economic and social benefits of US$ 289.2 billion from sustaining polio assets and integrating them into expanded immunization, surveillance and emergency response programmes across 8 priority countries (Afghanistan, Iraq, Libya, Pakistan, Somalia, Sudan, Syria, Yemen). Additional sources: https://www.who.int/news-room/feature-stories/detail/sustaining-polio-investments-offers-a-high-return
.
92.
ICRC. International campaign to ban landmines (ICBL) - ottawa treaty (1997).
ICRC https://www.icrc.org/en/doc/resources/documents/article/other/57jpjn.htm (1997)
ICBL: Founded 1992 by 6 NGOs (Handicap International, Human Rights Watch, Medico International, Mines Advisory Group, Physicians for Human Rights, Vietnam Veterans of America Foundation) Started with ONE staff member: Jody Williams as founding coordinator Grew to 1,000+ organizations in 60 countries by 1997 Ottawa Process: 14 months (October 1996 - December 1997) Convention signed by 122 states on December 3, 1997; entered into force March 1, 1999 Achievement: Nobel Peace Prize 1997 (shared by ICBL and Jody Williams) Government funding context: Canada established $100M CAD Canadian Landmine Fund over 10 years (1997); International donors provided $169M in 1997 for mine action (up from $100M in 1996) Additional sources: https://www.icrc.org/en/doc/resources/documents/article/other/57jpjn.htm | https://en.wikipedia.org/wiki/International_Campaign_to_Ban_Landmines | https://www.nobelprize.org/prizes/peace/1997/summary/ | https://un.org/press/en/1999/19990520.MINES.BRF.html | https://www.the-monitor.org/en-gb/reports/2003/landmine-monitor-2003/mine-action-funding.aspx
.
93.
OpenSecrets.
Revolving door: Former members of congress. (2024)
388 former members of Congress are registered as lobbyists. Nearly 5,400 former congressional staffers have left Capitol Hill to become federal lobbyists in the past 10 years. Additional sources: https://www.opensecrets.org/revolving-door
.
94.
Kinch, M. S. & Griesenauer, R. H.
Lost medicines: A longer view of the pharmaceutical industry with the potential to reinvigorate discovery.
Drug Discovery Today 24, 875–880 (2019)
Research identified 1,600+ medicines available in 1962. The 1950s represented industry high-water mark with >30 new products in five of ten years; this rate would not be replicated until late 1990s. More than half (880) of these medicines were lost following implementation of Kefauver-Harris Amendment. The peak of 1962 would not be seen again until early 21st century. By 2016 number of organizations actively involved in R&D at level not seen since 1914.
95.
Baily, M. N. Pre-1962 drug development costs (baily 1972).
Baily (1972) https://samizdathealth.org/wp-content/uploads/2020/12/hlthaff.1.2.6.pdf (1972)
Pre-1962: Average cost per new chemical entity (NCE) was $6.5 million (1980 dollars) Inflation-adjusted to 2024 dollars: $6.5M (1980) ≈ $22.5M (2024), using CPI multiplier of 3.46× Real cost increase (inflation-adjusted): $22.5M (pre-1962) → $2,600M (2024) = 116× increase Note: This represents the most comprehensive academic estimate of pre-1962 drug development costs based on empirical industry data Additional sources: https://samizdathealth.org/wp-content/uploads/2020/12/hlthaff.1.2.6.pdf
.
96.
Think by Numbers. Pre-1962 physician-led clinical trials.
Think by Numbers: How Many Lives Does FDA Save? https://thinkbynumbers.org/health/how-many-net-lives-does-the-fda-save/ (1966)
Pre-1962: Physicians could report real-world evidence directly 1962 Drug Amendments replaced "premarket notification" with "premarket approval", requiring extensive efficacy testing Impact: New regulatory clampdown reduced new treatment production by 70%; lifespan growth declined from 4 years/decade to 2 years/decade Drug Efficacy Study Implementation (DESI): NAS/NRC evaluated 3,400+ drugs approved 1938-1962 for safety only; reviewed >3,000 products, >16,000 therapeutic claims FDA has had authority to accept real-world evidence since 1962, clarified by 21st Century Cures Act (2016) Note: Specific "144,000 physicians" figure not verified in sources Additional sources: https://thinkbynumbers.org/health/how-many-net-lives-does-the-fda-save/ | https://www.fda.gov/drugs/enforcement-activities-fda/drug-efficacy-study-implementation-desi | http://www.nasonline.org/about-nas/history/archives/collections/des-1966-1969-1.html
.
97.
GAO. 95% of diseases have 0 FDA-approved treatments.
GAO https://www.gao.gov/products/gao-25-106774 (2025)
95% of diseases have no treatment Additional sources: https://www.gao.gov/products/gao-25-106774 | https://globalgenes.org/rare-disease-facts/
.
99.
NHS England; Águas et al. RECOVERY trial global lives saved ( 1 million).
NHS England: 1 Million Lives Saved https://www.england.nhs.uk/2021/03/covid-treatment-developed-in-the-nhs-saves-a-million-lives/ (2021)
Dexamethasone saved 1 million lives worldwide (NHS England estimate, March 2021, 9 months after discovery). UK alone: 22,000 lives saved. Methodology: Águas et al. Nature Communications 2021 estimated 650,000 lives (range: 240,000-1,400,000) for July-December 2020 alone, based on RECOVERY trial mortality reductions (36% for ventilated, 18% for oxygen-only patients) applied to global COVID hospitalizations. June 2020 announcement: Dexamethasone reduced deaths by up to 1/3 (ventilated patients), 1/5 (oxygen patients). Impact immediate: Adopted into standard care globally within hours of announcement. Additional sources: https://www.england.nhs.uk/2021/03/covid-treatment-developed-in-the-nhs-saves-a-million-lives/ | https://www.nature.com/articles/s41467-021-21134-2 | https://pharmaceutical-journal.com/article/news/steroid-has-saved-the-lives-of-one-million-covid-19-patients-worldwide-figures-show | https://www.recoverytrial.net/news/recovery-trial-celebrates-two-year-anniversary-of-life-saving-dexamethasone-result
.
100.
National September 11 Memorial & Museum.
September 11 attack facts. (2024)
2,977 people were killed in the September 11, 2001 attacks: 2,753 at the World Trade Center, 184 at the Pentagon, and 40 passengers and crew on United Flight 93 in Shanksville, Pennsylvania.
101.
World Bank. World bank singapore economic data.
World Bank https://data.worldbank.org/country/singapore (2024)
Singapore GDP per capita (2023): $82,000 - among highest in the world Government spending: 15% of GDP (vs US 38%) Life expectancy: 84.1 years (vs US 77.5 years) Singapore demonstrates that low government spending can coexist with excellent outcomes Additional sources: https://data.worldbank.org/country/singapore
.
102.
International Monetary Fund.
IMF singapore government spending data. (2024)
Singapore government spending is approximately 15% of GDP This is 23 percentage points lower than the United States (38%) Despite lower spending, Singapore achieves excellent outcomes: - Life expectancy: 84.1 years (vs US 77.5) - Low crime, world-class infrastructure, AAA credit rating Additional sources: https://www.imf.org/en/Countries/SGP
.
103.
World Health Organization.
WHO life expectancy data by country. (2024)
Life expectancy at birth varies significantly among developed nations: Switzerland: 84.0 years (2023) Singapore: 84.1 years (2023) Japan: 84.3 years (2023) United States: 77.5 years (2023) - 6.5 years below Switzerland, Singapore Global average: 73 years Note: US spends more per capita on healthcare than any other nation, yet achieves lower life expectancy Additional sources: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates/ghe-life-expectancy-and-healthy-life-expectancy
.
105.
PMC. Contribution of smoking reduction to life expectancy gains.
PMC: Benefits Smoking Cessation Longevity https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1447499/ (2012)
Population-level: Up to 14% (9% men, 14% women) of total life expectancy gain since 1960 due to tobacco control efforts Individual cessation benefits: Quitting at age 35 adds 6.9-8.5 years (men), 6.1-7.7 years (women) vs continuing smokers By cessation age: Age 25-34 = 10 years gained; age 35-44 = 9 years; age 45-54 = 6 years; age 65 = 2.0 years (men), 3.7 years (women) Cessation before age 40: Reduces death risk by 90% Long-term cessation: 10+ years yields survival comparable to never smokers, averts 10 years of life lost Recent cessation: <3 years averts 5 years of life lost Additional sources: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1447499/ | https://www.cdc.gov/pcd/issues/2012/11_0295.htm | https://www.ajpmonline.org/article/S0749-3797(24)00217-4/fulltext | https://www.nejm.org/doi/full/10.1056/NEJMsa1211128
.
106.
ICER. Value per QALY (standard economic value).
ICER https://icer.org/wp-content/uploads/2024/02/Reference-Case-4.3.25.pdf (2024)
Standard economic value per QALY: $100,000–$150,000. This is the US and global standard willingness-to-pay threshold for interventions that add costs. Dominant interventions (those that save money while improving health) are favorable regardless of this threshold. Additional sources: https://icer.org/wp-content/uploads/2024/02/Reference-Case-4.3.25.pdf
.
107.
GAO. Annual cost of u.s. Sugar subsidies.
GAO: Sugar Program https://www.gao.gov/products/gao-24-106144 Consumer costs: $2.5-3.5 billion per year (GAO estimate) Net economic cost: $1 billion per year 2022: US consumers paid 2X world price for sugar Program costs $3-4 billion/year but no federal budget impact (costs passed directly to consumers via higher prices) Employment impact: 10,000-20,000 manufacturing jobs lost annually in sugar-reliant industries (confectionery, etc.) Multiple studies confirm: Sweetener Users Association ($2.9-3.5B), AEI ($2.4B consumer cost), Beghin & Elobeid ($2.9-3.5B consumer surplus) Additional sources: https://www.gao.gov/products/gao-24-106144 | https://www.heritage.org/agriculture/report/the-us-sugar-program-bad-consumers-bad-agriculture-and-bad-america | https://www.aei.org/articles/the-u-s-spends-4-billion-a-year-subsidizing-stalinist-style-domestic-sugar-production/
.
108.
World Bank. Swiss military budget as percentage of GDP.
World Bank: Military Expenditure https://data.worldbank.org/indicator/MS.MIL.XPND.GD.ZS?locations=CH 2023: 0.70272% of GDP (World Bank) 2024: CHF 5.95 billion official military spending When including militia system costs: 1% GDP (CHF 8.75B) Comparison: Near bottom in Europe; only Ireland, Malta, Moldova spend less (excluding microstates with no armies) Additional sources: https://data.worldbank.org/indicator/MS.MIL.XPND.GD.ZS?locations=CH | https://www.avenir-suisse.ch/en/blog-defence-spending-switzerland-is-in-better-shape-than-it-seems/ | https://tradingeconomics.com/switzerland/military-expenditure-percent-of-gdp-wb-data.html
.
109.
World Bank. Switzerland vs. US GDP per capita comparison.
World Bank: Switzerland GDP Per Capita https://data.worldbank.org/indicator/NY.GDP.PCAP.CD?locations=CH 2024 GDP per capita (PPP-adjusted): Switzerland $93,819 vs United States $75,492 Switzerland’s GDP per capita 24% higher than US when adjusted for purchasing power parity Nominal 2024: Switzerland $103,670 vs US $85,810 Additional sources: https://data.worldbank.org/indicator/NY.GDP.PCAP.CD?locations=CH | https://tradingeconomics.com/switzerland/gdp-per-capita-ppp | https://www.theglobaleconomy.com/USA/gdp_per_capita_ppp/
.
110.
OECD.
OECD government spending as percentage of GDP. (2024)
OECD government spending data shows significant variation among developed nations: United States: 38.0% of GDP (2023) Switzerland: 35.0% of GDP - 3 percentage points lower than US Singapore: 15.0% of GDP - 23 percentage points lower than US (per IMF data) OECD average: approximately 40% of GDP Additional sources: https://data.oecd.org/gga/general-government-spending.htm
.
111.
OECD.
OECD median household income comparison. (2024)
Median household disposable income varies significantly across OECD nations: United States: $77,500 (2023) Switzerland: $55,000 PPP-adjusted (lower nominal but comparable purchasing power) Singapore: $75,000 PPP-adjusted Additional sources: https://data.oecd.org/hha/household-disposable-income.htm
.
112.
Wikipedia. Thalidomide scandal: Worldwide cases and mortality.
Wikipedia https://en.wikipedia.org/wiki/Thalidomide_scandal The total number of embryos affected by the use of thalidomide during pregnancy is estimated at 10,000, of whom about 40% died around the time of birth. More than 10,000 children in 46 countries were born with deformities such as phocomelia. Additional sources: https://en.wikipedia.org/wiki/Thalidomide_scandal
.
113.
PLOS One. Health and quality of life of thalidomide survivors as they age.
PLOS One https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0210222 (2019)
Study of thalidomide survivors documenting ongoing disability impacts, quality of life, and long-term health outcomes. Survivors (now in their 60s) continue to experience significant disability from limb deformities, organ damage, and other effects. Additional sources: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0210222
.
115.
FDA Study via NCBI. Trial costs, FDA study.
FDA Study via NCBI https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6248200/ Overall, the 138 clinical trials had an estimated median (IQR) cost of $19.0 million ($12.2 million-$33.1 million)... The clinical trials cost a median (IQR) of $41,117 ($31,802-$82,362) per patient. Additional sources: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6248200/
.
116.
GBD 2019 Diseases and Injuries Collaborators.
Global burden of disease study 2019: Disability weights.
The Lancet 396, 1204–1222 (2020)
Disability weights for 235 health states used in Global Burden of Disease calculations. Weights range from 0 (perfect health) to 1 (death equivalent). Chronic conditions like diabetes (0.05-0.35), COPD (0.04-0.41), depression (0.15-0.66), and cardiovascular disease (0.04-0.57) show substantial variation by severity. Treatment typically reduces disability weights by 50-80 percent for manageable chronic conditions.
117.
WHO. Annual global economic burden of alzheimer’s and other dementias.
WHO: Dementia Fact Sheet https://www.who.int/news-room/fact-sheets/detail/dementia (2019)
Global cost: $1.3 trillion (2019 WHO-commissioned study) 50% from informal caregivers (family/friends, 5 hrs/day) 74% of costs in high-income countries despite 61% of patients in LMICs $818B (2010) → $1T (2018) → $1.3T (2019) - rapid growth Note: Costs increased 35% from 2010-2015 alone. Informal care represents massive hidden economic burden Additional sources: https://www.who.int/news-room/fact-sheets/detail/dementia | https://alz-journals.onlinelibrary.wiley.com/doi/10.1002/alz.12901
.
118.
JAMA Oncology. Annual global economic burden of cancer.
JAMA Oncology: Global Cost 2020-2050 https://jamanetwork.com/journals/jamaoncology/fullarticle/2801798 (2020)
2020-2050 projection: $25.2 trillion total ($840B/year average) 2010 annual cost: $1.16 trillion (direct costs only) Recent estimate: $3 trillion/year (all costs included) Top 5 cancers: lung (15.4%), colon/rectum (10.9%), breast (7.7%), liver (6.5%), leukemia (6.3%) Note: China/US account for 45% of global burden; 75% of deaths in LMICs but only 50.0% of economic cost Additional sources: https://jamanetwork.com/journals/jamaoncology/fullarticle/2801798 | https://www.nature.com/articles/d41586-023-00634-9
.
120.
Diabetes Care. Annual global economic burden of diabetes.
Diabetes Care: Global Economic Burden https://diabetesjournals.org/care/article/41/5/963/36522/Global-Economic-Burden-of-Diabetes-in-Adults 2015: $1.3 trillion (1.8% of global GDP) 2030 projections: $2.1T-2.5T depending on scenario IDF health expenditure: $760B (2019) → $845B (2045 projected) 2/3 direct medical costs ($857B), 1/3 indirect costs (lost productivity) Note: Costs growing rapidly; expected to exceed $2T by 2030 Additional sources: https://diabetesjournals.org/care/article/41/5/963/36522/Global-Economic-Burden-of-Diabetes-in-Adults | https://doi.org/10.1016/S2213-8587(17)30097-9
.
122.
World Bank, Bureau of Economic Analysis. US GDP 2024 ($28.78 trillion).
World Bank https://data.worldbank.org/indicator/NY.GDP.MKTP.CD?locations=US (2024)
US GDP reached $28.78 trillion in 2024, representing approximately 26% of global GDP. Additional sources: https://data.worldbank.org/indicator/NY.GDP.MKTP.CD?locations=US | https://www.bea.gov/news/2024/gross-domestic-product-fourth-quarter-and-year-2024-advance-estimate
.
123.
Environmental Working Group. US farm subsidy database and analysis.
Environmental Working Group https://farm.ewg.org/ (2024)
US agricultural subsidies total approximately $30 billion annually, but create much larger economic distortions. Top 10% of farms receive 78% of subsidies, benefits concentrated in commodity crops (corn, soy, wheat, cotton), environmental damage from monoculture incentivized, and overall deadweight loss estimated at $50-120 billion annually. Additional sources: https://farm.ewg.org/ | https://www.ers.usda.gov/topics/farm-economy/farm-sector-income-finances/government-payments-the-safety-net/
.
124.
Drug Policy Alliance.
The drug war by the numbers. (2021)
Since 1971, the war on drugs has cost the United States an estimated $1 trillion in enforcement. The federal drug control budget was $41 billion in 2022. Mass incarceration costs the U.S. at least $182 billion every year, with over $450 billion spent to incarcerate individuals on drug charges in federal prisons.
125.
International Monetary Fund.
IMF fossil fuel subsidies data: 2023 update. (2023)
Globally, fossil fuel subsidies were $7 trillion in 2022 or 7.1 percent of GDP. The United States subsidies totaled $649 billion. Underpricing for local air pollution costs and climate damages are the largest contributor, accounting for about 30 percent each.
126.
Papanicolas, Irene et al. Health care spending in the united states and other high-income countries.
Papanicolas et al. https://jamanetwork.com/journals/jama/article-abstract/2674671 (2018)
The US spent approximately twice as much as other high-income countries on medical care (mean per capita: $9,892 vs $5,289), with similar utilization but much higher prices. Administrative costs accounted for 8% of US spending vs 1-3% in other countries. US spending on pharmaceuticals was $1,443 per capita vs $749 elsewhere. Despite spending more, US health outcomes are not better. Additional sources: https://jamanetwork.com/journals/jama/article-abstract/2674671
.
127.
Hsieh, C.-T. & Moretti, E. Housing constraints and spatial misallocation.
American Economic Journal: Macroeconomics https://www.aeaweb.org/articles?id=10.1257/mac.20170388 (2019)
We quantify the amount of spatial misallocation of labor across US cities and its aggregate costs. Tight land-use restrictions in high-productivity cities like New York, San Francisco, and Boston lowered aggregate US growth by 36% from 1964 to 2009. Local constraints on housing supply have had enormous effects on the national economy. Additional sources: https://www.aeaweb.org/articles?id=10.1257/mac.20170388
.
129.
Tax Foundation. Tax compliance costs the US economy $546 billion annually.
https://taxfoundation.org/data/all/federal/irs-tax-compliance-costs/ (2024)
Americans will spend over 7.9 billion hours complying with IRS tax filing and reporting requirements in 2024. This costs the economy roughly $413 billion in lost productivity. In addition, the IRS estimates that Americans spend roughly $133 billion annually in out-of-pocket costs, bringing the total compliance costs to $546 billion, or nearly 2 percent of GDP.
130.
Cook, C., Cole, G., Asaria, P., Jabbour, R. & Francis, D. P. Annual global economic burden of heart disease.
International Journal of Cardiology https://www.internationaljournalofcardiology.com/article/S0167-5273(13)02238-9/abstract (2014)
Heart failure alone: $108 billion/year (2012 global analysis, 197 countries) US CVD: $555B (2016) → projected $1.8T by 2050 LMICs total CVD loss: $3.7T cumulative (2011-2015, 5-year period) CVD is costliest disease category in most developed nations Note: No single $2.1T global figure found; estimates vary widely by scope and year Additional sources: https://www.ahajournals.org/doi/10.1161/CIR.0000000000001258
.
131.
Source: US Life Expectancy FDA Budget 1543-2019 CSV.
US life expectancy growth 1880-1960: 3.82 years per decade. (2019)
Pre-1962: 3.82 years/decade Post-1962: 1.54 years/decade Reduction: 60% decline in life expectancy growth rate Additional sources: https://ourworldindata.org/life-expectancy | https://www.mortality.org/ | https://www.cdc.gov/nchs/nvss/mortality_tables.htm
.
132.
Source: US Life Expectancy FDA Budget 1543-2019 CSV.
Post-1962 slowdown in life expectancy gains. (2019)
Pre-1962 (1880-1960): 3.82 years/decade Post-1962 (1962-2019): 1.54 years/decade Reduction: 60% decline Temporal correlation: Slowdown occurred immediately after 1962 Kefauver-Harris Amendment Additional sources: https://ourworldindata.org/life-expectancy | https://www.mortality.org/ | https://www.cdc.gov/nchs/nvss/mortality_tables.htm
.
133.
Centers for Disease Control and Prevention.
US life expectancy 2023. (2024)
US life expectancy at birth was 77.5 years in 2023 Male life expectancy: 74.8 years Female life expectancy: 80.2 years This is 6-7 years lower than peer developed nations despite higher healthcare spending Additional sources: https://www.cdc.gov/nchs/fastats/life-expectancy.htm
.
134.
US Census Bureau.
US median household income 2023. (2024)
US median household income was $77,500 in 2023 Real median household income declined 0.8% from 2022 Gini index: 0.467 (income inequality measure) Additional sources: https://www.census.gov/library/publications/2024/demo/p60-282.html
.
135.
Manuel, D. U.s. Defense spending history: 100 years of military budgets.
DaveManuel.com https://www.davemanuel.com/us-defense-spending-history-military-budget-data.php (2025)
US military spending in constant 2024 dollars: 1939 $29B (pre-WW2 baseline), 1940 $37B, 1944 $1,383B, 1945 $1,420B (peak), 1946 $674B, 1947 $176B, 1948 $117B, 2024 $886B. The post-WW2 demobilization cut spending 88% in two years (1945-1947). Current peacetime spending ($886B) is 30x the pre-WW2 baseline and 62% of peak WW2 spending, in inflation-adjusted dollars.
136.
Statista. US military budget as percentage of GDP.
Statista https://www.statista.com/statistics/262742/countries-with-the-highest-military-spending/ (2024)
U.S. military spending amounted to 3.5% of GDP in 2024. In 2024, the U.S. spent nearly $1 trillion on its military budget, equal to 3.4% of GDP. Additional sources: https://www.statista.com/statistics/262742/countries-with-the-highest-military-spending/ | https://www.sipri.org/sites/default/files/2025-04/2504_fs_milex_2024.pdf
.
137.
US Census Bureau. Number of registered or eligible voters in the u.s.
US Census Bureau https://www.census.gov/newsroom/press-releases/2025/2024-presidential-election-voting-registration-tables.html (2024)
73.6% (or 174 million people) of the citizen voting-age population was registered to vote in 2024 (Census Bureau). More than 211 million citizens were active registered voters (86.6% of citizen voting age population) according to the Election Assistance Commission. Additional sources: https://www.census.gov/newsroom/press-releases/2025/2024-presidential-election-voting-registration-tables.html | https://www.eac.gov/news/2025/06/30/us-election-assistance-commission-releases-2024-election-administration-and-voting
.
138.
U.S. Senate. Treaties.
U.S. Senate https://www.senate.gov/about/powers-procedures/treaties.htm The Constitution provides that the president ’shall have Power, by and with the Advice and Consent of the Senate, to make Treaties, provided two-thirds of the Senators present concur’ (Article II, section 2). Treaties are formal agreements with foreign nations that require two-thirds Senate approval. 67 senators (two-thirds of 100) must vote to ratify a treaty for it to take effect. Additional sources: https://www.senate.gov/about/powers-procedures/treaties.htm
.
139.
Federal Election Commission.
Statistical summary of 24-month campaign activity of the 2023-2024 election cycle. (2023)
Presidential candidates raised $2 billion; House and Senate candidates raised $3.8 billion and spent $3.7 billion; PACs raised $15.7 billion and spent $15.5 billion. Total federal campaign spending approximately $20 billion. Additional sources: https://www.fec.gov/updates/statistical-summary-of-24-month-campaign-activity-of-the-2023-2024-election-cycle/
.
140.
OpenSecrets.
Federal lobbying hit record $4.4 billion in 2024. (2024)
Total federal lobbying reached record $4.4 billion in 2024. The $150 million increase in lobbying continues an upward trend that began in 2016. Additional sources: https://www.opensecrets.org/news/2025/02/federal-lobbying-set-new-record-in-2024/
.
141.
Columbia/NBER. Odds of a single vote being decisive in a u.s. Presidential election.
Columbia/NBER: What Is the Probability Your Vote Will Make a Difference? https://sites.stat.columbia.edu/gelman/research/published/probdecisive2.pdf (2012)
National average: 1 in 60 million chance (2008 election analysis by Gelman, Silver, Edlin) Swing states (NM, VA, NH, CO): 1 in 10 million chance Non-competitive states: 34 states >1 in 100 million odds; 20 states >1 in 1 billion Washington DC: 1 in 490 billion odds Methodology: Probability state is necessary for electoral college win × probability state vote is tied Additional sources: https://sites.stat.columbia.edu/gelman/research/published/probdecisive2.pdf | https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1465-7295.2010.00272.x
.
142.
Hutchinson and Kirk.
Valley of death in drug development. (2011)
The overall failure rate of drugs that passed into Phase 1 trials to final approval is 90%. This lack of translation from promising preclinical findings to success in human trials is known as the "valley of death." Estimated 30-50% of promising compounds never proceed to Phase 2/3 trials primarily due to funding barriers rather than scientific failure. The late-stage attrition rate for oncology drugs is as high as 70% in Phase II and 59% in Phase III trials.
143.
DOT. DOT value of statistical life ($13.6M).
DOT: VSL Guidance 2024 https://www.transportation.gov/office-policy/transportation-policy/revised-departmental-guidance-on-valuation-of-a-statistical-life-in-economic-analysis (2024)
Current VSL (2024): $13.7 million (updated from $13.6M) Used in cost-benefit analyses for transportation regulations and infrastructure Methodology updated in 2013 guidance, adjusted annually for inflation and real income VSL represents aggregate willingness to pay for safety improvements that reduce fatalities by one Note: DOT has published VSL guidance periodically since 1993. Current $13.7M reflects 2024 inflation/income adjustments Additional sources: https://www.transportation.gov/office-policy/transportation-policy/revised-departmental-guidance-on-valuation-of-a-statistical-life-in-economic-analysis | https://www.transportation.gov/regulations/economic-values-used-in-analysis
.
144.
PLOS ONE. Cost per DALY for vitamin a supplementation.
PLOS ONE: Cost-effectiveness of "Golden Mustard" for Treating Vitamin A Deficiency in India (2010) https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0012046 (2010)
India: $23-$50 per DALY averted (least costly intervention, $1,000-$6,100 per death averted) Sub-Saharan Africa (2022): $220-$860 per DALY (Burkina Faso: $220, Kenya: $550, Nigeria: $860) WHO estimates for Africa: $40 per DALY for fortification, $255 for supplementation Uganda fortification: $18-$82 per DALY (oil: $18, sugar: $82) Note: Wide variation reflects differences in baseline VAD prevalence, coverage levels, and whether intervention is supplementation or fortification Additional sources: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0012046 | https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0266495
.
146.
PMC. Cost-effectiveness threshold ($50,000/QALY).
PMC https://pmc.ncbi.nlm.nih.gov/articles/PMC5193154/ The $50,000/QALY threshold is widely used in US health economics literature, originating from dialysis cost benchmarks in the 1980s. In US cost-utility analyses, 77.5% of authors use either $50,000 or $100,000 per QALY as reference points. Most successful health programs cost $3,000-10,000 per QALY. WHO-CHOICE uses GDP per capita multiples (1× GDP/capita = "very cost-effective", 3× GDP/capita = "cost-effective"), which for the US ( $70,000 GDP/capita) translates to $70,000-$210,000/QALY thresholds. Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC5193154/ | https://pmc.ncbi.nlm.nih.gov/articles/PMC9278384/
.
147.
Integrated Benefits Institute. Chronic illness workforce productivity loss.
Integrated Benefits Institute 2024 https://www.ibiweb.org/resources/chronic-conditions-in-the-us-workforce-prevalence-trends-and-productivity-impacts (2024)
78.4% of U.S. employees have at least one chronic condition (7% increase since 2021) 58% of employees report physical chronic health conditions 28% of all employees experience productivity loss due to chronic conditions Average productivity loss: $4,798 per employee per year Employees with 3+ chronic conditions miss 7.8 days annually vs 2.2 days for those without Note: 28% productivity loss translates to roughly 11 hours per week (28% of 40-hour workweek) Additional sources: https://www.ibiweb.org/resources/chronic-conditions-in-the-us-workforce-prevalence-trends-and-productivity-impacts | https://www.onemedical.com/mediacenter/study-finds-more-than-half-of-employees-are-living-with-chronic-conditions-including-1-in-3-gen-z-and-millennial-employees/ | https://debeaumont.org/news/2025/poll-the-toll-of-chronic-health-conditions-on-employees-and-workplaces/
.
148.
Peltzman, S.
An evaluation of consumer protection legislation: The 1962 drug amendments.
Journal of Political Economy 81, 1049–1091 (1973)
Foundational study quantifying the costs of the 1962 Kefauver-Harris Amendments. Peltzman estimated that the efficacy requirements reduced the flow of new drugs by 50-60% and that the costs of reduced innovation substantially exceeded the benefits of keeping ineffective drugs off the market. Concluded that the 1962 amendments resulted in net welfare losses.
149.
Wardell, W. M.
Therapeutic implications of the drug lag.
Clinical Pharmacology and Therapeutics 15, 73–96 (1974)
Documented the "drug lag" between US and UK drug approvals. Found that the UK had access to significantly more new drugs than the US, and that many effective drugs available in Europe were unavailable to American patients. Estimated beta-blockers alone could save 10,000 lives annually if approved in the US. Foundational work demonstrating the mortality cost of regulatory delay.
150.
FEE. Patients and doctors vs FDA.
FEE: Patients and Doctors vs FDA https://fee.org/articles/patients-and-doctors-vs-the-fda Dale Gieringer (1985): 21,000-120,000 lives lost per decade from FDA delay Gieringer: "Loss of life from delay alone in the hundreds of thousands" (not millions) Beta-blockers alone: William Wardell estimated "10,000 lives/year" if allowed; FDA delay 1965-1976 Sam Peltzman: Post-1962 death toll from regulatory delay "easily number in thousands per year Practolol (beta-blocker): "Could save 10,000 lives/year" (Wardell estimate) FDA allowed propranolol 1968 (3 years after Europe); for hypertension/angina not until 1978 Note: "4-10 million" figure not found in sources. Gieringer’s estimates: 21K-120K deaths per decade, "hundreds of thousands" total (not millions). Specific drug delays (beta-blockers): 100K deaths estimated Additional sources: https://fee.org/articles/patients-and-doctors-vs-the-fda | https://www.econlib.org/library/Enc/DrugLag.html | https://www.fdareview.org/issues/theory-evidence-and-examples-of-fda-harm/
.
152.
Institute for Health Metrics and Evaluation (IHME). IHME global burden of disease (2.55B DALYs, 2019).
Institute for Health Metrics and Evaluation (IHME) https://vizhub.healthdata.org/gbd-compare/ (2020)
Globally, in 2019, the total number of DALYs from all causes was 2.55 billion. Additional sources: https://vizhub.healthdata.org/gbd-compare/ | https://www.healthdata.org/research-analysis/about-gbd | https://pubmed.ncbi.nlm.nih.gov/33069326/
.
153.
WHO. 80% of cardiovascular disease is preventable.
WHO: Cardiovascular diseases (CVDs)) https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds) (2021)
As many as 80% of all heart attacks and strokes are preventable" through addressing lifestyle risk factors WHO: Most cardiovascular diseases can be prevented by addressing behavioral and environmental risk factors such as tobacco use, unhealthy diet, obesity, physical inactivity, harmful use of alcohol, and air pollution Cleveland Clinic: "90 percent of heart disease is preventable through healthier diet, regular exercise, and not smoking In 2 large cohort studies, a reduction of CVD risk of >80% and diabetes >90% were demonstrated in individuals who followed healthy lifestyle practices Only 5% of individuals follow all lifestyle factors for "ideal" cardiovascular health (American Heart Association) Additional sources: https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds) | https://world-heart-federation.org/what-we-do/prevention/ | https://newsroom.clevelandclinic.org/2021/09/29/90-percent-of-heart-disease-is-preventable-through-healthier-diet-regular-exercise-and-not-smoking | https://www.ncbi.nlm.nih.gov/pmc/articles/PMC162259/
.
154.
PMC. 30-50% of cancer is currently preventable; 90-95% has environmental/lifestyle roots.
PMC: Cancer is a Preventable Disease https://pmc.ncbi.nlm.nih.gov/articles/PMC2515569/ IARC/WHO: Environmental and lifestyle factors contribute to about 50% of the global cancer burden; expected to contribute to remaining 50% for which causes currently unknown WHO: 35% of cancer deaths worldwide are due to potentially preventable or modifiable risk factors PMC: "Only 5-10% of all cancer cases can be attributed to genetic defects, whereas the remaining 90-95% have their roots in the environment and lifestyle Breakdown: 25-30% due to tobacco, 30-35% linked to diet, 15-20% due to infections, remainder from radiation, stress, physical activity, pollutants US: 4 out of 10 cancer cases associated with preventable risk factors (tobacco/alcohol use, physical inactivity) Note: Current preventability ( 35-40%) vs. theoretical max (90-95% if all environmental/lifestyle factors addressed) Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC2515569/ | https://www.iarc.who.int/branches-env/ | https://cancerprogressreport.aacr.org/progress/cpr22-contents/cpr22-preventing-cancer-identifying-risk-factors/
.
155.
PMC. Aging reversal demonstrated in mammals using yamanaka factors.
PMC: Chemically Induced Reprogramming to Reverse Aging https://pmc.ncbi.nlm.nih.gov/articles/PMC10373966/ (2023)
Harvard/Sinclair: Loss of epigenetic information causes aging; restoring epigenome integrity reverses aging signs in mice OSK therapy (Oct4, Sox2, Klf4): Ectopic induction can restore youthful DNA methylation patterns, transcript profiles, and tissue function without erasing cellular identity Results in mice: Systemically delivered adeno-associated viruses encoding inducible OSK in 124-week-old mice extended median remaining lifespan by 109% over wild-type controls Vision restored in glaucoma mice - first successful reversal (not just halting progression) Cyclic partial reprogramming (2 days on, 5 days off) showed improvements after just 6 weeks including reduced age-related spinal curvature Human cells: Babraham Institute showed cellular reprogramming reverses epigenetic age of human skin cells by 30 years Chemical alternatives: Six chemical cocktails identified that restore youthful genome-wide transcript profile in less than a week without compromising cellular identity Note: Demonstrates biological aging is reversible, not inevitable; safety testing ongoing before human application Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC10373966/ | https://www.nature.com/articles/s41467-024-46020-5 | https://www.liebertpub.com/doi/10.1089/cell.2023.0072 | https://clinicalepigeneticsjournal.biomedcentral.com/articles/10.1186/s13148-021-01158-7
.
156.
WHO. Injuries are largely preventable events.
WHO: Injuries and Violence Fact Sheet https://www.who.int/news-room/fact-sheets/detail/injuries-and-violence WHO: "Injuries have traditionally been regarded as random, unavoidable ’accidents’. Today both unintentional and intentional injuries are viewed as largely preventable events. 4.4 million injury-related deaths annually: 3.16M unintentional, 1.25M violence-related Injuries are preventable by changing environment, individual behavior, products, social norms, legislation, and governmental/institutional policies When standardized per 100,000 population, death rate is nearly double in low/middle-income vs high-income countries (65 vs 35 per 100,000) 90% of injury-related deaths occur in low- and middle-income countries Note: 60% of accidental deaths theoretically preventable through policy, technology, and behavior change; 40% involve instantaneous trauma beyond medical intervention Additional sources: https://www.who.int/news-room/fact-sheets/detail/injuries-and-violence | https://pmc.ncbi.nlm.nih.gov/articles/PMC2912603/ | https://www.who.int/publications-detail-redirect/the-injury-chart-book-a-graphical-overview-of-the-global-burden-of-injuries
.
158.
PMC. Stem cell therapy shows promise for neurodegenerative diseases.
PMC: Regenerative Stem Cell Therapy for Neurodegenerative Diseases https://pmc.ncbi.nlm.nih.gov/articles/PMC7926761/ (2023)
R3 paradigm: Rejuvenation (restoring cell function), Regeneration (stimulating repair), Replacement (substituting lost cells) Alzheimer’s: Stanford study showed stem cell transplants reduced brain abnormalities in mice; Neural Stem Cell Therapy shown to improve cognitive function and reduce amyloid plaques Parkinson’s: Clinical trial found Neural Stem Cell Therapy significantly improved motor function and was well-tolerated ALS/Huntington’s: MSC (mesenchymal stem cell) therapy effectiveness confirmed; slows ALS progression Challenge: Clinical trials often enroll patients at advanced stages; many preclinically promising drugs ineffective in late-stage human trials Current status: Largely experimental and early clinical trial stages; researchers working to overcome delivery challenges, safety concerns, and targeting widespread neuronal damage Note: 80% theoretical max for neurodegenerative reflects early-stage intervention potential; current treatments limited ( 10% effective) Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC7926761/ | https://med.stanford.edu/news/all-news/2023/09/stem-cell-alzheimers.html | https://stemcellres.biomedcentral.com/articles/10.1186/s13287-025-04285-7
.
159.
AAF. Return on investment for vaccines.
AAF https://www.americanactionforum.org/research/vaccine-protection-and-productivity-the-economic-value-of-vaccines/ (2011)
Every $1 spent on childhood immunizations results in approximately $11 in savings (700% ROI). For low/middle-income countries: $26.1-$51.0 ROI using cost-of-illness approach, $52.2 ROI using value-of-statistical-life approach. US childhood vaccines 1994-2023 saved $540B in direct costs, $2.7T in total societal savings. Additional sources: https://www.americanactionforum.org/research/vaccine-protection-and-productivity-the-economic-value-of-vaccines/ | https://www.healthaffairs.org/doi/10.1377/hlthaff.2020.00103 | https://immunizationevidence.org/featured_issues/the-value-of-vaccines-investments-in-immunization-yield-high-returns/
.
160.
Barter, P. J. et al. Torcetrapib and cardiovascular events: The ILLUMINATE trial.
New England Journal of Medicine 357, 2109–2122 (2007)
Phase III trial of CETP inhibitor torcetrapib terminated early due to excess mortality. Of 15,067 participants, 82 deaths occurred in the torcetrapib arm vs. 51 in placebo (HR 1.58). Cardiovascular events were also significantly higher. Pfizer spent over $800 million on development before termination. Example of Phase III trial catching serious safety issues before broader approval.
161.
Doody, R. S. et al. A phase 3 trial of semagacestat for treatment of alzheimer’s disease.
New England Journal of Medicine 369, 341–350 (2013)
Phase III trial of gamma-secretase inhibitor semagacestat for Alzheimer’s disease was terminated early by Eli Lilly. Patients on treatment showed significantly WORSE cognitive outcomes than placebo, plus increased skin cancers and infections. 1,537 patients randomized. Example of Phase III trial preventing approval of a drug that would have harmed patients.
162.
McDonald, C. M. et al. A randomized placebo-controlled phase 3 trial of drisapersen in duchenne muscular dystrophy.
Neuromuscular Disorders 27, 1021–1029 (2017)
Phase III trial of drisapersen for Duchenne muscular dystrophy failed to show clinical benefit (P=0.415). FDA rejected approval in 2016 due to safety concerns including thrombocytopenia in 2% of patients, renal toxicity, and injection site reactions in 79% of patients. BioMarin discontinued development. Example of regulatory system preventing approval of ineffective drug with serious adverse effects.
163.
Graham, David (FDA) | Lancet. Vioxx cardiovascular deaths (rofecoxib).
PMC: FDA incapable of protecting against another Vioxx https://pmc.ncbi.nlm.nih.gov/articles/PMC534432/ (2007)
Graham testimony (2004): 88,000-139,000 U.S. heart attacks/strokes from Vioxx; up to 55,000 deaths (40% fatality rate) Lancet study estimate: 88,000 Americans had heart attacks from Vioxx; 38,000 died FDA memo (2004): Vioxx contributed to 27,785 heart attacks and sudden cardiac deaths (1999-2003) High-dose Vioxx: Tripled risk of heart attacks and sudden cardiac death Prescriptions: 92.8 million U.S. prescriptions 1999-2003 Withdrawn: September 30, 2004 after APPROVE trial showed cardiovascular risks Note: Vioxx case demonstrates failure of passive post-market surveillance (FAERS) to detect safety signals in time. Voluntary reporting missed cardiovascular risks for years despite millions of prescriptions Additional sources: https://pmc.ncbi.nlm.nih.gov/articles/PMC534432/ | https://www.npr.org/2007/11/10/5470430/timeline-the-rise-and-fall-of-vioxx | https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(05)67712-4/fulltext
.
164.
Sinn, M. P.
The Continuous Evidence Generation Protocol: Two-Stage Validation (RWE → Pragmatic Trials).
https://manual.warondisease.org/knowledge/appendix/dfda-spec-paper.html (2025) doi:
10.5281/zenodo.18203375 We present the Predictor Impact Score (PIS), a novel composite metric operationalizing Bradford Hill causality criteria for automated signal detection from aggregated N-of-1 observational studies. Combined with pragmatic trial confirmation (based on evidence from 108+ embedded trials), this two-stage framework would generate validated outcome labels at 44.1x lower cost than traditional Phase III trials. This enables continuous, population-scale pharmacovigilance and precision dosing recommendations.
165.
Sinn, M. P.
Ubiquitous Pragmatic Trial Impact Analysis: How to Prevent a Year of Death and Suffering for 84 Cents.
https://manual.warondisease.org/knowledge/appendix/dfda-impact-paper.html (2025) doi:
10.5281/zenodo.18243914 Only 15 diseases/year get their first treatment each year. With 6.65 thousand diseases lacking effective treatments, the backlog would take 443 years to clear. Integrating pragmatic trials into standard healthcare increases trial capacity 12.3x, cutting that timeline from 443 years to 36 years. The average untreated disease gets a treatment 212 years earlier, saving 10.7 billion deaths at $0.842 per year of healthy life saved.
166.
Sinn, M. P.
The 1% Treaty: Harnessing Greed to Eradicate Disease.
https://manual.warondisease.org/knowledge/economics/1-pct-treaty-impact.html (2025) doi:
10.5281/zenodo.18161560 6.65 thousand diseases have zero FDA-approved treatments; at current trial capacity, exploring them takes 443 years. Redirecting 1% of military spending scales capacity 12.3x, cutting the timeline to 36 years and preventing 10.7 billion deaths. At $0.00177/DALY, 50.3kx more cost-effective than the best existing interventions. Incentive Alignment Bonds make adoption politically viable.
167.
FDLI. Japan’s regenerative medicine act and conditional approval pathway.
FDLI: Japan’s Regen Med Pathways https://www.fdli.org/2019/02/global-focus-japans-regenerative-medicine-regulatory-pathways-encouraging-innovation-and-patient-access/ (2019)
Act on Safety of Regenerative Medicine (RM Act) + amended Pharmaceuticals and Medical Devices Act (PMD Act): passed Nov 2013, effective Nov 2014 Conditional and time-limited approval pathway: Obtain approval after exploratory trials demonstrate probable benefit and proven safety 7-year conditional approval period to confirm clinical benefit (e.g., using surrogate endpoints) SAKIGAKE designation (April 2015): Expedited pathway for innovative products targeting serious/life-threatening diseases without effective treatment Benefits: Prioritized consultation, accelerated review, extended re-examination period, premium pricing Examples: Terumo’s HeartSheet and Stemirac obtained conditional approval; Stemirac also SAKIGAKE-designated Additional sources: https://www.fdli.org/2019/02/global-focus-japans-regenerative-medicine-regulatory-pathways-encouraging-innovation-and-patient-access/ | https://www.insights.bio/cell-and-gene-therapy-insights/journal/article/310/Experiences-from-Japan-SAKIGAKE-Designation-System-for-Regenerative-Medical-Products | https://pmc.ncbi.nlm.nih.gov/articles/PMC6696404/
.
169.
Yong, C. S. M., Deng, J., Tan, E. W., et al. Challenges in global access to CAR-t cells: An asian perspective.
International Journal of Hematology https://pmc.ncbi.nlm.nih.gov/articles/PMC10937087/ (2024)
Reviews CAR-T cell therapy access across Asia. Japan has approved five CAR-T products under National Health Insurance: Kymriah, Yescarta, Breyanzi, Abecma, and Carvykti. All priced at 32,647,761 JPY. Japan’s high-cost medical care reimbursement system limits patient out-of-pocket costs.
172.
FDA. FDA sentinel initiative.
FDA: Sentinel Initiative https://www.fda.gov/safety/fdas-sentinel-initiative Launched: May 2008 in response to FDAAA 2007; transitioned to full system Feb 2016 Purpose: Active post-market risk identification and analysis (ARIA) for medical products Scale: World’s largest multisite distributed database for medical product safety; 128.7M members Data sources: Insurance claims, electronic health records, patient reports Privacy: Distributed data approach - data remains with owners, patient identifiers removed Structure (2019): 3 coordinating centers - Operations, Innovation, Community Building/Outreach Real-World Evidence: RWE Data Enterprise (RWE-DE) - 25.5M lives (21M commercial + 4.5M academic) 2008-2014: FDA mandated 657 studies under FDAAA authority Note: Major advancement in post-market surveillance. "Limited Transparency and Bureaucratic Constraints" may refer to challenges, but system represents significant FDA capability improvement Additional sources: https://www.fda.gov/safety/fdas-sentinel-initiative | https://pmc.ncbi.nlm.nih.gov/articles/PMC9667154/ | https://en.wikipedia.org/wiki/Sentinel_Initiative
.
174.
Institute of Medicine (US) Committee on the U.S. Physician Supply. U.s. Physician supply and requirements: Match or mismatch?
The Nation’s Physician Workforce: Options for Balancing Supply and Requirements https://www.ncbi.nlm.nih.gov/books/NBK232541/ (1996)
Historical physician workforce data: 126.6 active nonfederal M.D. physicians per 100,000 population in 1950; 127.4 in 1960; 137.4 in 1970 (DHHS 1993). At 1960 US population of 180M, this corresponds to approximately 229,000 active physicians.